INTRODUCTION
Despite the fact that the prevalence of human immunodeficiency virus (HIV) infection has gradually decreased over the course of this epidemic, significant challenges remain (WHO, 2021a, 2021b). In 2020, there were approximately 1.5 million new HIV infections worldwide (UNAIDS, 2021). Young adults (aged 15–24) accounted for the highest proportion (47%) of new infections in Thailand, which has one of the highest HIV burdens in Southeast Asia (HIV and AIDs Data Hub for Asia Pacific, 2019). On the other hand, HIV incidence and AIDS deaths were declining as antiretroviral therapy became more widely available (UNAIDS, 2021). However, considering the HIV/AIDS epidemic is a public health threat that is difficult to eradicate, reducing new HIV infections in society is a significant challenge. Several preventive strategies have been implemented to assist the world in meeting its HIV/AIDS targets (UNAIDS, 2021; WHO, 2020).
Pre-exposure prophylaxis (PrEP) is an HIV medication regimen that HIV-negative people use to protect themselves from infection (WHO, 2021b). Numerous clinical trials have shown that PrEP and post-exposure prophylaxis are effective at reducing the risk of HIV transmission (Thailand’s Ministry of Public Health, 2021; WHO, 2021b). Thailand has recently begun to scale up PrEP pilot projects within the national health system to prevent HIV in high-burden provinces among key higher-risk groups. Thailand’s Ministry of Public Health (2018) is also in the process of incorporating PrEP as a benefit into the country’s universal health coverage. According to the project, PrEP accessibility and use have increased significantly.
According to research on PrEP awareness in high-risk HIV-infected groups such as men who have sex with men (MSM), this group has a high level of awareness (Frankis et al., 2016; García and Harris, 2017; Iniesta et al., 2019; Werner et al., 2018; Yang et al., 2013). According to a review of recent studies, PrEP awareness among young adults ranges from 18.8% to 50.2%. While studies show that young adults are willing to use PrEP, a lack of public education about its availability, discomfort discussing sexual health with a healthcare provider, and a high level of risky sexual behavior all act as barriers to accessing PrEP (Ajayi et al., 2018, 2019; Okeke et al., 2021; Shamu et al., 2021; Taggart et al., 2020). To the best of our knowledge, there is only one report in Thailand on PrEP awareness and acceptance among MSM and transgender people (Yang et al., 2013). There is a research gap in the young adult population, which accounts for the vast majority of new HIV infections. It is critical to assess PrEP awareness, knowledge, and acceptability as population-based health services. Identifying sociodemographic and clinical predictors of PrEP acceptability and awareness will aid in identifying and promoting the management of PrEP approaches in any community. This study aimed to assess awareness of the existence, knowledge, and acceptability of PrEP among undergraduate college students in Southern Thailand.
METHODS
Study design and setting
This was a descriptive cross-sectional study among undergraduate students of Walailak University, and data was collected in the period between December 1, 2020, and March 31, 2021. This research collected information from students attending health and nonhealth schools. Health schools included dental, pharmacy, medicine, public health, veterinary medicine, allied health sciences, and nursing schools. Nonhealth schools included engineering and technology, architecture and design, and informatics. Liberal arts, management, political science and law, science, agriculture and food industry, language and general education, and international colleges were among the nonmedical schools
Participants and sampling method
Using a convenience sampling method, we calculated a minimum sample size of 259 participants based on the total population of 8,080 individuals. Undergraduate participants aged 18 and above who were full-time and active students at Walailak University were eligible. Respondents who provided missing data or refused to sign the consent form were excluded from the study. All study respondents were approached and asked to fill out a survey during the whole period of data collection. We chose one representative from each school to be evaluated in accordance with the research questions. This representative respondent was trained well and was briefed on the main purpose of this study. They assisted in the distribution of surveys and data collection. Participants were asked to sign the consent form before beginning to answer the survey questions.
Measures
The questionnaire was developed and designed using the literature from Garcia and Harris et al. (2017) and Frankis et al. (2016) to assess PrEP awareness, knowledge, and acceptability. The questionnaire contained 16 items and was divided into 4 sections. The first section contains demographic information (age, gender, religion, residency status, school type, and year of study) as well as other personal data, such as sexual behavior (sexual orientation, number of sexual partners, history of sexually transmitted infections (STIs), and HIV testing history). The second part consisted of a single question that assessed awareness of PrEP. Have you ever heard about PrEP before? (e.g., yes, no). The third part consisted of six questions designed to assess knowledge of PrEP. These questions focused on the eligibility requirements for PrEP, the locations where PrEP can be obtained in Thailand, and the costs, utilization, and benefits of PrEP. The evaluation of PrEP knowledge was limited to students who were aware of PrEP (answered Yes in the second part). The last part included two questions to address the acceptability of PrEP. 1) If you are likely to have HIV and PrEP is an effective medication for reducing your risk of infection, would you agree to take PrEP? 2) If PrEP is effective at reducing the risk of HIV infection but has some side effects. Are you willing to take PrEP? To determine the acceptability of using PrEP, the subject had to agree on both questions.
Those participants who answered “yes” for Q1 were recognized to be aware of HIV PrEP, whereas those who selected “drug user or people who have sex with men” (MSM) from Q2, “hospital” from Q3, “yes” from Q4, “before getting HIV” from Q5, “1 tablet a day” from Q6, and “no” from Q7 were considered to have a precise idea about PrEP knowledge. Subjects who responded “accept” to Q8 and Q9 were also deemed HIV PrEP acceptable. According to Bloom (1968), if the participant answered correctly, ?80% indicates a high level of knowledge, 60%–79% indicates a moderate level of knowledge, and <60 indicates a low level of knowledge.
The questionnaire was evaluated by three medical experts (one HIV physician expert and two HIV pharmacist experts) who have good experience in reviewing items of the survey. The medical experts assessed the items based on the index of item-objective congruence. In addition, a pilot study was conducted on 30 randomly selected undergraduate students who did not participate in the final study to assess the clarity and ease of understanding of the items, as well as the length of time it took to complete the questionnaire. Their suggestions and comments were used to improve the questionnaires. However, they were not included in the final sample size.
Statistical analysis
This study was analyzed using Statistical Package for the Social Sciences version 28, and descriptive statistics were used for sociodemographic characteristics, awareness of existence, knowledge, and acceptability of PrEP. The continuous variables were represented as mean and standard deviation (SD) and were defined as percentages or frequency. The chi-square test and Fisher’s exact test were used to find the association between the variables, and logistic regression was also used to determine the strength of the relationship between variables.
RESULTS
The study included a total of 259 participants who completed all aspects of the questionnaire successfully. The average age of the participants was 20.54 years (SD = 1.30). The majority of participants (31.69%) were under the age of 21, female (65.00%), and Buddhist (86.15%) and lived in a university dormitory (75.00%). Almost half of the participants were enrolled in health-related programs (46.92%), and the rest (53.08%) were students in nonmedical schools. In terms of sexual behavior, the majority of participants (79.23%) had a heterosexual interest, and 80% of the respondents declared they had no sexual partner. There was no history of STIs among the participants, and only 6.92% had ever tested for HIV, despite the fact that the majority had (Table 1).
Awareness of existence of PrEP
As shown in Table 2, only 20.8% of participants were aware of the existence of PrEP. Awareness of the existence of PrEP was highest among females, students in health sciences-related schools, students with no defined sexual interest, students with multiple partners, and students who had ever tested for HIV. Students in health sciences-related schools were 8.6 times more likely to be aware of PrEP than students in other schools. There was a significant relationship between being aware of PrEP’s existence and attending school (p < 0.005) (Table 3).
Knowledge of PrEP
As shown in Table 2, only 20.8% (54/259) of the total respondents believed that PrEP should be taken prior to the risk of HIV infection. The majority of participants (63%, 34/54) were unable to determine who qualifies for PrEP, 72.2% (39/54) were unaware of where to obtain PrEP, and 55.6% (30/54) were unaware of the cost of PrEP. Further, 63% (34/54) had no idea about the time to take PrEP, 38.9% (21/54) knew the method of taking PrEP, and 42.6% (23/54) were aware that PrEP could prevent STIs. According to the chi-square results, sexual partner, school type, religion, residential status, and gender were all predictors of PrEP knowledge (p < 0.005) (Table 3). This finding is confirmed by logistic analysis, which showed that medical students were 0.096 times more knowledgeable about where to buy PrEP than nonmedical students [odds 95% CI: 0.096 (0.017–0.532)] (Table 4). Likewise, medical students were 0.046 times more aware of the price of PrEP than non-health students [odds 95% CI: 0.046 (0.006–0.375)]. Furthermore, females were 7.07 times more likely than males to be aware of how to take PrEP [odds 95% CI: 7.07 (1.509–32.89)] (Table 4). Finally, logistic analysis revealed that medical students were 9.81 times more likely than nonmedical students to be aware that PrEP could also be used to prevent STIs [odds 95% CI: 9.81 (1.731–55.601)] (Table 4).
Acceptability of PrEP
In general, only 39.8% of the 259 participants agreed to use PrEP (Table 2). Those who have previously denied using PrEP wanted more information before making a decision. There was a significant relationship between gender, school type, and PrEP acceptability rates (p < 0.005). Gender and school type were both determinants of PrEP acceptability, and logistic regression revealed that females attending health schools had the highest rates of PrEP acceptance (p < 0.005) (Table 5). Furthermore, nearly half of the females enrolled in medical schools stated that they would accept taking PrEP if they were at high risk of contracting HIV, and 83 (49.4%) stated that they need more information before deciding to take PrEP (Table 5). This finding was supported by logistic analysis, which revealed that female undergraduate medical students were 2.98 times more likely to accept PrEP even if it had some side effects, but they needed more information before taking it [odds 95% CI: 2.98 (1.574–5.772)]. When asked about the side effects of PrEP, however, the majority of the female students from health schools either refused or needed more information before taking PrEP (Table 5).
DISCUSSION
To the best of our knowledge, this is the first study to examine awareness of the existence, knowledge, and acceptability of PrEP among undergraduate students in Thailand. It also determined the relationship between sociodemographic variables and PrEP awareness, knowledge, and acceptability. Our findings indicated that awareness of PrEP was low, which is consistent with prior studies among young adults in Nigeria and South Africa that used similar questionnaires to evaluate their awareness (Ajayi et al., 2018; Shamu et al., 2021; Taggart et al., 2020) and a study conducted among MSM in Thailand (Yang et al., 2013) but significantly lower than the findings of studies conducted in developed countries (García and Harris, 2017; Iniesta et al., 2019; Okeke et al., 2021; Taggart et al., 2020; Werner et al., 2018). The reason for the low awareness of the existence of PrEP among groups at high risk of contracting HIV could be explained by the fact that providers of PrEP have not completely strengthened PrEP awareness campaigns in Thailand, where PrEP is still relatively new (Thailand’s Ministry of Public Health, 2018). Our data, on the other hand, was lower than one study conducted in Kenya, which revealed that 64% of respondents were aware of PrEP (Ogunbajo et al., 2019). This finding emphasizes the significance of a multifaceted, multimedia public awareness campaign that provides evidence-based information about PrEP when it becomes available. Furthermore, community leaders, social government agencies, and HIV-friendly healthcare practitioners should be involved as networks for disseminating PrEP data to Thai students.
Our study also discovered that undergraduate students had a lack of knowledge about HIV PrEP. Low PrEP knowledge is similar to previous studies conducted in Spain (Ferrer et al., 2016), Malaysia (Lim et al., 2017), and the USA (Krakower et al., 2012). Students of health sciences-related schools were more aware of PrEP than students in other schools (34.7%, 8.7%, respectively). It is possible that students studying health sciences may have learned about PrEP in their classes. Despite the fact that there was no significant relationship between HIV testing history and PrEP awareness, our finding revealed that students who had ever tested for HIV were less likely (33.33%) to be aware of PrEP than those who did not (66.66%). This result is different from the findings of a prior study (Ajayi et al., 2019). According to our results, it may mean that those who are not concerned about contracting HIV are more likely to be aware of available prevention strategies.
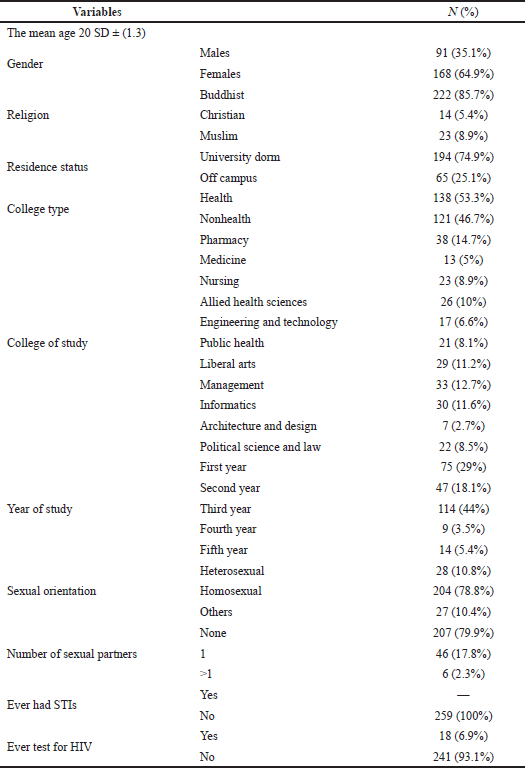 | Table 1. Sociodemographic characteristics, n = 259. [Click here to view] |
Our study found that undergraduate students are less accepting of PrEP than a prior report in Thai MSM (Plotzker et al., 2017). Participants who refused to take PrEP stated that they lacked sufficient information to consider PrEP. They wished to learn more about PrEP before making a decision. The other finding of this study is a low level of knowledge about PrEP. This is unsurprising, given that this method of prevention is relatively new in the study setting. A previous study among MSM in Ghana reported a low level of PrEP acceptability. However, their findings indicated that acceptability increased when participants knew about PrEP (Ogunbajo et al., 2019).
Another interesting finding from our study is that awareness of PrEP is associated with the acceptability rate. Participants who are aware of the existence of PrEP are more likely to accept it than those who are not. Being aware of PrEP is a step toward HIV prevention using PrEP. This may imply that before federal governments can foster demand for PrEP uptake, they must first guarantee that communities are aware of PrEP. Campaigns to encourage young people to use PrEP must first educate and raise community awareness about PrEP’s benefits and risks.
 | Table 2. Awareness, accseptability, and knowledge of HIV PrEP. [Click here to view] |
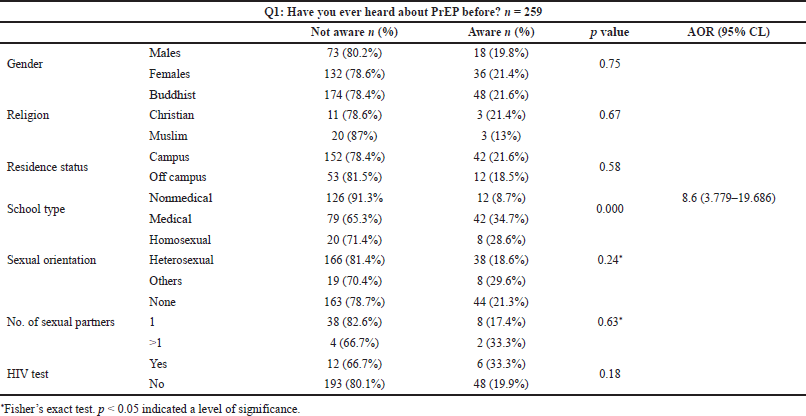 | Table 3. Association between HIV PrEP and awareness among participants, n = 259. [Click here to view] |
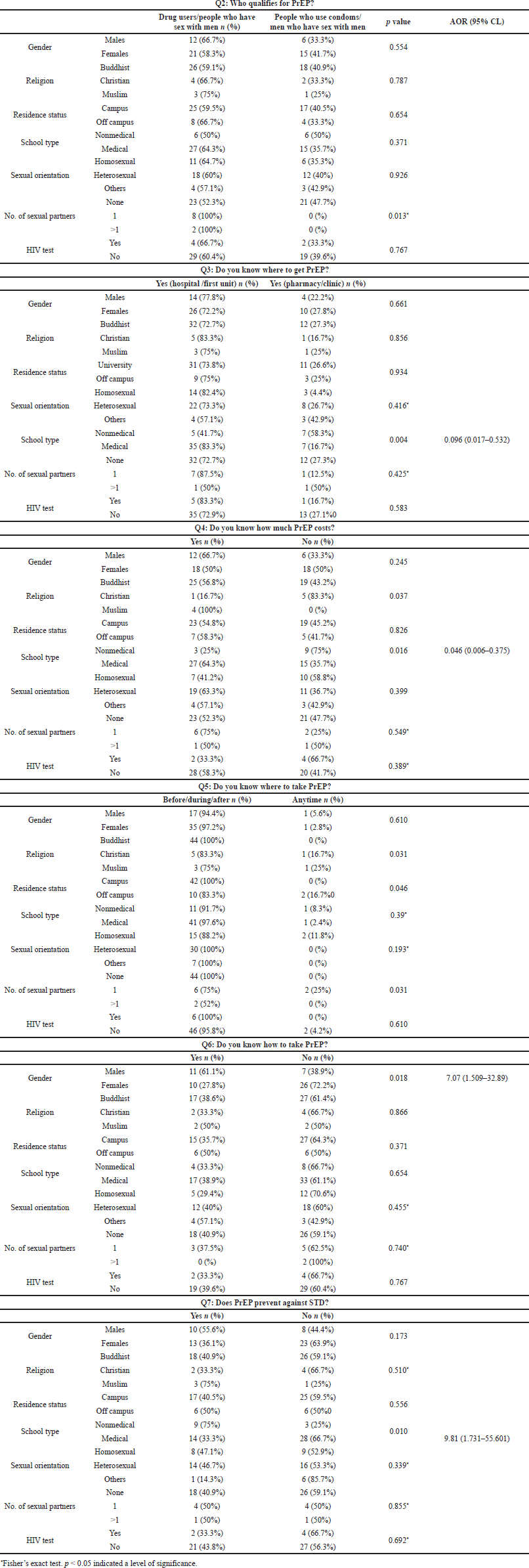 | Table 4. Association between HIV PrEP and knowledge among participants, n = 54. [Click here to view] |
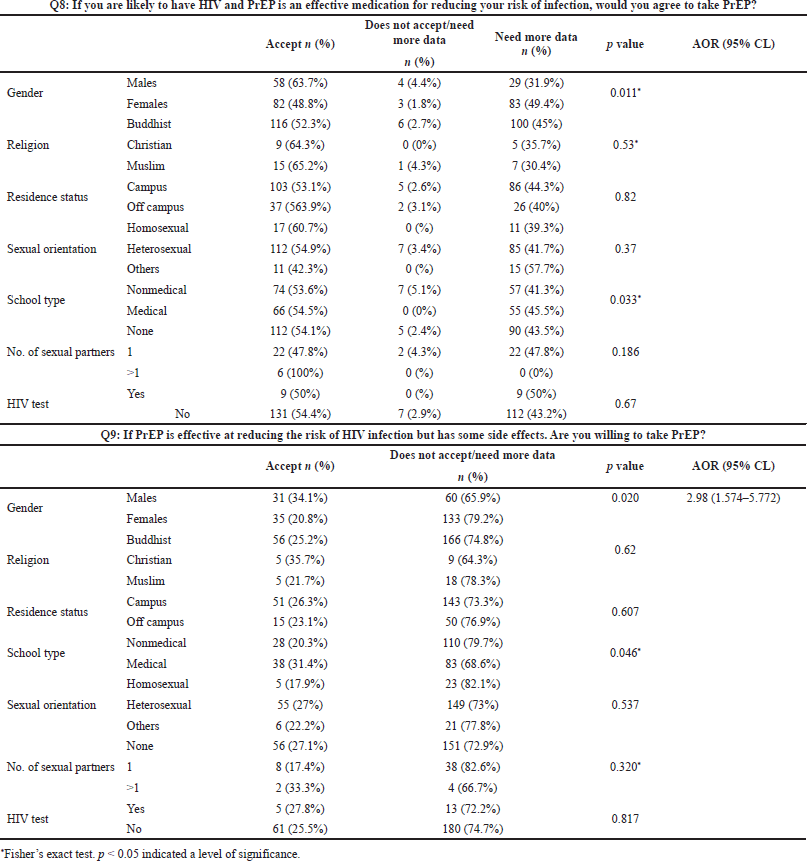 | Table 5. Association between HIV PrEP and acceptability among participants, n = 259. [Click here to view] |
According to our data, female health students have a conditional acceptance level of PrEP. Concerns about the negative effects of PrEP among respondents were similar to previous research findings (Goedel et al., 2016; Yi et al., 2017), which found adverse reactions to be a significant obstacle to the willingness to use PrEP among people at high risk of getting HIV. It is critical to make sure that Thai students are aware of the adverse effects and what to do if side effects exist. Finally, the observable efficiency of PrEP in preventing HIV was a requirement for its acceptance. Previous research has shown that skepticism about the efficacy of PrEP is correlated with a lower willingness to use PrEP (Yi et al., 2017). Providing Thai students with clear and understandable evidence of the efficacy of PrEP may alleviate some of their concerns about how well PrEP prevents HIV.
The study has two limitations. First, this cross-sectional design study does not establish causality from our findings. Second, results for this study were collected from a single university, which means that these findings cannot be generalized to Thailand as a whole. Finally, by using hypothetical questions, we assessed awareness of the existence and acceptability of PrEP. Although the fact that the questions had been used in previous research, caution should be practised when interpreting the results.
CONCLUSION
Despite these drawbacks, our observations focus on providing extra evidence on PrEP understandings and acceptability among university students. Selection of PrEP for high-risk individuals will enhance PrEP’s role in decreasing HIV transmission. This study demonstrates that awareness of the existence, knowledge, and acceptability of PrEP among university students in Thailand is low. To increase PrEP acceptability, awareness, public education, and engagement campaigns are necessary. Finally, more research is needed to determine whether PrEP awareness and knowledge correlate with population encouragement and satisfaction with PrEP.
ACKNOWLEDGMENTS
The authors would like to thank the Department of Pharmaceutical Care, School of Pharmacy, Walailak University, for their support. Moreover, great gratitude goes to Assist. Prof. Dr. Suriyon Uitrakul for the review and helpful comments. Finally, all participants that joined this study are the crucial elements for this accomplishment.
CONFLICTS OF INTEREST
No potential conflicts of interest were reported by the authors.
FUNDING
This study received no external funding.
DATA AVAILABILITY
Data used to support the findings of this study are available upon request from the author (Tiwaphon Thongsutt).
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
ETHICAL APPROVALS
This research was approved by the Human Research Ethics Committee of Walailak University No. WUEC -21-010-01.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Ajayi AI, Ismail KO, Adeniyi OV, Akpan W. Awareness and use of pre-exposure and postexposure prophylaxes among Nigerian university students. Medicine, 2018; 97(36):e12226; doi:10.1097/md.0000000000012226 CrossRef
Ajayi AI, Mudefi E, Yusuf MS, Adeniyi OV, Rala N, Goon DT. Low awareness and use of pre-exposure prophylaxis among adolescents and young adults in high HIV and sexual violence prevalence settings. Medicine, 2019; 98(43):e17716; doi:10.1097/md.0000000000017716 CrossRef
Bloom BS. Learning for mastery. Instruction and curriculum. Regional Education Laboratory for the Carolinas and Virginia, Topical Papers and Reprints, Number 1, 1968.
Ferrer L, Folch C, Fernandez-Davila P, Garcia A, Morales A, Belda J, Susperregui AR, Casabona J, Ad hoc Study Group for PrEP Acceptability. Awareness of pre-exposure prophylaxis for HIV, willingness to use it and potential barriers or facilitators to uptake among men who have sex with men in Spain. AIDS Behav, 2016; 20(7):1423–33 CrossRef
Frankis J, Young I, Flowers P, McDaid L. Who will use pre-exposure prophylaxis (PrEP) and why? Understanding PrEP awareness and acceptability amongst men who have sex with men in the UK—a mixed methods study. PLoS One, 2016; 11(4):e0151385; doi:10.1371/journal.pone.0151385 CrossRef
García M, Harris AL. PrEP awareness and decision-making for Latino MSM in San Antonio, Texas. PLoS One, 2017; 12(9):e0184014; doi:10.1371/journal.pone.0184014 CrossRef
Goedel WC, Halkitis PN, Greene RE, Duncan DT. Correlates of awareness of and willingness to use pre-exposure prophylaxis (PrEP) in gay, bisexual, and other men who have sex with men who use geosocial-networking smartphone applications in New York City. AIDS Behav, 2016; 20(7):1435–42. CrossRef
HIV and AIDS Data Hub for Asia Pacific. Key facts on HIV in Asia and the Pacific. 2019. Available via https://www.aidsdatahub.org/ (Accessed 1 June 2020).
Iniesta C, Álvarez-Del Arco D, García-Sousa LM, Alejos B, Díaz A, Sanz N, Garrido J, Meulbroek M, Pujol F, Moreno S, Fuster-Ruiz de Apocada MJ, Coll P, Antela A, Del Romero J, Ayerdi O, Riera M, Hernández J, Del Amo J. Awareness, knowledge, use, willingness to use and need of pre-exposure prophylaxis (PrEP) during World Gay Pride 2017. PLoS One, 2019; 14(4):e0216376; doi:10.1371/journal.pone.0216376 CrossRef
Krakower DS, Mimiaga MJ, Rosenberger JG, Novak DS, Mitty JA, White JM, Mayer KH. Limited awareness and low immediate uptake of pre-exposure prophylaxis among men who have sex with men using an internet social networking site. PLoS One, 2012; 7(3):e33119. CrossRef
Lim SH, Mburu G, Bourne A, Pang J, Wickersham JA, Wei CKT, Yee IA, Wang B, Cassolato M, Azwa I. Willingness to use pre-exposure prophylaxis for HIV prevention among men who have sex with men in Malaysia: findings from an online survey. PLoS One, 2017; 12(9):e0182838. CrossRef
Ogunbajo A, Iwuagwu S, Williams R, Biello K, Mimiaga MJ. Awareness, willingness to use, and history of HIV PrEP use among gay, bisexual, and other men who have sex with men in Nigeria. PLoS One, 2019; 14(12):e0226384. CrossRef
Okeke NL, McLaurin T, Gilliam-Phillips R, Wagner DH, Barnwell VJ, Johnson YM, James O, Webb PB, Parker SD, Hill B, McKellar MS, Mitchell JT. Awareness and acceptability of HIV pre-exposure prophylaxis (PrEP) among students at two historically Black universities (HBCU): a cross-sectional survey. BMC Public Health, 2021; 21(1):1–9; doi:10.1186/s12889-021-10996-2 CrossRef
Plotzker R, Seekaew P, Jantarapakde J, Pengnonyang S, Trachunthong D, Linjongrat D, Janyam S, Nakpor T, Charoenying S, Mills S, Vannakit R, Cassell M, Phanuphak P, Lertpiriyasuwat C, Phanuphak N. Importance of risk perception: predictors of PrEP acceptance among Thai MSM and TG women at a community-based health service. J Acquir Immune Defic Syndr, 2017; 76(5):473–81; doi:10.1097/qai.0000000000001536 CrossRef
Shamu S, Shamu P, Khupakonke S, Farirai T, Chidarikire T, Guloba G, Nkhwashu N. Pre-exposure prophylaxis (PrEP) awareness, attitudes and uptake willingness among young people: gender differences and associated factors in two South African districts. Glob Health Action, 2021; 14(1):1886455; doi:10.1080/16549716.2021.1886455 CrossRef
Taggart T, Liang Y, Pina P, Albritton T. Awareness of and willingness to use PrEP among Black and Latinx adolescents residing in higher prevalence areas in the United States. PLoS One, 2020; 15(7):e0234821; doi:10.1371/journal.pone.0234821 CrossRef
Thailand’s Ministry of Public Health. Thailand National Guidelines on HIV/AIDS Diagnosis, Treatment and Prevention. 2021. Available via http://www.thaiaidssociety.org/images/PDF/thai_aids_guidelines_2020_2021.pdf
Thailand’s Ministry of Public Health. Thailand National Guideline on pre-exposure prophylaxis: HIV-PrEP. Aksorn Graphic and Design Publishing Limited Partnersip. 2018. Available via http://aidssti.ddc.moph.go.th/medias/view/126/549
UNAIDS. HIV AIDS Asia Pacific Research Statistical Data Information Resources—AIDS Data Hub. 2021. Available via https://aphub.unaids.org/ (Accessed 1 June 2021).
Werner RN, Gaskins M, Ahrens J, Jessen H, Kutscha F, Mosdzen R, Osswald W, Sander D, Schellberg S, Schwabe K, Wünsche T, Dressler C, Sammons M, Nast A. Knowledge and use of HIV pre-exposure prophylaxis among men who have sex with men in Berlin—a multicentre, cross-sectional survey. PLoS One, 2018; 13(9):e0204067; doi:10.1371/journal.pone.0204067 CrossRef
World Health Organization. Sustainable development goals. 2020. Available via https://www.who.int/health-topics/sustainable-development-goals (Accessed 1 June 2021).
World Health Organization. Updated recommendations on HIV prevention, infant diagnosis, antiretroviral initiation and monitoring. 2021b. Available via https://apps.who.int/iris/rest/bitstreams/1336192/retrieve
World Health Organization. HIV data and statistics. 2021a. Available via https://www.who.int/teams/global-hiv-hepatitis-and-stis-programmes/hiv/strategic-information/hiv-data-and-statistics (Accessed 1 June 2021).
Yang D, Chariyalertsak C, Wongthanee A, Kawichai S, Yotruean K, Saokhieo P, Guadamuz T, Suwanvanichkij V, Beyrer C, Chariyalertsak S. Acceptability of pre-exposure prophylaxis among men who have sex with men and transgender women in Northern Thailand. PLoS One, 2013; 8(10):e76650; doi:10.1371/journal.pone.0076650 CrossRef
Yi S, Tuot S, Mwai GW, Ngin C, Chhim K, Pal K, Igbinedion E, Holland P, Choub SC, Mburu G. Awareness and willingness to use HIV pre-exposure prophylaxis among men who have sex with men in low-and middle-income countries: a systematic review and meta-analysis. J Int AIDS Soc, 2017; 20(1):21580. CrossRef