INTRODUCTION
The World Health Organization considered the concept of “vaccine hesitancy” as “one of the top-ten threats to global health” (Godlee, 2019). The utility of vaccine campaigns to prevent COVID-19 is not merely dependent on vaccine efficacy and safety. The acceptance of the vaccine among the people and healthcare workers appears to have a critical role in the successful control of the pandemic. Vaccine hesitancy is still a barrier to full inoculation of the population against highly infectious diseases (Sallam, 2021; Soleimanpour and Yaghoubi, 2021).
There are many reasons people may refuse COVID-19 vaccines. These reasons include apprehension regarding the rapid global development of COVID-19 vaccines, which raises concerns about their safety, that is, thinking a vaccine which is produced in a short period is too dangerous (Wibawa, 2021). Others consider that the nature of COVID-19 is harmless so there is no need to use the vaccine. These are in addition to doubts about the efficacy of the vaccine, the belief to be already immunized, and mistrust of healthcare especially among minorities and those with lower levels of knowledge (Dror et al., 2020; Khubchandani et al., 2021; Kimura et al., 2007; Robertson et al., 2021; Troiano and Nardi, 2021).
As a consequence, interventional educational campaigns targeted toward populations at risk of vaccine hesitancy are urgently needed to avoid low inoculation rates and combat misinformation so as to increase vaccination rates. Also, because the vaccine agreement remains inconsistent and variable, widespread public educational campaigns will be required for successful inoculation against COVID-19 regarding vaccine efficacy and safety (Dror et al., 2020; Harrison and Wu, 2020). Policy and educational-level interventions that are evidence based must be implemented to address vaccine hesitancy and encourage COVID-19 immunization programs. The rates of willingness to be vaccinated might change now assuming the accessibility of the vaccines and their long-term effects will increase the uptake of COVID-19 vaccines (Barello et al., 2020; Khubchandani et al., 2021).
Pharmacists, as healthcare providers, must act to inform, educate, and intervene to increase COVID-19 vaccine acceptance rates in the entire population (Petrelli et al., 2019). While the decision to receive the vaccination is a patient’s choice, pharmacists have the main responsibility of educating patients so that they can make informed choices, carefully weighing the benefits versus risks of vaccination (Lisenby et al., 2021). Students are a good target for educational campaigns as they are open to changing their habits. Educational interventions are the preferred strategy to improve students’ attitude, adherence, and knowledge about vaccinations, and this is demonstrated by a lot of evidence (Afonso et al., 2014; Babcock et al., 2010; Marotta et al., 2017).
Pharmacy students should be taught about vaccination and how to give the vaccines in order to administer them to children and adults in community pharmacies and to improve workforce capability when they become future healthcare providers. They should be more actively involved in counteracting vaccine hesitancy, as immunization programs are only successful when there are high rates of coverage and acceptance. Thus, the aim of this study is to evaluate the impact of an educational workshop on counteracting hesitancy toward the COVID-19 vaccine among pharmacy students in Jordan.
METHODS
Study design and participants
This study is a pre-post interventional study that was conducted during April 2021. During the study period, a convenient sample of pharmacy students was invited to participate in this study. The inclusion criteria were third- to sixth-year pharmacy students. Students were invited via an announcement that had been distributed through various social media platforms to register in the educational workshop, namely, via pharmacy students’ Facebook group, which was created to ease communication amongst the students themselves and with their academic teachers. A WhatsApp group was created for the purpose of the study research, and then a link was sent to participants via Facebook in order to enable them to join this group automatically upon clicking on the link. An ethical approval form was obtained from the International Review Board at the Deanship of Academic Research at The University of Jordan (Reference No. 69/2021). The study was conducted following the ethical standards outlined in the World Medical Association Declaration of Helsinki guideline (WMA 2014). Electronic consents were obtained from all students, and they were informed that their participation would be voluntary. Students’ data were kept confidential. No compensation was offered to participate in the study.
Sample size calculations
Sample size was calculated after consideration of a predetermined level of significance (α) of 0.05, power, and power (1−β) of 80%, which indicated the probability of detecting true relationships among variables. Sample size was calculated using G.Power 3.1®. The total sample size that was required for the study was 200 students (Vyas et al., 2018). A 20% overrecruitment to allow for any dropouts was done.
Study tool
The study survey was developed following an extensive literature review (Abu-Farha et al., 2021; Biasio et al., 2021; Dybsand et al., 2019). Thereafter, the authors added some changes and additional questions to properly assess the objectives above. A test survey was sent to other experts in the field to assess questions prior to sending the survey to participants. A study questionnaire was designed to collect the following information: 1) demographics (age, gender, current city of residence, name of the university, academic year, and GPA); 2) students’ experience with COVID-19 infection; 3) students’ willingness to take the COVID-19 vaccine; 4) students’ perceptions of COVID-19 vaccines, and 5) students’ knowledge about COVID-19 vaccines.
Educational workshop material
The educational session included information about COVID-19 vaccines such as what the COVID-19 vaccines are, how they work, types and examples of them, their safety, their side effects, and what the consequence of taking the vaccine is, for whom COVID-19 vaccines are contraindicated, what the process of creating and approving a new COVID-19 vaccine is, and what the reasons for quick development of the vaccines are and discussion about COVID-19: what it is, signs and symptoms of this disease, severity of COVID-19, and how to manage it.
Educational workshop and data collection
Before the educational workshop, the online survey was created using Google Forms®, and then, it was sent to students by WhatsApp to assess their experience, knowledge, perception, willingness, and hesitancy toward COVID-19 vaccines and the associated reasons. As of April 9, 2021, the educational workshop about COVID-19 vaccines was conducted where information was provided about vaccines’ mechanism of action, constituents, efficacy and safety, side effects, contraindication, and types of vaccines that are available in Jordan. The session lasted for 90 minutes, and due to the pandemic restrictions, it was delivered to the students by the Zoom videoconferencing application (Zoom Video Communications Inc., 2016). After the education session, students’ willingness, knowledge, and perception of COVID-19 vaccines were revaluated as well as an appraisal of the education they had received on vaccinations, in addition to questions about their satisfaction with the workshop. Each survey took 5–10 minutes to answer by the students.
Statistical analysis
Data were analyzed using the Statistical Package for Social Sciences (SPSS) version 25 (SPSS Inc., Chicago, IL). The descriptive analysis was done using the median and interquartile range (IQR) for continuous variables and frequency (percentage) for categorical variables. To ascertain whether the educational workshop had an impact on students’ knowledge, awareness, and willingness to take the COVID-19 vaccine, the McNemar test was performed. p values of ≤ 0.05 were considered to be statistically significant.
RESULTS
Demographic characteristics of the study sample
Out of 150 recruited participants, 100 students completed both surveys (completion rate 66.7%). The baseline demographic characteristics of the study participants are summarized in Table 1. The mean age of the participants was 22 years (IQR = 2.0), with the majority being female (n = 81, 81%), affiliated with private universities (n = 84, 84%), and residing in Amman (n =73, 73%). Around half of the students did not have medical insurance (n = 55, 55%). Lastly, most of the participants (n = 65, 65%) had not received the seasonal influenza vaccine previously.
Students’ experience with COVID-19
As depicted in Table 2, around one-third of the students (n = 34, 34%) revealed that they had been infected with COVID-19, with only 16 students of them (47.1%) reporting to be completely committed to quarantine during their period of infection. The majority of infected students (n = 33, 97.1%) reported that they had informed their relatives and friends when they got infected with COVID-19. The median score of their fear of COVID-19 when they knew that they got infected or suspected to have the infection was 6 out of 10 (IQR = 2). Moreover, most of the students (n = 92, 92%) reported knowing someone infected with COVID-19, and half of them (n = 50, 50%) knew someone who died of COVID-19.
 | Table 1. Baseline demographic characteristics of the study participants (n = 100). [Click here to view] |
Impact of the education workshop on improving students’ willingness to take COVID-19 vaccine
Figure 1 shows the impact of the educational workshop on improving students’ willingness to take the COVID-19 vaccine. Following the workshop, the proportion of study participants who were willing to take the COVID-19 vaccine if it is available significantly increased from 68% (n = 68) to 95% (n = 95), p < 0.001. In addition, the percentage of students who were willing to take the COVID-19 vaccine if it is recommended by their universities significantly increased from 78% (n = 78) to 97% (n = 97), p < 0.001.
Impact of the education workshop on improving students’ knowledge about COVID-19 vaccines
All the participating students answered 15 questions regarding COVID-19 vaccines before and after the workshop, and the results are presented in Table 3. After the educational workshop, an improvement in students’ knowledge was noted clearly. In comparison to 78% of the respondent (n = 78) that knew the most common side effect of the COVID-19 vaccine is fever, this percentage improved significantly to 90% (n = 90) after the workshop (p value = 0.004). Moreover, 78% of the students (n = 78) knew that the COVID-19 vaccine is given via the intramuscular route of administration, compared to 92% (n = 92) following the workshop (p value = 0.004). In addition, 59% of the respondents (n = 59) realized that there was no effective medicine available for treating COVID-19; this percentage significantly improved after the workshop (n = 71, 71%) (p value = 0.029). Before the workshop, 40% of the students (n = 40) knew that AstraZeneca is an example of a viral vector vaccine, and this percentage improved significantly to 55% (n = 55) after the workshop (p value = 0.032). Finally, participants showed an enhancement in their awareness that the COVID-19 vaccine is not safe for children, where the percentage improved from 60% (n = 60) before the workshop to 77% (n = 77) following the workshop (p value = 0.006). For the overall knowledge score (out of 15), the overall median knowledge score was improved from 11 (IQR = 3) pre-workshop to a median of 12 (IQR = 3.75) post-workshop (p value < 0.001).
Impact of the workshop on improving students’ perception towards COVID-19 vaccines
Around half of the respondents showed a positive perception of the vaccines before and after intervention with significant changes in their responses after the intervention (Table 4, p value < 0.05). Among the study participants, 76% (n = 76) of them agreed and strongly agreed that the COVID-19 vaccine is a safe and reliable way to stop the spread of the pandemic, which increased to 98% (n = 98) after the workshop (p value < 0.001). Moreover, 73% of the participants (n = 73) believed that they are responsible for advocating the benefit of vaccines and educating the public on the diseases, and this percentage increased to 90% (n = 90) after the workshop (p value < 0.001). On the other hand, pre-workshop, 45% of the study sample thought that COVID-19 vaccines were developed in a very short period of time so they might be associated with serious side effects, which declined to 29% (n = 29) after the workshop (p value = 0.020).
Students’ satisfaction with the training workshop
All participants responded to eight statements with the aim of evaluating their satisfaction with the training workshop (Table 5). The majority of the students (n = 96, 96%) agreed that the workshop helped them learn and helped them understand the vaccine development process and to understand the importance of immunization. The respondents strongly agreed/agreed that the educational workshop would help them practice what they learned at their practice sites (n = 94, 94%).
 | Table 2. Students’ experience about COVID-19 (n = 100). [Click here to view] |
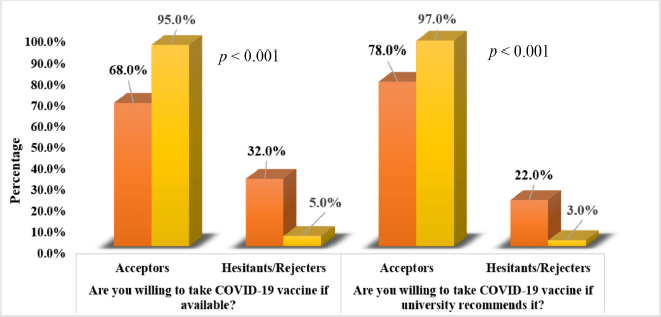 | Figure 1. Impact of educational workshop on improving students’ willingness to take COVID-19 vaccine (n= 100). p values were calculated using the McNemar test. [Click here to view] |
DISCUSSION
Managing vaccine hesitancy is complex, and there is no single intervention that can address this issue entirely, especially in the context of COVID-19 where evidence for effective strategies to address it is currently limited (Razai et al., 2021). One of these strategies is educating people to increase vaccination uptake by using different educational methods (e.g., workshops and brochures). This study assessed the benefits of utilizing an educational workshop in increasing the acceptance of COVID-19 vaccines and counteracting vaccine hesitancy in pharmacy students. In addition, it examined the impact of this workshop on the knowledge of the perception of these vaccines. As far as our knowledge goes, this study was the first study that evaluated these aspects through using an educational workshop.
Our study showed a significant improvement in pharmacy students’ knowledge of COVID-19 vaccines after the educational workshop (p value < 0.001). Krawczyk et al. (2012) had similar findings to ours, but the educational intervention was about the human papillomavirus (HPV) vaccine. They reported significantly higher knowledge in the intervention group compared to the control group following the education session (P value < 0.05) (Krawczyk et al., 2012). Moreover, Awadh et al. (2014) studied the effect of educational intervention that is prepared by experts from the school of pharmacy in Malaysia on improving parents’ knowledge of childhood immunization (infant vaccine schedule). The result showed that parents’ knowledge increased significantly after the intervention compared to the baseline result (p value < 0.001) (Awadh et al., 2014). Sitaresmi et al. (2020) also evaluated the effect of structured educational intervention on improving parents’ knowledge and awareness of the human papillomavirus vaccination. They revealed that parents’ knowledge and awareness significantly improved following the intervention (Sitaresmi et al., 2020). However, the effect of the educational program of this current study showed some negative effects on students’ knowledge of the safety of COVID-19 vaccines on pregnant women and breastfeeding women (P values 0.029 and 0.121), respectively. This could be a result of the absence of clear evidence of the safety of the vaccine in these situations at the time of giving the lecture, which could have been misinterpreted by the students as a lack of efficacy/safety.
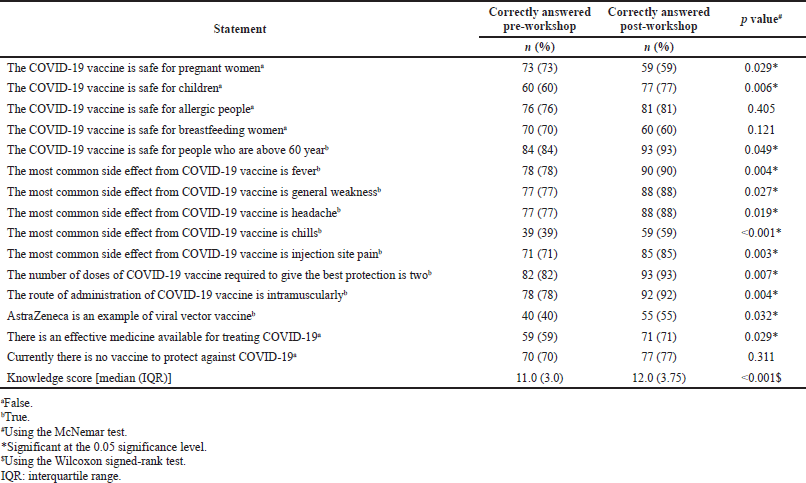 | Table 3. Students’ knowledge about COVID-19 vaccine (n = 100). [Click here to view] |
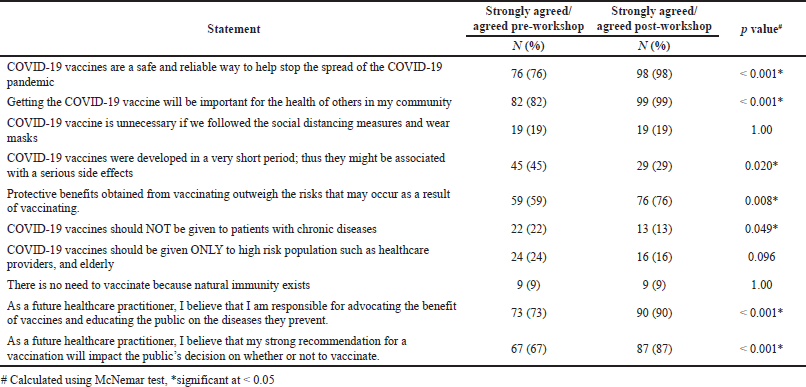 | Table 4. Students’ perception toward COVID-19 vaccine (n = 100). [Click here to view] |
 | Table 5. Students’ satisfaction with the training workshop (n = 100). [Click here to view] |
On the other hand, our findings showed strong improvement in the participants’ perception of COVID-19 vaccines after the educational session, indicating that this educational workshop was very useful and efficient in combating negative attitudes toward the various COVID-19 vaccines. Numerous previous studies elucidated the improvement in participants’ perception after conducting educational intervention (Blanchard et al., 2019; Sitaresmi et al., 2020). A similar finding was reported in a Canadian study which evaluated the effect of an interactive education session on the perceptions toward polio, measles, rubella, and pertussis vaccines. They reported that students’ perception of vaccines’ safety improved significantly after delivering the education session (Blanchard et al., 2019). Moreover, our results are similar to that observed by Sitaresm et al. (2017), which evaluated the effect of structured educational intervention on various aspects including the perception of the HPV vaccine. The study showed that there was a significant improvement in parents’ perception of the HPV vaccine (Sitaresmi et al., 2020) Findings of our study were also consistent with Madlon-Kay and Smith (2020), which evaluated the effect of an educational session on medical interpreters’ perception about childhood vaccines, it concluded that interpreters were less likely to perceive those vaccines causes autism (p-value = 0.020) but they were significantly more likely to perceive that children get too many vaccines after the presentation that is provided by authors themselves (Madlon-Kay and Smith, 2020).
Regarding the willingness to take COVID-19 vaccines, our results showed that the educational intervention significantly raised students’ willingness to get the vaccine (p value < 0.001) and thus had decreased vaccine hesitancy or refusal. Similar studies have been conducted with comparable results but with other types of vaccines. Gowda et al. (2011) studied the effect of individually tailored education for the measles, mumps, and rubella (MMR) vaccine provided to hesitant parents of children less than six years old on MMR uptake vaccination intention. The main findings of this study showed that parents who received tailored education had better positive vaccination intention than those who did not get the educational information (58% vs. 46%, respectively), and parents in the intervention group had a greater magnitude of change in vaccination intention than participants in the control group (Gowda et al., 2013). Butteri et al. (2010) also reported that the healthcare worker (HCW) acceptance rate of the influenza vaccine increased from 65% to 73% after an education program which was provided by registered nurses and medical doctors for 15 min (Butteri et al., 2010).
Although our study is the first of its kind, it has some limitations, where there was no long-term follow-up period after the workshop to reassess the knowledge, perception, and willingness to take COVID-19 vaccines due to recruitment difficulties. Regarding the sample size, we acknowledge this limitation, but this is an inherent limitation of studies that involve educational workshops; recruiting students and maintaining their interest was very difficult, especially the fact it was offered online during COVID-19 quarantine restrictions. However, it involved students from different universities in Jordan. The significance of this study is that it was the first and only intervention study to evaluate the effect of pharmacist-led education on the rate of vaccine acceptance at that time of the pandemic when rejection rates were high in the region.
Therefore, this study highlights the importance of incorporating topics about vaccines in the curricula of pharmacy programs in Jordanian universities, so as to increase their knowledge and enhance their attitudes toward relevant topics.
CONCLUSION
An educational workshop about the COVID-19 vaccine significantly improved students’ knowledge, perception, and willingness to take the vaccine by pharmacy students. Pharmacy students as future healthcare providers can play an essential role in counteracting vaccine hesitancy and increasing COVID-19 vaccine acceptance. Performing similar studies with a larger sample size, longer follow-up, and more sessions of education to assess the effect of educational workshops on the willingness of COVID-19 vaccine uptake is therefore recommended.
ACKNOWLEDGMENTS
The authors would like to thank all the pharmacy students who participated in this workshop.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
FUNDING
There is no funding to report.
ETHICAL APPROVALS
The ethical approval was obtained from the Institutional Review Board at the Deanship of Academic Research at The University of Jordan (Reference No. 69/2021).