INTRODUCTION
Mental health is an integral part of health and well-being. According to the World Health Organization (WHO), mental health is “a state of well-being in which the individual realizes his or her own abilities, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to his or her community” (Bhugra et al., 2013). Mental health disorders are one of the leading causes of disability (Hambisa et al., 2020). A study estimated that 792 million people in 2017 lived with a mental health disorder which was slightly more than 1 in 10 people globally (10.7%) (Ritchie et al., 2020). Anxiety is the most common, followed by depression disorder (Hollyman, 2002). The WHO Action Plan on Mental Health (2013–2020) signifies that a collective evidence-based effort is needed for the improvement of worldwide mental health (WHO, 2013). Despite substantial research advances showing what can be done to prevent and treat mental disorders and to promote mental health, translation into real-world effects has been painfully slow (Patel et al., 2018).
University students’ mental health represents a growing public health concern requiring epidemiological data (Eisenberg et al., 2013). Psychological health is crucial for their academic achievement, social progress, economic development, and success of a country. It is well documented that healthcare university students experience a higher level of stress than their university peers (Dyrbye et al., 2006; Mao et al., 2019; Omigbodun et al., 2006).
Worldwide research indicates a high level of depression, anxiety, and stress (DAS) among different healthcare students (AlFaris et al., 2016; Bati et al., 2013; Bresolin et al., 2020; Ersan et al., 2018; Macauleya et al., 2018; Quek et al., 2019). In Saudi Arabia, the recent upgradations of health education curricula have increased stress liability. Saudi Gazette of 2017 reported that 67% of the medical students were stressed (Saudi Gazette Report, 2017). In addition, high incidences of psychological disorders have been reported among Saudi medical (Abdulghani et al., 2011; Alghamdi et al., 2017; Al Rasheed et al., 2017; Ibrahim et al., 2013; Kulsoom et al., 2015), dental (Basudan et al., 2017), pharmacy/Pharm D (Bin-Mallouh et al., 2016; Gallagher et al., 2014; Hakami, 2018; Khalid et al., 2017), and nursing students (Alahmed et al., 2018). Hence, a comparative study of different psychological conditions among healthcare students could be of interest and helpful to policymakers of higher education.
The screening of students’ mental health is crucial to understanding the prevalence rates of DAS as well as the associated factors. The present study aimed to investigate the prevalence of DAS among university undergraduate healthcare students for a better understanding of the relationship with the course and other contributing factors. Ultimately, the outcomes of the study can aid in the planning and development of efficient screening and intervention programs to prevent psychological problems in the target population, make policies, and find sustainable solutions.
MATERIALS AND METHOD
Setting and population
A cross-sectional study was conducted among the students of MBBS (medical), BDS (dental), Pharm D, and BSc (nursing) programs offered at different colleges of Jazan University, Saudi Arabia. All students in the second to final year of their study program available during October to December of 2018 were included as participants. In each class, after a regular lecture, the students were briefed about the purpose of the research by our well-trained internship students in the final year Pharm D program. All participants were provided the information brochure prior to the questionnaire. The questionnaires were then distributed to those who volunteered for participation. The first-year students were excluded from the study as they are more likely to be biased due to the apprehensive trait that they may relate their response scores to curricular performance evaluation. Similarly, the students under treatment may provide responses under the influence of their medication and counseling according to psychological status and hence were excluded.
Sample size
The estimated sample size was 334 based on the 5% margin of error, 50% prevalence, and 95% confidence interval. In order to minimize error and account for nonresponders, an additional sample was included in the study (Tripathi et al., 2020).
Study tools
A standardized (structured, precoded, and validated) questionnaire was developed which consisted of two parts. The first part inquires about sociodemographic information, and the second part is based on Depression, Anxiety, and Stress Scale (DASS). The short version of the DASS (DASS-21) was considered superior to the full-scale version DASS-42 being a validated, reliable, and consistent instrument; it requires less time to administer and offers better psychometric properties. The reliability coefficient of the DAS scales ranges from 0.81 to 0.97, and the three subscales show discriminative ability to differentiate between psychiatric and nonpsychiatric respondents (McDowell, 2006). The depression, anxiety, and stress level of students were measured using the subscale scores categorized as per the Lovibond scoring scale for psychological mood (Table 1). This scoring scale consists of a set of three self-report scales with seven items per scale to measure the negative emotional states of DAS levels (Lovibond e al., 1995). Based on the DASS manual for student samples, (1) difficulty in relaxing, nervous arousal, and ease of being agitated are assessed on the stress scale; (2) autonomic arousal and skeletal muscle effect are assessed on the anxiety scale; and (3) dysphoria, hopelessness, self-deprecation, and lack of interest are assessed on the depression scale.
The final score for each subscale of DASS was calculated by summing the DASS-21 scores of the relevant items and multiplied by two to obtain values corresponding to the full version (DASS-42). The severity was evaluated in each case on the basis of its rating index. A pilot questionnaire was pretested on 10 random students of a healthcare college, and the language of questions was revised based on the feedback to simplify understanding.
Outcome measures
The current study assesses the level of stress, anxiety, and depression based on the DASS-21 questionnaire and attempts to implicate the explanatory variables such as area, gender, age, healthcare program type, academic years, grade point average (CGPA) grade, body mass index (BMI), marital status, living status, and economic status. The study also measures the contribution of possible risk factors, viz. academic, family and relationship, health and lifestyle, and environment-related issues that affect mental health levels. The study questionnaire included seven commonly appreciated mood alleviators: emotional support from family, friends, or others, physical exercise, religious practice, getting involved in other activities, professional help, sleep or taking a nap, and giving up the task.
Data collection and statistical analysis
Data were collected using a random sampling method and analyzed using the Stata 15.0 software. For categorical variables, data were presented as frequencies and percentages. A chi-squared test was used to examine the association between each item in psychological health and the explanatory variable in the bivariate analysis. Multivariable logistic regression was computed using stress, anxiety, and depression as an outcome separately to examine the relationships in the adjusted analysis. p-value ≤0.05 was considered statistically significant.
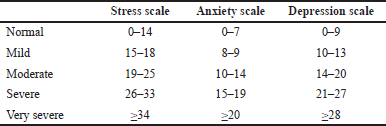 | Table 1. Lovibond scoring scale for psychological mood. [Click here to view] |
Ethical considerations
Ethical approval was obtained from the Scientific Research Ethics Committee, Jazan University, via Reference No. 203/1601/1440. Verbal consent to conduct the survey was obtained from the heads of each healthcare program before beginning the research. All participants were briefed about the procedures, purpose, and significance of the study, and written consent was obtained from each participant before distributing the questionnaire. Confidentiality and anonymity were assured through the codification of collected data.
RESULTS
Sociodemographic characteristics of the healthcare students
Depending on the presence in class and exclusions as mentioned before, 600 questionnaires were distributed among four healthcare departments, viz. medical, dental, nursing, and pharmacy, of which 473 were completed and returned, indicating the participation rate of 78.83%. The statistics of their demographic and socioeconomic details are presented in Table 2. Pharmacy students (150; 31.7%) contributed the maximum response, while medical students’ contribution was the least, 22% of the total. Most of the respondents (98.5%) were Saudi nationals, and 54.3% belonged to rural areas, while 45.7% were from the urban region. The participants were female in the majority (86.3%) and in the age group of 20–24 years. Of these, 66.8% were single and 27.7% married, while the remaining few were either divorced or did not prefer to disclose their marital status. Among the respondents, most (77.8%) were staying with family, and a fairly good proportion stayed with their friends (12.5%) or lived alone (9.3%). The socioeconomic groups of participants with a nominal family income below 5,000 SAR represented 29.2%, while those with 5,000–10,000 SAR formed the greater component (33.2%), but those with income more than 10,000 SAR were less (20.1%). A significant number (82; 17.3%) refrained from declaring their family income (Table 2).
Prevalence of DAS among study participants
The overall DAS scores (mild to extremely severe), for the whole population of healthcare students put together, indicate that anxiety (78.6%) was the most common psychological condition, followed by depression (72.1%) and then stress (61.5%) (Fig. 1). Furthermore, the depression and anxiety levels were significantly higher in females than male participants, while stress levels among the two genders did not differ significantly. More female respondents (75%) suffer from depression, with 36.3% in the severe to extremely severe range, while a relatively smaller proportion (53.8%) of males had depression, and only 16.9% fall in the severe to extremely severe category. Also, anxiety is observed in 80.6% of the female population compared to that in the male population (66.2%), and severe to extremely severe anxiety existed in 49% of the females compared to males (18.5%) (Table 3).
The comparison of the psychological conditions among different healthcare programs shows that the highest incidence of depression (mild to extremely severe level) was found among medical students (86.5%), followed by dental, nursing, and pharmacy, while anxiety and stress were reported to be high among dental students (89.3% and 79.5%), followed by medical, nursing, and pharmacy. However, the severity score (severe to extremely severe level) of DAS (45.2%, 63.5%, and 36.5%) was highest among medical students, followed by nursing students, respectively. It was observed that pharmacy students were significantly (p < 0.05) less depressed, anxious, and stressed than other healthcare participants (Table 4).
The psychological state of students at different levels/years of their studies was found to be different. Medical students reported the highest percentage of depression in the fourth year (93.1%), anxiety in the third year (91.7%), and stress in the second year (78.6%) of academic studies. Depression existed at a higher percentage (90.6%) in the third year, while anxiety and stress were higher in the fourth year of dental studies. Similarly, in nursing also the highest depression rates were reported in the third year (83.8%), anxiety in the fifth and fourth years, and stress in the fourth year of their study. In pharmacy, more students in the fifth year (52.8%) reported depression; second year had anxiety; and internship students suffered from stress. The academic year was found to be a nonsignificant variable for DAS among medical, nursing, and pharmacy participants. Dental students also do not show much variation in depression and stress with the year of study, but the level of anxiety was significantly higher (p = 0.02) in the fourth- and fifth-year students of dentistry (Table 5).
In bivariate analysis, the differences among CGPA groups were significant for depression and anxiety (p = 0.016 and 0.026) among those with high and low CGPA but nonsignificant for stress (Fig. 2). Moreover, depression was found to be highest among overweight (85.7%), followed by obese (80.5%), then underweight, and then normal participants (Fig. 3). All participants displayed the highest prevalence of anxiety, followed by depression and stress that differed significantly among the BMI groups (p = 0.006, 0.025, and 0.032, respectively).
Table 6 shows the adjusted odds ratios and their 95% confidence intervals for the explanatory variables from logistic regressions in which the outcomes were depression, anxiety, and stress. The adjusted analyses indicate that students in medical (OR: 5.36; p value <0.001), dental (OR: 3.42; p value< 0.001), and nursing (OR: 4.46; p < 0.001) colleges were more likely to have depression than those in the pharmacy college. Likewise, they were more likely to have anxiety and stress than pharmacy students. Female students were more likely to have depression (OR: 3.63; p < 0.001) and anxiety (OR: 6.05; p < 0.001) than male students. Internship students were more likely to have depression (OR: 2.43; p = 0.036) and anxiety (OR: 0.41; p = 0.048) than those in other academic years. Moreover, students with high CGPA (4.50–5.00) (OR: 1.84; p = 0.027) and obese students (OR: 2.31; p = 0.041) were more likely to have stress than others.
Stressors and stress alleviators
The majority of the respondents (68.1%) reported academic factors as the foremost risk factor for triggering stress, while 50.9% attributed the stress to family- and relationship-related issues. Health-related concerns and environmental factors were also indicated as contributing factors for growing stress by an appreciable number of respondents (Fig. 4).
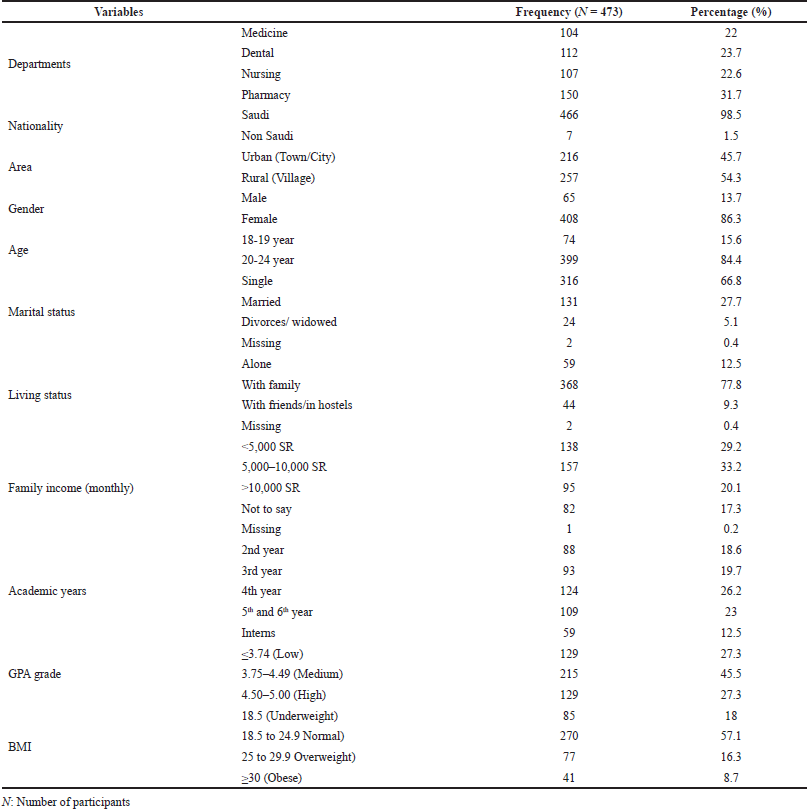 | Table 2. Demographic and socioeconomic details. [Click here to view] |
The participants used different coping methods of their preference independently, in combination, or sequentially or to get rid of circumstantial stress. The responses indicated that the preferred method to reduce stress was emotional support (16.3%), followed by physical exercise (15.6%) and diverting attention by getting involved in other activities (12.9%). The other options were also accepted as effective means of reducing or overcoming stress. A matter of grievous concern is that unfortunately 8.6% of participants responded that they might even prefer to give up (Fig. 5).
DISCUSSION
The current study was undertaken to address the psychological health issues among undergraduate healthcare students and determine how different variables, i.e., gender, program type, professional year, CGPA, and BMI, relate to DAS.
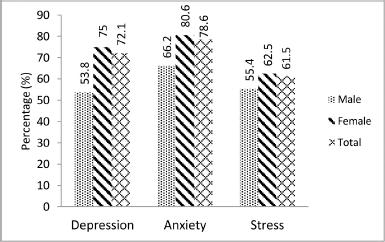 | Figure 1. Prevalence of DAS among all healthcare student participants. [Click here to view] |
Depression appeared highest among medical students in comparison to participants of other healthcare programs, while anxiety and stress were found more in dental students, which is in accordance with inferences of similar previous studies pertaining to the Middle East (Amr et al., 2013; Birks et al., 2009; Ibrahim et al., 2015; Mane et al., 2011; Waghachavare et al., 2013). However, some other studies reported contrasting results with higher incidences of stress in the medical program (Alqomaizi et al., 2018; Dutta et al., 2006; Moayedi et al., 2016). Foster et al. (2018) reported that students of dentistry and pharmacy were more stressed than those of nursing. Furthermore, less prevalence of DAS was found in pharmacy compared to other healthcare students, which is supported by previous reports (Alqomaizi et al., 2018; Dutta et al., 2006; Mane et al., 2011). On the contrary, Henning et al. (1998) reported a disproportionately high level of distress in pharmacy students.
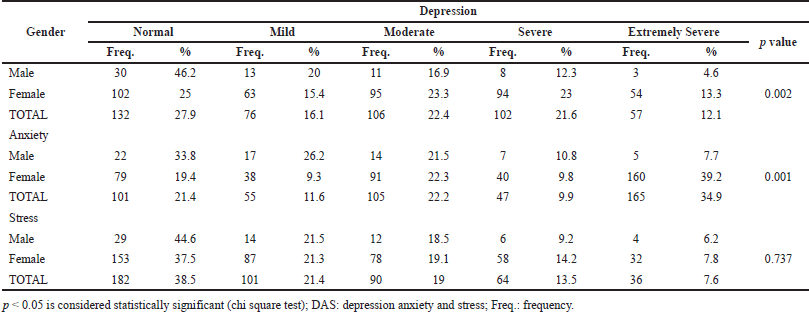 | Table 3. Gender-wise prevalence of DAS among healthcare students. [Click here to view] |
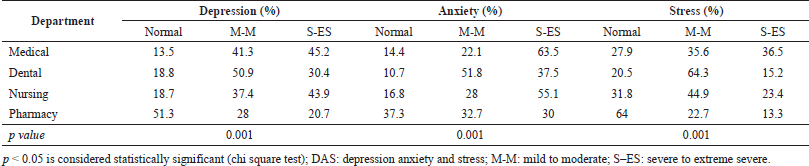 | Table 4. Prevalence of DAS among different healthcare departments. [Click here to view] |
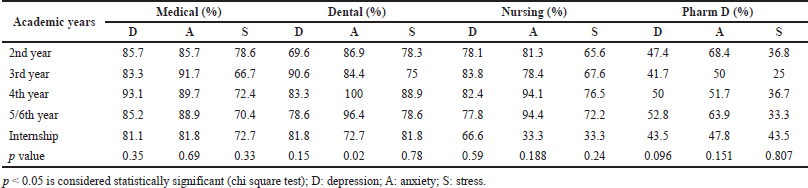 | Table 5. Academic year-wise prevalence of DAS among healthcare students. [Click here to view] |
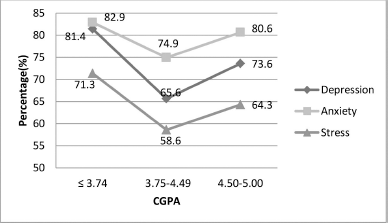 | Figure 2. Prevalence of DAS among healthcare students by CGPA groups. p < 0.05 is considered statistically significant (chi-square test); D: depression; A: anxiety; S: stress. [Click here to view] |
The discrepancies in psychological health among different healthcare programs could be attributed to the different educational environments, course curricula, teaching patterns, expectations, skills for professional training, psychological support from parents, teachers, and peers, and cultural and social values of the different geographic regions being studied.
The students’ level of study is a probable moderating factor for their psychological well-being, but the evidence is debatable. Similar to previous reports, our study also indicates medical students were psychologically disturbed throughout their course (Niemi et al., 2006); depression and anxiety score was noted to be highest in the fourth year (Kulsoom et al., 2015) and anxiety in the third year (Alghamdi et al., 2017), and stress score was recorded more in the second year (Dahlin et al., 2005), which is in concordance with previous reports. The findings can be attributed to the fact that medical students not only face continuous examinations throughout their academic program but are also expected to accomplish multiple clinical tasks in all specialties making the study of medicine more demanding and leaving smaller scope to socialize and recreate.
Dental students experience disturbance in their clinical years compared to preclinical years (Alzahem et al., 2013; Halboub et al., 2018) of the program when the transition from learning to clinical practice takes place. This could be due to an increased level of involvement in the clinical phase of the curriculum, where they start more responsible patient handling. Mental health was noted to be poor among nursing students of advanced years compared to in earlier years. Similarly, Oermann (1998) also found that stress increased as they progressed through the program; this might be because of two main domains, “patients care” and “clinical training,” which is not prominent in preclinical levels and students are somewhat relaxed.
Regarding pharmacy students, DAS was found more in initial and later years compared to middle years. However, previous studies reported that advanced-year pharmacy students had less stress than initial levels (Henning et al., 1998; Dutta et al., 2006; Votta et al., 2013). The findings can be referring to the fact that the entry-level students may face difficulties in adjusting to the new environment, but as they move into the middle years, they become more adapted to the academic intricacies of the program and devise more efficient ways to overcome different stressors and anxiety, but during their final year of studies they are obliged to accomplish multiple assignments and lab and clinical tasks as well as to learn professional patient-care skills during internship causing enormous psychological pressure.
As indicated by multivariate regression analysis, the internship students of all courses were more likely to have depression and anxiety that could be attributed to speculations of career challenges.
The present findings indicate that female healthcare students were more vulnerable to getting disturbed psychologically than males. This is consistent with several previous studies all around the world (Waghachavare et al., 2013; Moayedi et al., 2016; Amr et al., 2013; Alahmed et al., 2018) as well as in KSA among medical (Moayedi et al., 2016; Kulsoom et al., 2015), dental (Basudan et al., 2017; Hakami, 2018; Halboub et al., 2018), and pharmacy students (Basudan, 2017). Still, some reports found that there is no significant difference according to gender (Niemi et al., 2006). Gender comparisons could not be made for nursing courses as the present study included only female participants.
The higher prevalence of psychological stress among Saudi female students might have originated from the undergoing sociocultural reforms in the recent few years that promote professional education among females. As a result, more than half of the registered medical, dental, nursing, and pharmacy students are female, indicating a larger representation of women in once male-dominated fields in Saudi Arabia. Perhaps this recent trend has imposed some of the pressure on women to face the challenges of proving their worth equal or even outperforming their male counterparts.
Students who suffer from DAS are usually at risk of poor academic performance with lower grade point averages (Akinsola et al., 2017). The present study found a negative correlation, as has been reported earlier for dental (Halboub et al., 2018) and pharmacy students (Waghachavare et al., 2013). Poor psychological health among students with high CGPA can be attributed to the individual challenge of maintaining the position and superiority among their peers. However, few studies concluded that psychological health is not associated with CGPA in medical (Yusoff et al., 2013), pharmacy (Bin-Mallouh et al., 2016; Dutta et al., 2016), and even dental students (Basudan et al., 2017).
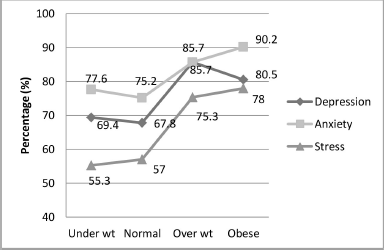 | Figure 3. Prevalence of DAS among healthcare students by BMI groups. p < 0.05 is considered statistically significant (chi-square test); D: depression; A: anxiety; S: stress. [Click here to view] |
BMI is associated with the clinical manifestation of psychological problems (Javadi et al., 2017). In the present study, overweight and obese participants were found to be more depressed, anxious, and stressed, which adds to the growing evidence that mental health may be important at higher ends (high BMI) of the weight spectrum. This may be attributed to their effortful attempt to regain normal BMI with a fear of obesity-associated diseases like diabetes and hypertension at an early age. Interestingly, in our study, area, age, living status, marital status, and family income were nonsignificant predictors of DAS among healthcare undergraduates.
The factors precipitating psychological distress cannot be uniform globally and are likely to be influenced by local traditions and sociocultural characteristics of the study group. The key stress triggers in the current study were academic factors such as examinations, assignments, laboratory/clinical practices, and grades. In addition to education demand, the participants also appreciated the family, environmental, and health-associated factors as an important cause of mental disturbances. The present findings corroborate other similar investigations conducted among healthcare students all over the world, including in Saudi Arabia. The stress among students is a temporary phenomenon, and when they are exposed to such condition, they adopt some means to alleviate it. Spending time with family and friends ranked first as a key stress alleviator in our study; similar findings were reported by others (Beall et al., 2015; Mane et al., 2011).
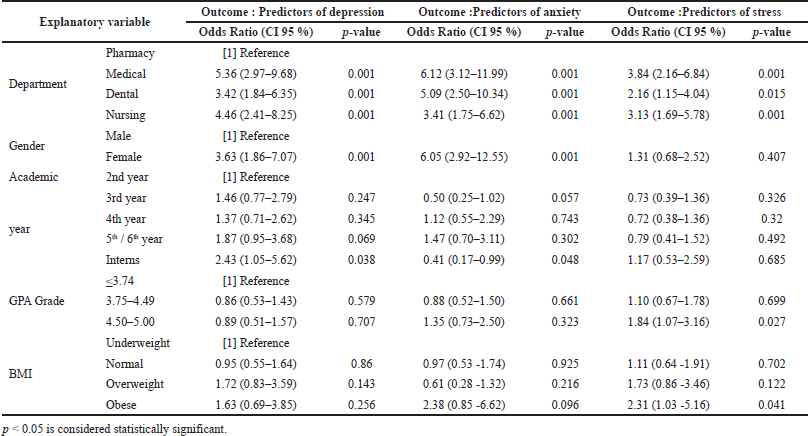 | Table 6. Multivariable logistic regression. [Click here to view] |
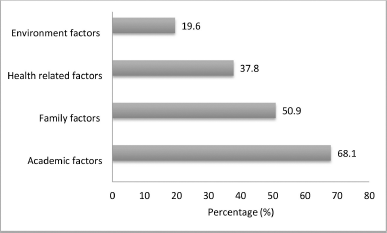 | Figure 4. Main stressors among healthcare student participants. [Click here to view] |
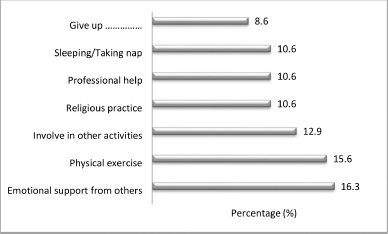 | Figure 5. Methods for stress reduction. [Click here to view] |
Limitations
This is a cross-sectional study among the students of Saudi Arabia (single ethnicity) performed at only one campus (Jazan University); hence, caution needs to be taken in generalizing the results. Instead of authenticated administrative records, the study relies on self-reported CGPA scores, weight, and height (BMI), etc., which may influence or limit survey outcomes. The conditions reflected in this study represent the state of mind at that particular moment and may be different in other stressful situations, like exams.
CONCLUSION
Students of all healthcare programs included in the study are exposed to different levels of DAS. However, medical, dental, and nursing students are more prone to developing psychological sickness than pharmacy ones. Variables like gender, academic year, CGPA, and BMI contribute positively to influence the psychological appreciation of DAS. Females, interns, high CGPA, and obese participants are more vulnerable to poor mental health. Academic factors are the key stressor while seeking emotional support is the main stress reliever. Additional studies on a larger population may be warranted to evaluate the individual contribution of different factors in elevating stress level among healthcare students to such a high level and to devise more effective interventions.
There is an urgent need for intervention by specific measures to ensure a substantial decrease in the psychological burden of the students. Adequate interventions through curricular reforms, the creation of a student-friendly environment, and counseling for the target sensitive group may improve psychological health. Furthermore, the teachers and parents should be made aware that an undue expectation about academic achievement is responsible for distress. The students shall be encouraged to indulge in regular extracurricular activities to avoid stress and seek help from friends, family, or religious leaders to overcome the formidable DAS.
CONFLICTS OF INTEREST
The authors report no financial or any other conflicts of interest in this work.
ACKNOWLEDGMENTS
The authors are thankful to Fatima MH, Mashael JM, Khulud MN, Saja IH, and Rawan H, the Pharm D internship students, College of Pharmacy, Jazan University, for their assistance in collecting data. The authors acknowledge the cooperation and unbiased volunteering by students of the healthcare colleges of Jazan University, viz. Pharmacy, Medicine, Dental, and Nursing.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
FUNDING
There is no funding to report.
ETHICAL APPROVALS
Ethical approval was obtained from the Scientific Research Ethics Committee, Jazan University, via Reference No. 203/1601/1440.
DATA AVAILABILITY
All data generated and analyzed are included within this research article.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Abdulghani HM, AlKanhal AA, Mahmoud ES, Ponnamperuma GG, Alfaris EA. Stress and its effects on medical students: a cross-sectional study at a college of medicine in Saudi Arabia. J Health Popul Nutr, 2011; 29(5):516–22. CrossRef
Akinsola EF, Nwajei AD. Test anxiety, depression and academic performance: assessment and management using relaxation and cognitive restructuring techniques. Psycholgy, 2013; 4(06):18–24. CrossRef
Al Rasheed F, Naqvi AA, Ahmad R, Ahmad N. Academic stress and prevalence of stress-related self-medication among undergraduate female students of health and non-health cluster colleges of a public sector University in Dammam, Saudi Arabia. J Pharm Bioallied Sci, 2017; 9(4):251–8; doi: 10.4103/jpbs.JPBS_189_17
Alahmed S, Anjum I, Masuadi E. Perceptions of mental illness etiology and treatment in Saudi Arabian healthcare students: a cross-sectional study. 2018; SAGE Open Med, 2018; 6:1–10; doi: 10.1177/2050312118788095 CrossRef
AlFaris E, Irfan F, Qureshi R, Naeem N, Alshomrani A, Ponnamperum G, Vleuten C. Health professions’ students have an alarming prevalence of depressive symptoms: exploration of the associated factors. BMC Med Educ, 2016; 16:279; doi:10.1186/s12909-016-0794-y CrossRef
Alghamdi T, Ansari T, Alfahaid F, Alzaharani M, Almansour M, Sami W, Alnasser A, Almutiri I, Alanazi T, Albader S. Prevalence of mental distress among undergraduate medical students at Majmaah university, Kingdom of Saudi Arabia. Majmaah J Heal Sci, 2017; 5(2):66–75. CrossRef
Alqomaizi N, Alfarraj A, Alrefy H, Altwair M, Almaaz D, Asdaq SMB. Prevalence of stress and its associated factors among students of Al-Maarefa Colleges of Riyadh, Saudi Arabia: a comparative cross-sectional study. Asian J Pharm, 2018; 12(2):S698.
Alzahem AM, Van der Molen HT, De Boer BJ. Effect of year of study on stress levels in male undergraduate dental students. Adv Med Educ Pract, 2013; 4:217–22; doi: 10.2147/AMEP.S46214 CrossRef
Amr M, Amin TT, Saddichha S, Malki SA, Al Samail M, Al Qahtani N, Al AbdulHadi A, Al Shoaibi A. Depression and anxiety among Saudi university students: prevalence and correlates. Arab J Psychiatry, 2013; 24:1–7; doi:10.12816/0000092 CrossRef
Basudan S, Binanzan N, Alhassan A. Depression, anxiety and stress in dental students. Int J Med Educ, 2017; 8:179–86; doi: 10.5116/ijme.5910.b961 CrossRef
Bati AH, Ozer MA, Govsa F, Pinar Y. Anxiety of first cadaver demonstration in medical, dentistry and pharmacy faculty students. Surg Radiol Anat, 2013; 35(5):419–26; doi: 10.1007/s00276-013-1075-7 CrossRef
Beall JW, DeHart RM, Riggs RM, Hensley J. Perceived stress, stressors, and coping mechanisms among doctor of pharmacy students. Pharmacy, 2015; 3(4):344–54; doi:10.3390/pharmacy3040344 CrossRef
Bhugra, D., A. Till, Sartorius N. What is mental health? Int J Soc Psychaiatry, 2013; 59(1):3–4; doi: 10.1177/0020764012463315 CrossRef
Bin-Mallouh LT, Gamal M, Ali AAH, Abdelrahim MEA, Khan MSA, Al-Sanea MM. Investigation of perceived stress and quality of life assessment of Pharm. D. students at Ibn Sina National College in Saudia Arabia during 2016. J App Pharm Sci, 2018; 8(3):82–90; doi:10.7324/JAPS.2018.8312
Birks Y, McKendree J, Watt I. Emotional intelligence and perceived stress in healthcare students: a multi-institutional, multi-professional survey. BMC Med Educ 2009;9:61; doi: 10.1186/1472-6920-9-61 CrossRef
Bresolin JZ, Dalmolin GL, Vasconcellos SJL, Barlem ELD, Andolhe R, Magnago TSBS. Depressive symptoms among healthcare undergraduate students. Rev Lat Am Nursing, 2020; 28:e3239; doi:10.1590/1518-8345.3210.3239 CrossRef
Dahlin M, Joneborg N, Runeson B. Stress and depression among medical students: a cross-sectional study. Med Educ, 2005; 39:594–604; doi:10.1111/j.1365-2929.2005.02176.x CrossRef
Dutta AP, Pyles MA, Miederhaff P. Measuring and understanding stress in pharmacy students. In: Landow MV (eds). Stress and mental health of college students, Nova Science Publishers, Hauppauge, NY, pp 1–28, 2006.
Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med, 2006; 81(4):354–73. CrossRef
Eisenberg D, Hunt J, Speer N. Mental health in American colleges and universities: variation across student. J Nerv Ment Dis, 2013; 201:60–7. CrossRef
Ersan N, Döleko?lu S, Fi?ekçio?lu E, ?lgüy M, Oktay ?. Perceived sources and levels of stress, general self-efficacy and coping strategies in preclinical dental students. Psychol Health Med, 2018; 23(5):567–77; doi:10.1080/13548506.2017.1384844 CrossRef
Foster K, Fethney J, Kozlowski D, Fois R, Reza F, McCloughen A. Emotional intelligence and perceived stress of Australian pre-registration healthcare students: a multi-disciplinary cross-sectional study. Nurse Educ Today, 2018; 66:51–6; doi:10.1016/j.nedt.2018.04.001 CrossRef
Gallagher CT, Mehta AN, Selvan R, Mirza IB, Radia P, Bharadia NS, Hitch G. Perceived stress levels among undergraduate pharmacy students in the UK. Curr Pharm Teach Learn, 2014; 6(3):437–41; doi:doi:10.1016/j.cptl.2014.02.004 CrossRef
Hakami RM. Prevalence of psychological distress among undergraduate students at Jazan University: A cross-sectional study. Saudi J Med Med Sci, 2018; 6(2):82–8; doi:10.4103/sjmms.sjmms_73_17 CrossRef
Halboub E, Alhajj MN, AlKhairat AM, Sahaqi AM, Quadri MFA. Perceived stress among undergraduate dental students in relation to gender, clinical training and academic performance. Acta Stomatol Croat, 2018; 52(1):37–45; doi:10.15644/asc52/1/6 CrossRef
Hambisa MT, Derese A, Abdeta T. Depressive symptoms among Haramaya University students in Ethiopia: a cross-sectional study. Dep Res Treat, 2020; 1–9; doi: 10.1155/2020/5027918 CrossRef
Henning K, Ey S, Shaw D. Perfectionism, the imposter phenomenon and psychological adjustment in medical, dental, nursing and pharmacy students. Med Educ, 1998; 32(5):456–64. CrossRef
Hollyman J. Fighting for mental health: A personal view. Sartorius, N. Cambridge University Press, Cambridge, UK, p 266, 2002; doi:http://dx.doi.org/10.1136/jnnp.74.7.1010-a CrossRef
Ibrahim N, Al-Kharboush D, El-Khatib L, Al-Habib A, Asali D. Prevalence and predictors of anxiety and depression among female medical students in King Abdulaziz University, Jeddah, Saudi Arabia. Iran J Public Health, 2013; 42(7):726–36.
Javadi M, Jourabchi Z, Shafikhani AA, Tajik E. Prevalence of depression and anxiety and their association with body mass index among high school students in Qazvin, Iran, 2013–2014. Electron Physician, 2017; 9(6):4655–60; doi:10.19082/4655 CrossRef
Khalid S, Bukhari A, Azhar S, Saeed N, Manzoor S, Syed H, Khan FM, Syed A, Ali SA, Ali M, Kamboh MS. Incidence of depression and the coping styles used for it by under graduate and post graduate pharmacy students: a comparison. J Hum Virol Retrovirol, 2017;5(2):1-5.doi: 10.15406/jhvrv.2017.05.00146 CrossRef
Kulsoom B, Afsar NA. Stress, anxiety, and depression among medical students in a multiethnic setting. Neuropsychiatr Dis Treat, 2015; 11:1713–22; doi:10.2147/NDT.S83577 CrossRef
Lovibond SH, Lovibond PF. 1995. Manual for the depression anxiety stress scales. 2nd edition, Pscyhology Foundation, Sydney, Australia. Available via https://trove.nla.gov.au/work/30421447 CrossRef
Macauleya K, Plummerb L, Bemisb C, Brockb G, Larsonb C, Spanglerb J. Prevalence and predictors of anxiety in healthcare professions students. Health Prof Educ, 2018; 4(3):176–85. CrossRef
Mane Abhay B, Krishnakumar MK, Niranjan Paul C, Hiremath Shashidhar G. Differences in perceived stress and its correlates among students in professional courses. J Clin Diag Res, 2011; 5(1):1228–33.
Mao Y, Zhang N, Liu J, Zhu B, He, R., Wang X. A systematic review of depression and anxiety in medical students in China. BMC Med Educ, 2019; 19:327; doi: 10.1186/s12909-019-1744-2 CrossRef
McDowell I. Measuring health: a guide to rating scales and questionnaires, 3rd edition, Oxford University Press, New York, NY, 2006.
Ministry of Education. Saudi Gazette Report: 67% Saudi medical students suffer due to stress. Available via http://saudigazette.com.sa/article/519378 (Accessed 15 October 2017).
Moayedi F, Bastami MM, Ashouri FP, Hamadiyan H, Rasekhi S. Comparison of sources and severity of perceived stress between paramedical and medical students. Int J Med Res Health Sci, 2016; 5(6):183–90.
Niemi PM, Vainiomäki PT. Medical students’ distress quality, continuity and gender differences during a six-year medical programme. Med Teach, 2006; 28(2):136–41. CrossRef
Oermann MH. Differences in clinical experiences of and and BSN students. J Nurs Educ, 1998; 37(5):197–201. CrossRef
Omigbodun OO, Odukogbe AT, Omigbodun AO, Yusuf OB, Bella TT, Olayemi O. Stressors and psychological symptoms in students of medicine and allied health professions in Nigeria. Soc Psychiatry Psychiatr Epidemiol, 2006; 41(5):415–21; doi:10.1007/s00127-006-0037-3 CrossRef
Patel V, Saxena S, Lund C, Thornicroft G, Baingana F, Bolton P, UnÜtzer J. (2018). The Lancet Commission on global mental health and sustainable development. Lancet, 2018; 392(10157):1553–98; doi:10.1016/S0140-6736(18)31612-X CrossRef
Quek TT, Tam WW, Tran BX, Zhang M, Zhang Z, Ho CS, Ho RC. The Global prevalence of anxiety among medical students: a meta-analysis. Int J Environ Res Pub Health, 2019; 16(15):E2735; doi:10.3390/ijerph16152735 CrossRef
Ritchie H, Roser M. 202“. “Mental Health”. Published online at OurWorldInData.org. Available via https://ourworldindata.org/mental-health (Accessed 08 January 2019).
Tripathi R, Albarraq AA, Makeen HA, Alqahtani SS, Tripathi P, Pancholi SS. Knowledge and perceptions of antimicrobial stewardship program among health-care students in Saudi Arabia. Saudi J Health Sci, 2020; 9(2):122–9; doi:10.4103/sjhs.sjhs_192_19 CrossRef
Votta RJ, Benau EM. Predictors of stress in doctor of pharmacy students: results from a nationwide survey. Curr Pharm Teach Learn, 2013; 5(5):365–72; doi:10.1016/j.cptl.2013.06.014 CrossRef
Waghachavare VB, Dhumale GB, Kadam YR, Gore AD. A Study of stress among students of professional colleges from an urban area in India. Sultan Qaboos Univ Med J, 2013; 13(3):429–36. CrossRef
World Health Organization. Mental health action plan 2013–2020. WHO, Geneva, Switzerland, 2013. Available via https://www.who.int/mental_health/publications/action_plan/en/ (Accessed 18 October 2018).
Yusoff MS, Abdul Rahim AF, Baba AA, Ismail SB, Mat Pa MN, Esa AR. Prevalence and associated factors of stress, anxiety and depression among prospective medical students. Asian J Psychiatr, 2013; 6(2):128–33; doi:10.1016/j.ajp.2012.09.012 CrossRef