INTRODUCTION
Dispensing and using antibiotics with no prescription is strongly associated with excessive antibiotic usage and this practice is common (Servia-Dopazo and Figueiras, 2018). This dispensing practice is widespread in most countries (Morgan et al. 2011). Multiple healthcare providers are involved in the general process of antibiotic dispensing with no prescription (Homedes and Ugalde, 2013; Morgan et al. 2011). According to numerous studies using fictitious customers, this practice in pharmacies is fairly common in many nations, with no obvious geographic or temporal patterns in evidence. As a result, pharmacists are frequently one of the main sources for obtaining antibiotics without a prescription in many nations. Antibiotic dispensing is a complex behavior, with intrinsic factors (e.g., sociodemographic variables, lack of knowledge, or attitudes), which are directly related to the community pharmacists’ (CPs) dispensing practice and extrinsic factors (e.g., patients’ inability to afford physician consultation, patients’ self-medication behavior, lax law enforcement, etc.), which are indirectly related to their decision to dispense antibiotics. Therefore, in developing effective interventions in the future, understanding the context regarding these determinants is needed. The purpose of this review is to pinpoint the elements that lead CPs in developing nations to dispense antibiotics without a prescription.
Given that the majority of developing countries practice the unrestricted distribution of antibiotics, the results of this review will have a significant positive impact on society. This could lead to antibiotic resistance which is one of the greatest challenges to global development and health today (WHO, 2020). The greater demand for antibiotics justifies the need for stricter regulations of antibiotic dispensing with its stringent implementation, effective counseling, and education to the public and/or CPs for its rational use. Thus, community pharmacies can apply new strategies and programs to train their pharmacists better for effective antibiotic utilization outcomes and implement or enhance regulations regarding dispensing of antibiotics. The findings of this study will constitute an important baseline that may help all future researchers, health policymakers, and professional health organizations, in developing future antibiotics guidelines to combat drug resistance issues and enhance antibiotic dispensing practices.
MATERIALS AND METHODS
The findings of this study provide a summary of the factors that influence CPs in developing countries to dispense antibiotics without a prescription. To fulfill the objectives of this review, the researchers searched for research articles on PubMed and ScienceDirect databases. In order to get results, the following search criteria were used: antibiotic OR antimicrobial AND dispense* OR “community pharmacy” AND factor* OR knowledge* OR perception*. The researchers also conducted a manual search of research articles that would fulfill the purpose of the systematic review using Google Scholar using the keywords “antibiotics,” “antibiotic dispensing,” “CPs,” and “without prescription.”
Inclusion and exclusion criteria
The review included studies that would meet the requirement in the inclusion criteria: (i) articles conducted/focused in developing countries, (ii) published in English language, (iii) contained factors associated with both intrinsic and extrinsic concerning dispensing of antibiotics without a prescription, and (iv) published in January 2000 to 2021, and (v) the population of the study included CPs. The methodological characteristics of the research articles selected are shown in Table 1.
In this review, the authors based the development classification of each country on the year when a particular study was published. Research works conducted in developed or least developed nations that did not focus on CPs’ practice of dispensing antibiotics without a prescription, did not explore the factors associated with this practice and addressed other target populations (such as nurses, doctors, dentists, and veterinarians, among others) were excluded.
Quality assessment
The following tools were used to assess the quality and bias susceptibility of the studies that were selected for inclusion: (1) the Critical Appraisal Skills Programme (CASP) quality tool for qualitative studies and (2) the Appraisal Tool for Cross-Sectional Studies (AXIS) for quantitative and mixed studies. These tools also determine whether the conclusions that were published as a result of a study were trustworthy and credible in light of its goal, procedures, and findings.
According to Long et al. (2020), the CASP tool is the most widely used tool for quality appraisal in health-related qualitative evidence synthesis. To know the validity of the study and its results, the tool contains ten questions that each focus on a different methodological aspect of a qualitative study as shown in Table 2. In relation, AXIS which was the second tool used in this review contains 20 questions that should generally appear in a study, for instance, the aim/s and objectives of the study which should be clearly stated to be able to know the extent to which the study objectives were achieved. This one important question alone could be a factor in appraising the quality of the paper; thus, the AXIS tool in the systematic interpretation of the study further allows the researcher to identify which study to be included as it contains appropriate and clearly focused questions as shown in Table 1.
All articles that included quantitative analyses complied with the majority of the AXIS tool’s questions, as indicated in Table 1 and Figure 1, and were therefore deemed suitable for the systematic review. Most studies fulfilled almost all the questions on the AXIS criterion. Furthermore, all the qualitative research articles selected passed the screening questions (questions 1 and 2 with the asterisk symbol) in the CASP tool. All the qualitative studies were included in the systematic review because the intrinsic and extrinsic factors related to the dispensing practice of CPs were present and all of them have a low susceptibility to bias since most of them fulfilled almost all of the criteria as shown in Table 2 and Figure 2.
RESULTS AND DISCUSSION
Search results, data extraction, and analysis
Figure 3 shows the detailed search results. The data were gathered from primary studies. The authors independently selected, screened, and extracted the research articles, with any disparities or disagreements being resolved by consensus.
Type of relationship and its symbol
The symbols used in Tables 3 and 4 that may help in assessing the link between the factors (intrinsic and extrinsic) and the dispensing practice of CPs are described by the terminology below in quantitative research publications.
Direct relationship. This relationship pertains to a factor that is related to an increased antibiotic without prescription. Its statistical significance is given with a p-value ≤ 0.05. In the table, it is depicted as (↑).
No relationship. This relationship pertains to a factor that tends to have no influence on the dispensing of antibiotics without a prescription. Its statistical significance is given with a p-value ≤ 0.05, depicted in the table as (≅).
No symbol. The absence of either (↑) or (≅) symbols pertains to the factor that is associated with the dispensing of antibiotics without prescription, but hypothesis testing was not conducted in the research.
Intrinsic factors
According to a study by Morgan et al. (2011), dispensing antibiotics is influenced by intrinsic factors such as sociodemographic variables, lack of knowledge, or attitudes, which directly influenced the CPs’ dispensing practice. The intrinsic factors identified were categorized into CPs’ sociodemographic characteristics and lack of knowledge/attitudes as shown in Table 3. Based on the different research articles included in the review, the following six attitudes are the common factors that were found to influence CPs’ antibiotic dispensing.
Lack of knowledge: The antibiotic dispensed by CPs is not suitable for the condition experienced by the patients. This act is a reflection of CPs’ lack of knowledge, awareness, and training.
Self-satisfaction: CPs dispense antibiotics without prescription to meet what they perceive as being their customer’s expectations.
Economic benefit: CPs’ attitude to prioritize the financial gain or profit of the pharmacy when dispensing antibiotics without prescription.Confidence: An attitude that pertains to the level of self-confidence felt by CPs in dispensing antibiotics without prescription can be associated with the knowledge and wisdom that they gained practicing the field of community pharmacy for many years.
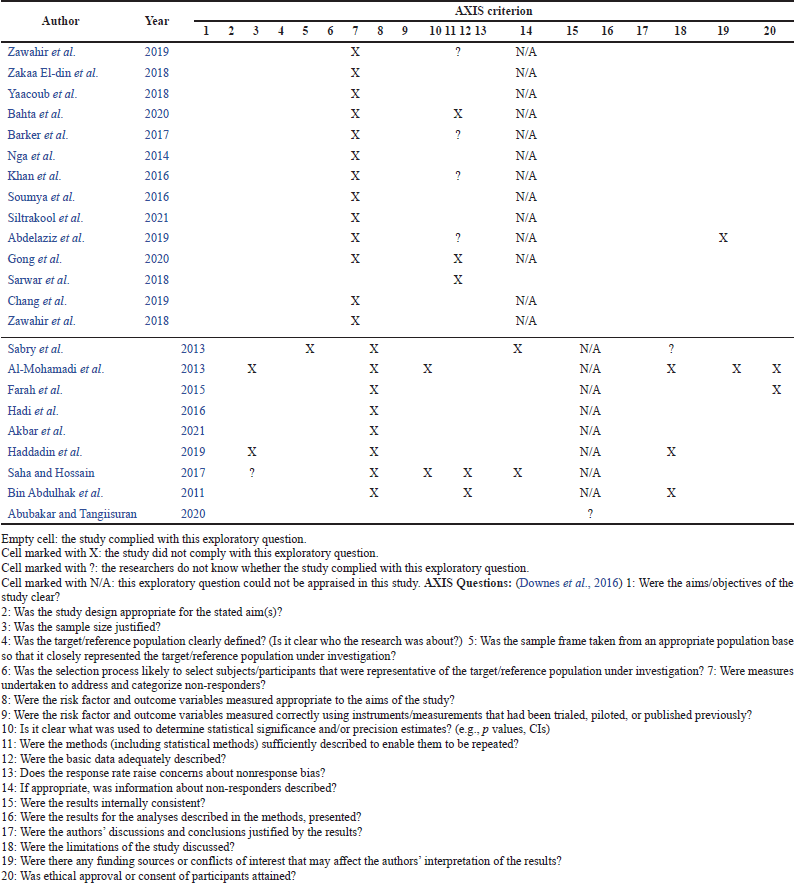 | Table 1. Study of assessment of quality and susceptibility to bias of quantitative and mixed studies: AXIS. [Click here to view] |
Empathy: An attitude that pertains to the responsibility felt by CPs to the customers which led them in dispensing antibiotics without prescription.
Fear: The attitude that reflects the fear of CPs of losing customers if they do not dispense antibiotics without a prescription.
Extrinsic factors
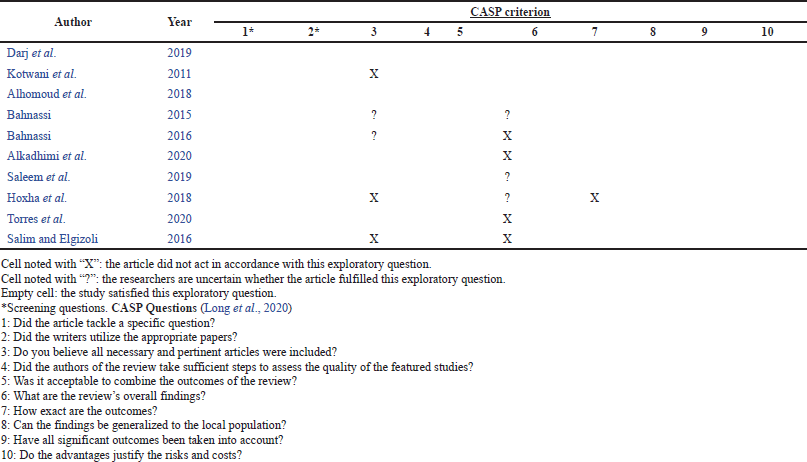 | Table 2. Quality assessment table in respect of qualitative and mixed studies: CASP. [Click here to view] |
Aside from intrinsic factors, extrinsic factors such as patients’ inability to afford physician consultation, patients’ self-medication behavior, etc., indirectly influenced CPs’ decisions in antibiotic dispensing (Morgan et al. 2011). As indicated in Table 4, the detected extrinsic factors in this review are divided into patient-related factors and other extrinsic factors. The researchers discovered nine important factors based on the various study articles they reviewed:
The inability of patients to afford physician consultation: The financial status of the patients is responsible for this factor. Compared to the health system of developed countries in the world, the health system of developing countries does not always address the needs of its constituents, despite their existing laws (e.g., Universal Healthcare Laws), and thus some marginalized patients are affected by it and few are discouraged to have a consultation with a physician due to financial constraints.
Cost of the antibiotics: Some patients in developing countries cannot afford to pay for all the antibiotics needed in their prescription; thus, they only buy the incomplete quantity of the antibiotics that their money allows. This dispensing practice is allowed in some developing countries, most notably in the Philippines, as long as the prescription is signed by the pharmacist.
High patient demand: This factor is related to pharmacists wanting to gain sales for their pharmacy because some patients would rather go to other pharmacies to obtain a particular drug without a prescription; consequently, making that particular drug in demand considering most of the pharmacies will not allow patients to obtain one without prescription and only a few will allow them to do so.
Patients’ self-medication behavior: The use of antibiotics in self-medication and dispensing of antibiotics without prescription has been a study of interest across countries. Evidence revealed that self-medication is linked to pharmacists’ antibiotic dispensing practices (Torres et al., 2020). For some pharmacists, if physicians prescribe the same antibiotics for different health conditions to different patients, physicians are influencing patients’ decisions to avoid medical services and gratify self-medication with antibiotics.
Patients lack time to consult a physician: In developing countries, there is a low physician-patient ratio (e.g., Mozambique); thus, it would take longer for one patient to get a consultation. There are also instances where the patients belong to far-flung areas which would not enable them to have the luxury of time to have a consultation with a physician even though they have resources for such.
Lack of public awareness: There is a lack of awareness among the general public regarding the rational use of antibiotics and/or antibiotic resistance which consequently encourages people to purchase antibiotics without a prescription or self-refill previous prescriptions.
Inappropriate physician prescribing: It pertains to the antibiotics prescribed by physicians not intended for the specific illness (e.g., antibiotics for viral diseases). These prescribing practices include regularly prescribing the same antibiotics for various health issues, prescribing blindly or needlessly, prescribing antibiotics quickly, and communicating poorly with patients about the prescribed antibiotic, which also contributes to patients’ self-medication behavior (Torres et al., 2020).
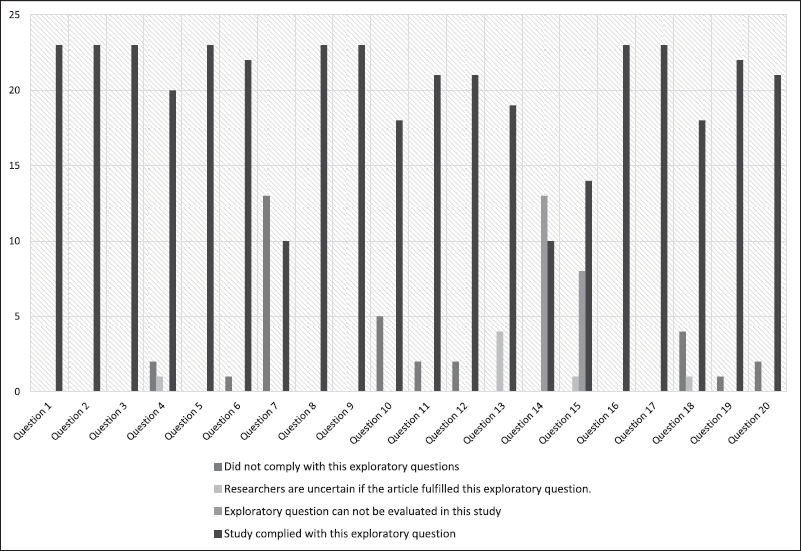 | Figure 1. Number of studies that were compliant, non-compliant, or neither with the exploratory questions by AXIS. [Click here to view] |
Incentives/profit from business owners and/or pharmaceutical companies: The unethical antibiotic dispensing within pharmacies is a result of the drive for profits coupled with aggressive marketing methods with incentives for pharmacists to enhance sales.
Lax law enforcement: In some developing countries (e.g., Lebanon, Sri Lanka, etc.), a prevalence of over-the-counter availability of antibiotics is present; this practice was widespread and common among CPs due to the poor implementation of the existing laws to control an orderly manner in the dispensation of antibiotics.
Characteristics of the selected studies
The studies selected were composed of 21 quantitative studies and 10 qualitative studies, and two were classified as mixed-type studies (studies containing quantitative and qualitative study design) as shown in Table 5.
The scope of the research articles included in the review is the following: research articles conducted/focused in developing countries, published in the English language, contained factors associated with both intrinsic (e.g., pharmacists’ lack of training, personal experience, and lack of knowledge) and extrinsic (e.g., patients’ lack of awareness, inability in relation to dispensing of antibiotics without a prescription, self-medication, and lax law enforcement regulating the dispensation of antibiotics), and published in the year 2000 to 2021, and the population of the study includes CPs.
The study population or participants in the majority of the research articles reviewed consisted of CPs. Furthermore, the research article by Zawahir et al., (2019) also included pharmacy assistants and the research article by Bahta et al. (2020) also included pharmacist technicians.
With regard to the data collection, most of the studies utilized structured questionnaires. Most studies also focused on the observation of the interaction between the community pharmacist and the patient/customer. Only the study of Kotwani et al. (2011)utilized a focus group discussion.
Factors identified that influence CPs
The factors with regard to the antibiotic dispensing of CPs without a prescription were gathered from the research articles that passed the inclusion criteria. The determined factors were then split into two main groups: intrinsic and extrinsic factors. Each research article was selected and evaluated to identify what factors have influenced CPs in dispensing antibiotics without prescription.
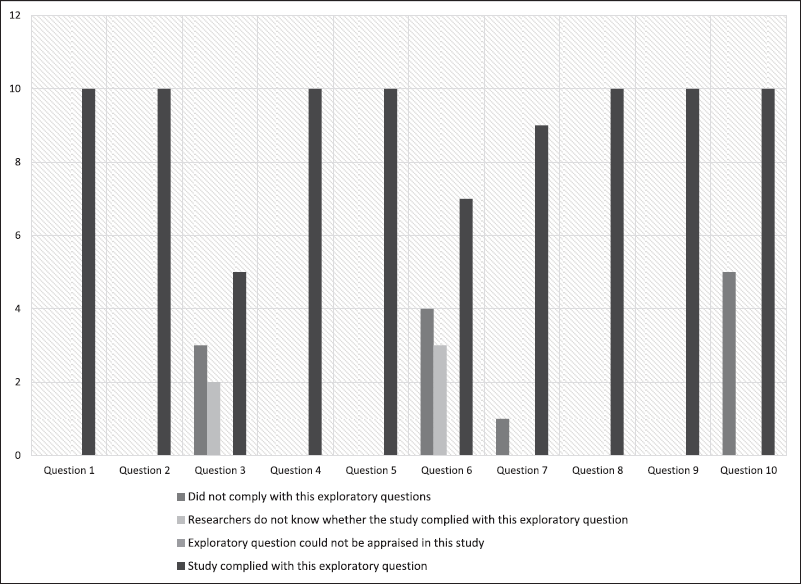 | Figure 2. Number of studies that were compliant, non-compliant, or neither with the exploratory questions by CASP. [Click here to view] |
Intrinsic factors
Socio demographic characteristics
The sociodemographic traits of CPs have been mentioned in numerous research. Twenty-one quantitative studies indicated different sociodemographic characteristics as a factor that influences antibiotic dispensing practice. Based on age, 5/21 of research articles indicated that it does not have an influence, contrary to 3/21 which indicated a statistical significance equating it as a factor to influence the dispensing of antibiotics. With regard to gender, a huge variation between different studies was observed because 7/21 quantitative studies stated that gender does not have an effect, whereas only 2/21 quantitative studies indicated that gender is a statistically significant factor that impacts their dispensing practice. With regard to pharmacists’ years of professional experience, 2/21 quantitative studies reported it to be a nonsignificant factor, whereas 6/21 indicated it as a determinant that leads to an increase in antibiotic dispensing without prescription. From the 21 quantitative studies gathered, age and gender do not have an influence on the antibiotic dispensing of CPs while years of professional experience do have an impact as shown in Figure 2.
CPs’ attitudes
CPs’ attitudes have been one of the most crucial aspects when it comes to antibiotic dispensing without prescription based on the research articles reviewed. A total of 29/33 studies evaluated these attitudes, with lack of knowledge being rated as the most common intrinsic factor. Fifteen studies did conduct hypothetical testing while six studies indicated it. Thus, the former did not have a p-value to show the association between the factor and the antibiotic dispensing of CPs, both of which demonstrated that the factor has an influence on the antibiotic dispensing of CPs, and one study reported it does not influence their antibiotic dispensing as shown in Figure 3.
Self-satisfaction was identified to be one of the intrinsic factors. Two studies have demonstrated a direct relationship between this component and the rise in the number of antibiotics obtained without a prescription. Five studies have demonstrated a mere association (no hypothesis testing was done), and one study has demonstrated no relationship at all. A study by Nga et al. (2014) indicated that patients’ demand for antibiotics affected CPs’ antibiotic dispensing practice, making them more business-oriented, and according to them, this can be changed if patients’ awareness is improved and when the knowledge of the dispensers is sufficient to provide professional advice.
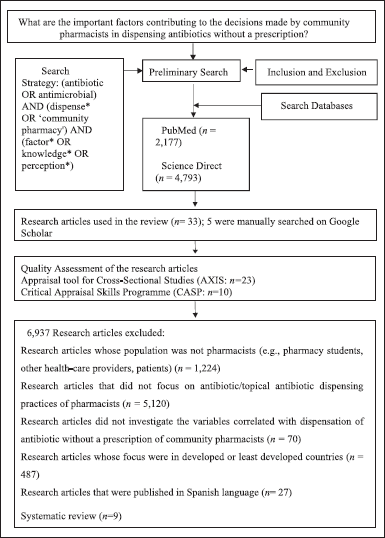 | Figure 3. Identification and inclusion of research article. [Click here to view] |
Lastly, fear (4/33) and confidence (5/33) were shown to be associated with antibiotic dispensing; however, their p-values were not stated. A study by Alhomoud et al. (2018) showed that CPs’ antibiotic dispensing is influenced by the fear that they would lose a customer since patients may go to other pharmacies to obtain antibiotics without a prescription. Thus, this would affect their pharmacy business. Moreover, pharmacists felt that they are confident, qualified, knowledgeable, and experienced in dispensing antibiotics.
Extrinsic factors
Patient-related factors
The inability of patients to afford physician consultation, the cost of the antibiotics, high patient demand, patients’ self-medication behavior, patients lacking time to consult a physician, and lack of public awareness are factors that are included in this section.
As shown in Figure 4, the top two common factors that are present in the research articles reviewed are the inability of patients to afford physician consultation (12/33) and lack of public awareness (10/33). A total of four research articles highlighted the patients’/customers’ high demand for antibiotics. A research article by Torres et al. (2020) emphasized the fact that the patients’ demand for antibiotics was related to their expectations and beliefs on the healing power of antibiotics.
The lack of time to consult a physician for a check-up was indicated in four research articles. A study by Alhomoud et al. (2018) indicated that pharmacists felt that patients prefer to visit community pharmacies rather than hospitals to obtain antibiotics due to their accessibility—visiting community pharmacies saves patients a lot of time.
Patients’ self-medication behavior was mentioned in three research articles and the univariate analysis of a study by Haddadin et al. (2019) indicated that patients’ self-medication behavior and the CPs’ years of experience (>10 years) were linked to incorrect antibiotic distribution. This association received a p-value of <0.05, which is regarded as statistically significant. According to the analyses, self-medication with antibiotics was significantly and independently linked with ineffective antibiotic dispensing (95% C, p = 0.001).
Lastly, two research articles indicated that the cost of antibiotics affects the antibiotic dispensing practice of CPs. A study by Saleem et al. (2019) indicated that socioeconomic factors are important in determining irrational practices of the community pharmacist and most of the time, the patients demand a lesser amount of antibiotics than the fully prescribed course by the physician because they cannot afford the full course.
Other extrinsic factors
The factors included in this section did not belong to any patient-related factors. The common factors read by the researchers include inappropriate physician prescribing, lax law enforcement, and incentives/profit from business owners and/or pharmaceutical companies.
Six research articles stressed inappropriate physician prescribing as a factor that contributes to the serving of antibiotics without a prescription practice of CPs. A study by Sabry et al. (2013) stated that this factor is associated with physicians’ attitudes such as complacency and fear for the patient’s health—this fear may want them use stronger medications for better health outcomes. As result, doctors prefer to use newer, costly antimicrobial agents over cost-effective or well-established, evidence-based antimicrobial agents.
As shown in Figure 5, the most notable factor in this subcategory is lax law enforcement, which is present in 22/33 research articles and most of it called for more stringent law enforcement because the existence of the law is not sufficient enough to reduce the number of obtaining antibiotics without a prescription. An investigation by Torres et al. (2011) stated that due to the lack of law enforcement and accountability mechanisms, this dispensing practice is prevalent, and the way to solve it is through compliance and accountability.
Few of the research articles (12/33) indicated that due to the result of a thirst for financial incentives/profit from business owners and/or pharmaceutical companies, CPs dispense antibiotics without a prescription. A research article by Alhomoud et al. (2018) indicated that some pharmacists are aware that dispensing antibiotics without a prescription is wrong, but they had to do it otherwise their business would be affected, as nearby pharmacies would sell antibiotics without a prescription. Furthermore, a study by Sarwar et al. (2018) stated that more studies are needed to relate the financial benefits coming from business owners or pharmaceutical companies to the current dispensing practices of CPs.
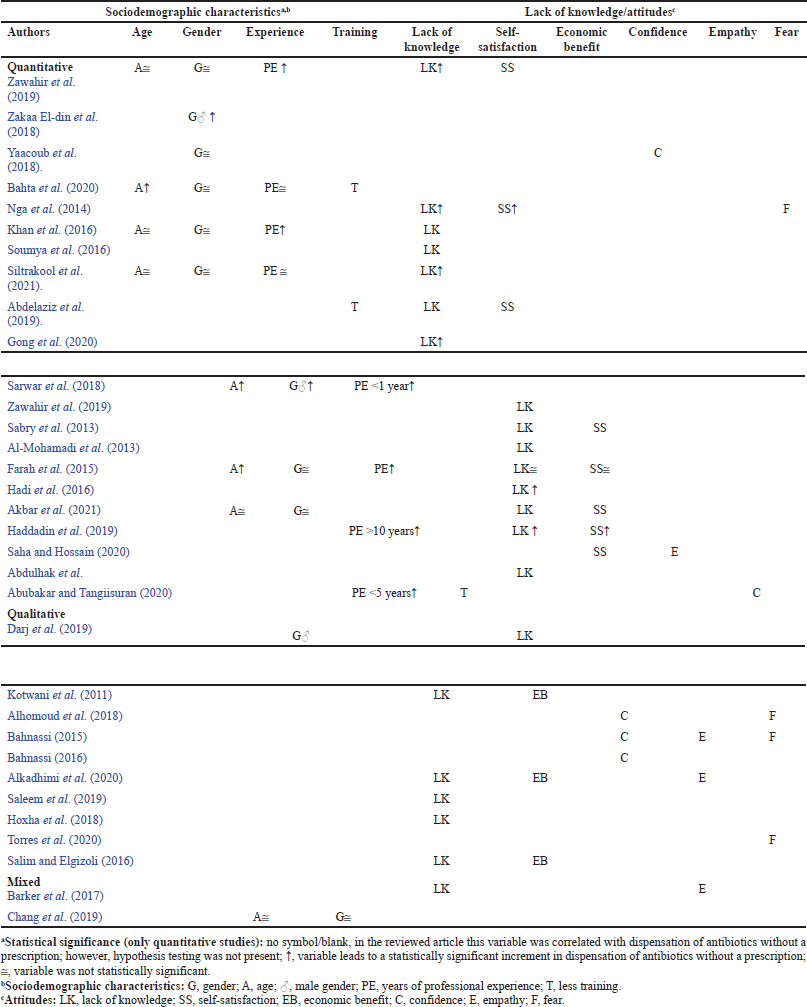 | Table 3. Intrinsic factors correlated with dispensation of antibiotics without a prescriptiona. [Click here to view] |
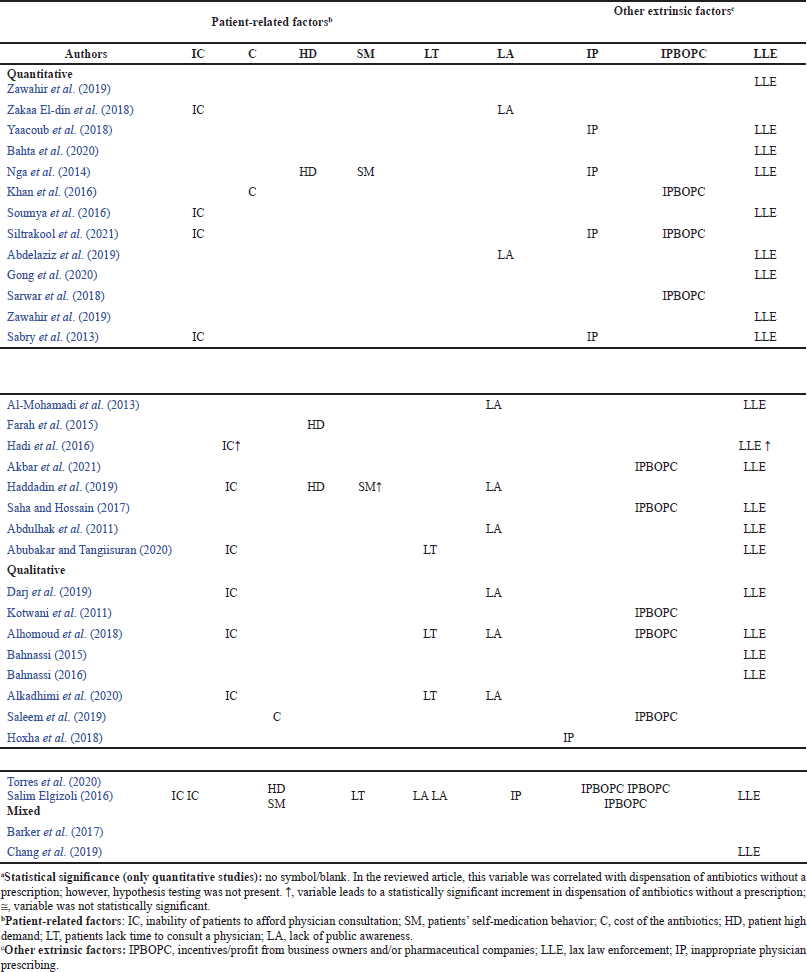 | Table 4. Extrinsic factors correlated with dispensation of antibiotics without a prescriptiona. [Click here to view] |
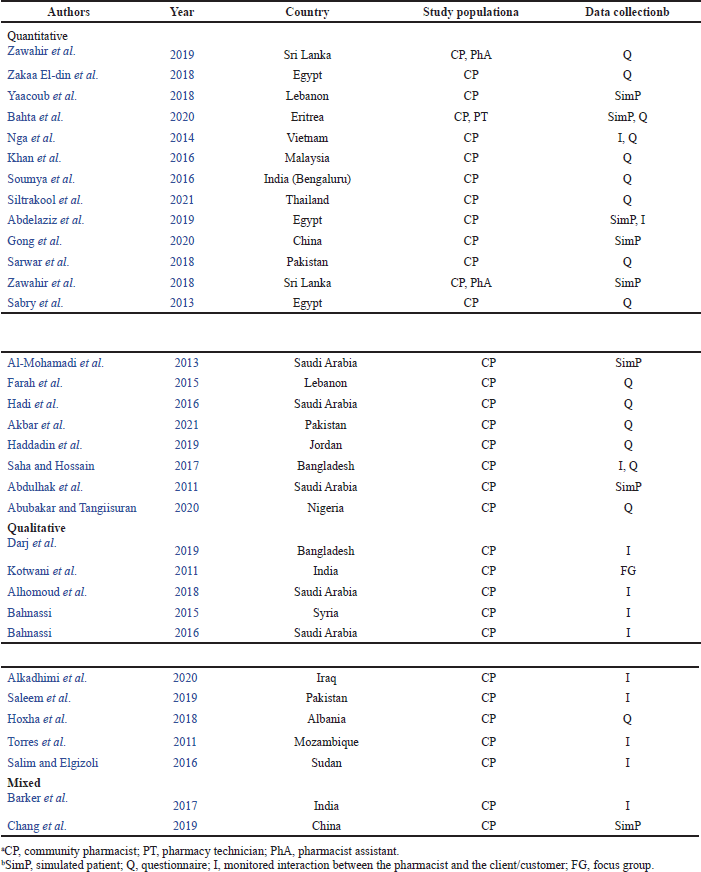 | Table 5. Characteristics of methodology of the research articles included. [Click here to view] |
Dispensing of antibiotics without prescription is one of the factors that contribute to the irrational use of antibiotics, thus increasing the risk of antimicrobial resistance (Alkaghimi et al., 2020). According to Ayukekbong et al. (2017), the causes of antimicrobial resistance in developing countries are complex and may be rooted in healthcare providers’ practices as well as patient’s behavior toward the improper usage of antimicrobials and supply chains of antimicrobials in the community. Over 50% of antimicrobials are estimated to be obtained without a prescription from community pharmacies (Cars and Nordberg, 2005).
In developing countries, dispensing antibiotics without a prescription is commonly practiced among CPs and it is determined by their attitudes. According to the CPs in the collected studies, other factors that also influence the antibiotic dispensing practice include the inability of patients to afford physician consultation, inappropriate physician prescribing, and lax law enforcement. Moreover, the sociodemographic characteristics (e.g., years of professional experience, age, gender, and training) do not seem to have an impact on dispensing without a prescription, despite the fact that some studies claimed they were a factor that contributed to a statistically significant rise in antibiotic dispensing without a prescription.
According to Kuepper (2020), developing countries are those with a low gross domestic product per capita and strongly depend on agriculture as the primary industry. In general, these countries are reliant on foreign capital and development assistance, not highly industrialized, and do not have a strong industrial base. In this systematic review, the authors based the development classification of each country on the year when a particular study was published regardless of when its categorization (developed, least developed, etc.) in the year 2021, has changed. Since the range of the year from most of the studies gathered was from 2011 to 2021, the authors utilized the World Economic Situation and Prospects report (made by the United Nations Department of Economic and Social Affairs, with inputs from the five United Nations regional commissions and United Nations Conference on Trade and Development) published in the aforementioned range of years to know if a particular country in the study selected was a part of the developing countries in the year when it was published.
The main sociodemographic factor linked with CPs’ antibiotic dispensing without prescription is their experience. The number of years of experience that CPs have is correlated with their confidence in providing antibiotics without a prescription. According to CPs, they are highly confident to dispense antibiotics since they have been dispensing these for a very long time (e.g., >10 years) (Haddandin et al., 2019). Conversely, CPs dispensing practices were also affected by a lack of experience in the field (Abdelaziz et al., 2019). According to the study of Abubakar and Tangiisuran (2020), the primary justification for CPs dispensing antibiotics without a prescription was their confidence in their knowledge of antibiotic management. Compared to those with 5 years of experience, CPs with less experience dispense antibiotics without a prescription five or more times each day. Thus, education and training in handling antibiotics among CPs could be an essential intervention (Hadi et al., 2016).
CPs’ attitudes reflect their way of dispensing antibiotics. According to Roque et al.(2013), attitudes of pharmacists toward known patients tended to be different due to the familiarity with the individual patient’s history which leads to the antibiotics being handed in later. Attitude is the major contributor to their dispensing practices along with economic benefit, self-satisfaction, confidence, empathy, and fear, which were also identified as factors that favored dispensing without prescription. These findings demonstrate a lack of knowledge and awareness of the risks associated with antibiotic resistance as well as the management of antibiotics. Thus, educational strategies or programs such as antibiotic dispensing guidelines and education seminars amongst pharmacists are essential to respond to the issue.
Many CPs expressed their fear with regard to losing customers. A study by Nga et al. (2014) stated that this factor is common among CPs because they know that customers will be able to acquire one without any prescription being presented and might as well dispense it without a prescription. This was also supported by another study which stated that pharmacists could not resist the increasing demand for antibiotics, believing that patients may acquire them from other community pharmacies (Mahmoud et al., 2018). Some CPs also justified their fear of the need to ensure the business’s survival.
Since patient-related factors, for example, may have an impact on dispensing behaviors, improving CPs’ knowledge and attitudes will not be adequate (Dillip et al., 2015; Saengcharoen et al., 2008). These factors indicate the need for the implementation of interventions through awareness campaigns and education programs that would target the whole population, especially people who lack education and poor understanding of the issue. According to the American Society of Health-System Pharmacists (2010), a pharmacist’s responsibilities for antimicrobial stewardship and infection prevention and control include the promotion and optimal antimicrobial use, reducing the transmission of infections, as well as educating other health professionals, patients, and the public.
According to studies by Salim and Elgizoli (2016) and Farah et al. (2015), clients’ poor socioeconomic status is directly associated with greater rates of dispensing without a prescription. This may be due to the fact that many individuals lack the resources to see a doctor, making pharmacies their first (and, in some cases, only) point of contact with the healthcare system (Haddadin et al., 2019). Consumer spending as measured by out-of-pocket expenditure (OOPE) represents a large share of resources spent on health in developing countries, raising concern about the accessibility of services by those patients who do not have the means to pay (Fathalla and Fathalla, 2008). In developing countries, high OOPE is on the rise due to the extent of poverty, impoverishment, and indebtedness (Mishra and Mohanty, 2019). In our review, 12/33 research articles indicated that patients cannot afford a consultation with a physician for a check-up, mostly due to financial constraints. Moreover, in this circumstance, many pharmacists acknowledge that they become more lenient with patients (Nga et al., 2014; Farah et al., 2015) and for this reason, every health strategy should specifically target this group of patients (Hadi et al., 2016; Salim and Elgizoli, 2016).
Twelve studies show that incentives/profit from business owners and/or pharmaceutical companies are factors contributing to CPs dispensing practices. A study by Siltrakool et al. (2021)stated that community pharmacies tend to be business-oriented, and their business model is based on the sales of medicines and the need to satisfy customers to maintain competitiveness. With that being said, community pharmacies are not patient-oriented and think only of the benefits they can acquire. Nevertheless, the statement aforementioned is not applicable to all drug establishments. Thus, financial incentives and business orientations of community pharmacies have been regarded as the determinants for the irrational dispensing of antibiotics (Khan et al., 2016).
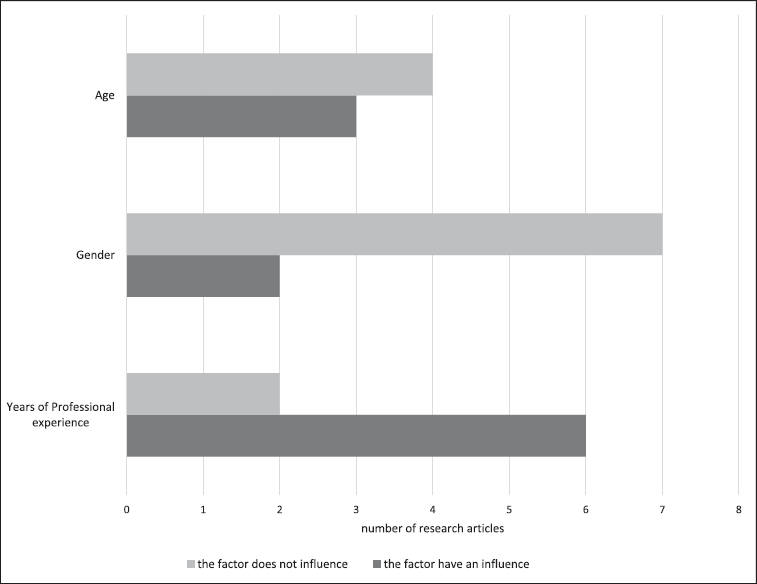 | Figure 4. Frequency of sociodemographic characteristics in the selected research articles (qualitative studies). [Click here to view] |
Developing countries have an existing legal framework that prohibits dispensing antibiotics without a prescription; however, the dispensing practice is still frequent (Belachew et al., 2021). Another critical factor is the lax law implementation which is present in almost all of the research articles reviewed as shown in Table 5; this factor is related to the lack or ineffectiveness of antibiotic policies, as well as non-compliance with them (Hadi et al., 2016; Salim and Elgizoli, 2016). Almost all research articles agree on the importance of strengthening the legal system by a stringent implementation to prevent inappropriate antibiotic dispensing. It has been demonstrated that public awareness initiatives (such as educational and support interventions) and legislative measures are both ineffective unless enforcement can be ensured (Hadi et al., 2016). The studies reviewed suggest a variety of interventions, including limiting the sales or advertising of antibiotics that provided opportunities for false information and misconceptions, vigorous law enforcement that targets pharmacists and pharmacies by prosecuting, punishing, and fining the noncompliant pharmacists, and public awareness campaigns (Alhomoud et al., 2018; Torres et al., 2020). This essentially includes stepping up and strengthening the regulation of the legislative and executive branches of government, with developed countries (e.g., New Zealand, Australia, countries in Northern Europe, and North America) serving as models (Alhomoud et al., 2013).
All of the factors aforementioned are shown to be affecting the dispensing of CPs in developing countries. These factors need to be addressed by health authorities in every country. It should be emphasized that this issue should be addressed with regard to prohibiting the sale of antibiotics since community pharmacies are frequently the initial access to health. Thus, the health infrastructure of each country should be prioritized. Furthermore, for all measures to be implemented, there should be an improvement in coordination among physicians, pharmacists, other healthcare providers, and health authorities. The importance of pharmacists’ roles should be enhanced, not only in terms of education but also in terms of patient counseling regarding the appropriate use of these antibiotics.
Finally, quantitative observational studies will need to be used to more accurately define the association between the aforementioned characteristics and CPs’ practice of supplying antibiotics without a prescription. This will enable effective interventions to be tailored to the particular factors associated with dispensing antibiotics without prescription in any given setting. Standardized tools, such as questionnaires, are crucial to achieving this goal and should be based on qualitative research that is targeted at a particular target demographic.
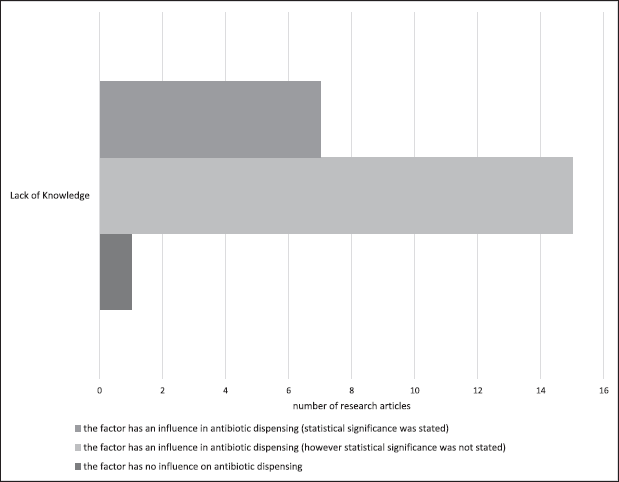 | Figure 5. Frequency of lack of knowledge on all types of studies (quantitative, qualitative, and mixed). [Click here to view] |
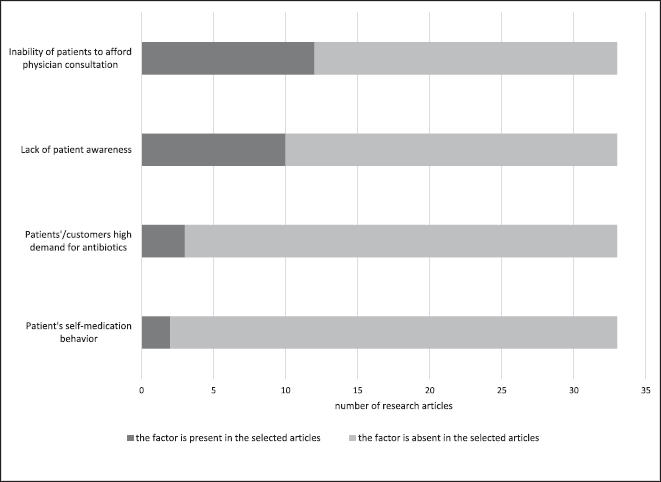 | Figure 6. Frequency of the patient-related factors in the selected research articles (quantitative, qualitative, and mixed). [Click here to view] |
As not all available databases were used to search for articles for this study, this can be a limitation. Studies published in languages other than English were also not included.
CONCLUSION
In order to combat antibiotic resistance worldwide, it is essential to take action on the intrinsic and extrinsic factors that contribute to dispensing antibiotics without prescription. Most studies in this review have indicated that lack of knowledge among CPs and lax law enforcement, from intrinsic and extrinsic factors, respectively, as the most frequent aspects associated with antibiotic dispensing without a prescription, thus, measures to be taken to counteract or reduce these determinants should be considered by the decision-makers when creating a policy to countervail the dispensation of non-OTC drugs without prescription and the pharmacists when dispensing those prescription drugs. Future interventions, despite having pharmacists’ prescription drug dispensation factors that vary in each country, should be made to remedy more than one factor. These interventions could greatly contribute to the minimization of antibiotic resistance worldwide, specifically in developing countries. Knowing the dynamics and complexities affiliated with pharmacists’ nonprescribed antibiotic dispensing and consumers’ self-medication with antibiotic practices is important for generating evidence-based facts. This would be beneficial in developing effective and experiential approaches to promoting health and raising awareness about antibiotic conservation and stewardship in the country. In addition, policymakers must adopt a top-down strategy to alleviate the profit-driven behavior of pharmacy proprietors by relieving the burden on pharmacists, bolstering good dispensing practices, and penalizing noncompliant pharmacists.
ACKNOWLEDGMENTS
The researchers express gratitude to the administrators of the Department of Pharmacy for the opportunity to conduct this study.
AUTHORS’ CONTRIBUTIONS
Gabriel Atabay thought of the study topic and planned how it will be conducted. He conducted the study including the assessment of papers to be included in this review. He wrote and edited the paper.
Teressa Esteves thought of the study topic and planned how it will be conducted. She conducted the study including the assessment of papers to be included in this review. She wrote and edited the paper.
Elizabeth Tan thought of the study topic and planned how it will be conducted. She was the third person to decide whether the paper will be included in the review or not if the two other authors’ decision is not unanimous. She revised and edited the paper.
FINANCIAL SUPPORT
There is no funding to report.
CONFLICTS OF INTEREST
The authors report no financial or any other conflicts of interest in this work.
ETHICAL APPROVALS
This study does not involve experiments on animals or human subjects.
DATA AVAILABILITY
All data generated and analyzed are included in this research article.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Abdelaziz A, Tawfik A, Rabie K, Omran M, Hussein M, Abou-Ali A, Ahmed A. Quality of community pharmacy practice in antibiotic self-medication encounters: a simulated patient study in Upper Egypt. Antibiotics, 2019; 8(2):35. CrossRef
Abubakar U, Tangiisuran B. Knowledge and practices of community harmacists towards non-prescription dispensing of antibiotics in northern Nigeria. Int J Clin Pharm, 2020; 42(2):756–64. CrossRef
Akbar Z, Saleem Z, Shaukat A, Farrukh MJ. Perception and practice of community pharmacist towards antimicrobial stewardship in Lahore, Pakistan. J Glob Antimicrob Resist, 2021; 25:157–61. CrossRef
Alhomoud F, Almahasnah R, Alhomoud FK. “You could lose when you misuse” – factors affecting over-the-counter sale of antibiotics in community pharmacies in Saudi Arabia: a qualitative study. BioMed Central, 2018; 18(1):915. CrossRef
Alkadhimi A, Dawood OT, Hassali MA. Dispensing of antibiotics in community pharmacy in Iraq: a qualitative study. Pharm Pract, 2020; 18(4):2095. CrossRef
Al-Mohamadi A, Badr A, Bin Mahfouz L, Samargandi D, Al Ahdal A. Dispensing medications without prescription at Saudi community pharmacy: extent and perception. SPJ, 2013; 21(1):13–8. CrossRef
American Society of Health System Pharmacists. ASHP statement on the pharmacist’s role in antimicrobial stewardship and infection prevention and control. Am J Health Syst Pharm, 2010; 67(7):575–7. CrossRef
Ayukekbong JA, Ntemgwa M, Atabe AN. The threat of antimicrobial resistance in developing countries: causes and control strategies. Antimicrob Resist Infect Control, 2017; 6(1):47. CrossRef
Bahta M, Tesfamariam S, Weldemariam DG, Yemane H, Tesfamariam EH, Alem T, Russom M. Dispensing of antibiotics without prescription and associated factors in drug retail outlets of Eritrea: a simulated client method. PLoS One, 2020; 15(1):e0228013. CrossRef
Barker AK, Brown K, Ahsan M, Sengupta S, Safdar N. What drives inappropriate antibiotic dispensing? A mixed-methods study of pharmacy employee perspectives in Haryana, India. BMJ Open, 2017; 7(3):e013190; doi:10.1136/bmjopen-2016-013190. CrossRef
Belachew S, Hall L, Selvey LA. Non-prescription dispensing of antibiotic agents among community drug retail outlets in Sub-Saharan African countries: a systematic review and meta-analysis. Antimicrob Resist Infect Control, 2021; 10(1):13. CrossRef
Bin Abdulhak AA, Altannir MA, Almansor MA, Almohaya MS, Onazi AS, Marei MA, Aldossary OF, Obeidat SA, Obeidat MA, Riaz MS, Tleyjeh IM. Non prescribed sale of antibiotics in Riyadh, Saudi Arabia: a cross sectional study. BMC Public Health, 2011; 11(1); doi:10.1186/1471-2458-11-538. CrossRef
Cars O, Nordberg P. Antibiotic resistance-the faceless threat. Int J Risk Saf Med, 2005; 17:103–10.
Chang J, Xu S, Zhu S, Li Z, Yu J, Zhang Y, Zu J, Fang Y, Ross-Degnan D. Assessment of non-prescription antibiotic dispensing at community pharmacies in China with simulated clients: a mixed cross-sectional and longitudinal study. Lancet Infect Dis, 2019; 19:1345–54; doi:10.1016/S1473-3099(19)30324-X. CrossRef
Darj E, Newaz MS, Zaman MH. Pharmacists’ perception of their challenges at work, focusing on antimicrobial resistance: a qualitative study from Bangladesh. Glob Health Action, 2019; 12(sup1):1735126; doi:10.1080/16549716.2020.1735126. CrossRef
Dillip A, Embrey M, Shekalaghe E, Ross-Degnan D, Vialle-Valentin C, Kimatta S, Liana J, Rutta E, Valimba R, Chalker J. What motivates antibiotic dispensing in accredited drug dispensing outlets in Tanzania? A qualitative study. Antimicrob Resist Infect Control, 2015; 4(1):30. CrossRef
Downes MJ, Brennan ML, Williams HC, Dean RS. Development of a critical appraisal tool to assess the quality of cross-sectional studies (AXIS). BMJ Open, 2016; 6(12):e011458; doi:10.1136/bmjopen-2016-011458 CrossRef
Farah R, Lahoud N, Salameh P, Saleh N. Antibiotic dispensation by Lebanese pharmacists: a comparison of higher and lower socio-economic levels. J Infect Public Health, 2015; 8(1):37–46. CrossRef
Fathalla MF, Fathalla MMF. Sexual and reproductive health: overview. In: Heggenhougen HK (ed.). International encyclopedia of public health, Elsevier, Amsterdam, The Netherlands, pp 695–705, 2008. CrossRef
Gong Y, Jiang N, Chen Z, Wang J, Zhang J, Feng J, Lu Z, Yin X. Over- the-counter antibiotic sales in community and online pharmacies, China. Bull World Health Organ, 2020; 98(7):449–57; doi:10.2471/BLT.19.242370. CrossRef
Haddadin RN, Alsous M, Wazaify M, Tahaineh L. Evaluation of antibiotic dispensing practice in community pharmacies in Jordan: a cross sectional study. PLoS One, 2019; 14(4):e0216115. CrossRef
Hadi MA, Karami NA, Al-Muwalid AS, Al-Otabi A, Al-Subahi E, Bamomen A, Mohamed M, Elrggal M. Community pharmacists’ knowledge, attitude, and practices towards dispensing antibiotics without prescription (DAwP): a cross-sectional survey in Makkah Province, Saudi Arabia. Int J Infect Dis, 2016; 47:95–100. CrossRef
Homedes N, Ugalde A. Mexican pharmacies: benefits and risks for border residents in the United States of America and Mexico. Rev Panam de Salud Pública, 2013; 33(3):196–204. CrossRef
Hoxha I, Malaj A, Kraja B, Bino S, Oluka M, Markovi?-Pekovi? V, Godman B. Are pharmacists’ good knowledge and awareness on antibiotics taken for granted? The situation in Albania and future implications across countries. J Glob Antimicrob Resist, 2018; 13:240–5; doi: 10.1016/j.jgar.2018.01.019. CrossRef
Khan MU, Hassali MA, Ahmad A, Elkalmi RM, Zaidi S, Dhingra S. Perceptions and practices of community pharmacists towards antimicrobial stewardship in the state of Selangor, Malaysia. PLoS One, 2016; 11(2):e0149623. CrossRef
Kotwani A, Wattal C, Joshi PC, Holloway K. Irrational use of antibiotics and role of the pharmacist: an insight from a qualitative study in New Delhi, India. J Clin Pharm Ther, 2011; 37(3):308–12. CrossRef
Kuepper J. What is a developing country? [document on the Internet]. The Balance, New York, NY, 2020. Available via https://www.thebalance.com/what-is-a-developing-country-1978982 (Accessed 6 January 2022)
Long HA, French DP, Brooks JM. Optimising the value of the critical appraisal skills programme (CASP) tool for quality appraisal in qualitative evidence synthesis. Res Methods Med Health Sci, 2020; 1(1):31–42; doi:10.1177/2632084320947559 CrossRef
Mahmoud MA, Aldhaeefi M, Sheikh A, Aljadhey H. Community pharmacists perspectives about reasons behind antibiotics dispensing without prescription: a qualitative study. Biomed Res, 2018; 29(21):3792–6. CrossRef
Mishra S, Mohanty SK. Out-of-pocket expenditure and distress financing on institutional delivery in India. Int J Equity Health, 2019; 18(1):99. CrossRef
Morgan DJ, Okeke IN, Laxminarayan R, Perencevich EN, Weisenberg S. Non-prescription antimicrobial use worldwide: a systematic review. Lancet Infect Dis, 2011; 11(9):692–701. CrossRef
Nga DT, Chuc NT, Hoa NP, Hoa NQ, Nguyen NT, Loan H, Toan T, Phuc H, Horby P, Yen P, Kinh N, Wertheim H. Antibiotic sales in rural and urban pharmacies in northern Vietnam: an observational study. BMC Pharmacol Toxicol, 2014; 15(1):6. CrossRef
Roque F, Soares S, Breitenfeld L, López-Durán A, Figueiras A, Herdeiro MT. Attitudes of community pharmacists to antibiotic dispensing and microbial resistance: a qualitative study in Portugal. Int J Clin Pharm, 2013; 35(3):417–24. CrossRef
Sabry NA, Farid SF, Dawoud DM. Antibiotic dispensing in Egyptian community pharmacies: an observational study. Res Soc Adm Pharm, 2014; 10(1):168–84; doi: 10.1016/j.sapharm.2013.03.004. CrossRef
Saengcharoen W, Chongsuvivatwong V, Lerkiatbundit S, Wongpoowarak P. Factors influencing dispensing of antibiotics for upper respiratory infections among southern Thai community pharmacists. J Clin Pharm Ther, 2008; 33(2):123–9. CrossRef
Saha S, Hossain MT. Evaluation of medicines dispensing pattern of private pharmacies in Rajshahi, Bangladesh. BMC Health Services Res, 2017; 17(1):136; doi:10.1186/s12913-017-2072-z. CrossRef
Saleem Z, Hassali MA, Hashmi FK, Godman B, Saleem F. Antimicrobial dispensing practices and determinants of antimicrobial resistance: a qualitative study among community pharmacists in Pakistan. Fam Med Community Health, 2019; 7(3):e000138; doi:10.1136/fmch-2019-000138. CrossRef
Sarwar MR, Saqib A, Iftikhar S, Sadiq T. Knowledge of community pharmacists about antibiotics, and their perceptions and practices regarding antimicrobial stewardship: a cross-sectional study in Punjab, Pakistan. Infect Drug Resist, 2018; 11:133–45; doi:10.2147/IDR.S148102. CrossRef
Salim AMA, Elgizoli B. Exploring the reasons why pharmacists dispense antibiotics without prescriptions in Khartoum state, Sudan. Int J Pharm Pract, 2016; 25(1):59–65. CrossRef
Servia-Dopazo M, Figueiras A. Determinants of antibiotic dispensing without prescription: a systematic review. J Antimicrob Chemother, 2018; 73(12):3244–53. CrossRef
Siltrakool B, Berrou I, Griffiths D, Alghamdi S. Antibiotics’ use in Thailand: community pharmacists’ knowledge, attitudes and practices. Antibiotics, 2021; 10(2):137. CrossRef
Soumya R, Devarashetty V, Jayanthi CR, Sushma M. Drug dispensing practices at pharmacies in Bengaluru: a cross-sectional study. Indian J Pharmacol, 2016; 48(4):360–4; doi:10.4103/0253-7613.186204. CrossRef
Torres NF, Solomon VP, Middleton LE. Identifying the commonly used antibiotics for self-medication in urban Mozambique: a qualitative study. BMJ Open, 2020; 10(12):e041323. CrossRef
World Health Organization. Antibiotic resistance. 2022 Available via https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance (Accessed 21 January 2021)
Yaacoub SG, Lahoud NA, Francis NJ, Rahme DW, Murr TH, Maison PF, Saleh NG. Antibiotic prescribing rate in lebanese community pharmacies: a nationwide patient-simulated study of acute bacterial rhinosinusitis. J Epidemiol Glob Health, 2019; 9(1):44–9; doi:10.2991/jegh.k.190305.001. CrossRef
Zakaa El-Din M, Samy F, Mohamed A, Hamdy F, Yasser S, Ehab M. Egyptian community pharmacists’ attitudes and practices towards antibiotic dispensing and antibiotic resistance; a cross-sectional survey in Greater Cairo. Curr Med Res Opin, 2019; 35(6):939–46; doi:10.1080/03007995.2018.1544119. CrossRef
Zawahir S, Lekamwasam S, Aslani P. A cross-sectional national survey of community pharmacy staff: knowledge and antibiotic provision. PLoS One, 2019; 14(4):e0215484. CrossRef