INTRODUCTION
Obesity is a global health issue that is continuously increasing in prevalence rate throughout the world, being the highest in the United States (Arroyo-Johnson et al., 2016). According to the American Heart Association statistics in 2015, 35.1% of adults in the USA were obese (Eanes, 2015). Obesity is defined as a body mass index (BMI) of 30 kg/m2 or more (Apovian, 2016). It is affected by a cluster of genetic, socioeconomic, and cultural factors (Omer, 2020a). According to the WHO estimates of 2010, the prevalence of obesity was 38% in females compared to 20% in males. Obesity is a risk factor for several diseases such as hypertension, type 2 diabetes mellitus (DM), and heart diseases (Fruh, 2017). It increases the risk of morbidity and mortality, and it has a detrimental effect on the overall public health and economic cost to the health system (Omer, 2020b). In Jordan, the prevalence of obesity is high and has shown an increasing tendency in the last few years. The prevalence rate was 20% and 32% in males and females, respectively, according to the WHO estimates of 2010 (Badran et al., 2011). Among adolescents, the prevalence rate of obesity was reported in a previous study to be 6.2% (Al-Rahamneh, 2020). A recent study reported that the rate of prevalence had increased to 75.6% and 60.4% in female and male adults, respectively, compared to a prevalence rate of 53.1% and 28.1% in women and men, respectively, in 2008 in the same country (Ajlouni et al., 2020).
There are many strategies for controlling and management of obesity. Lifestyle changes, including a healthy diet, exercise, and behavioral therapy, can be considered the mainstay of obesity management. Other options available are treatment using drugs, surgery, or medical devices for patients who do not respond to lifestyle interventions (Kahan, 2016). For effective weight loss, one of the approaches is a healthy diet combined with moderate physical activity (at least 150 minutes per week) (Bray et al., 2016). According to obesity guidelines recommendations, a 6-month program of physical activity with low-calorie intake can achieve a weight loss of up to 8% of the program’s start weight which should be followed by a one-year maintenance program in order to prevent weight regain (Wadden et al., 2020).
On the other hand, bariatric surgery is suggested as the most suitable option after the failure of all other interventions. The major obstacle expected after surgery is the need for lifelong nutritional supplements (Ruban et al., 2019). Although several drugs were approved by the Food and Drug Administration (FDA) for the treatment of obesity, orlistat is the only approved medication for the treatment of obesity in children (Londoño-Lemos, 2018).
Another drug that has begun to be more popular for its benefit in weight reduction is metformin. Metformin is structurally a biguanide (1,1-dimethylbiguanide hydrochloride) and is an old synthesized medication using a structurally similar natural compound found in the traditional antidiabetic plant Galega officinalis, better known as French lilac. Metformin has been used in the management of DM as the first line of therapy for a long time (Zhou et al., 2018). Other than its use in the management of DM, several studies have shown that metformin can be used in the treatment of many other pathological conditions, including cancer, obesity, hepatic diseases, renal diseases, and heart diseases (Lv et al., 2020). The pharmacological activity of metformin is based on multiple mechanisms, such as reduction of glucose synthesis, activation of AMP-activated protein kinase through affecting intracellular Adenosine triphosphate (ATP): Adenosine diphosphate (ADP) ratio (ATP/ADP), or inhibition of mitochondrial function (Rena et al., 2017). Metformin works by decreasing the synthesis of hepatic glucose. In order to enter cells and produce this effect, metformin needs membrane transport proteins which are encoded by specific genes. The variations in these genes among ethnic groups affect the pharmacokinetics and pharmacodynamics of metformin which determines a patient’s response to metformin (Al-Eitan et al., 2019). The proposed mechanism of metformin efficacy in weight loss is due to its alteration in the appetite regulatory center, the intestine microbiome, as well as in the reversal of aging complications (Yerevanian et al., 2019).
Several studies revealed the effectiveness of metformin in weight loss due to its role in increasing the activity of growth/differentiation factor 15 which is known to reduce weight by reducing food intake (Coll et al., 2020). In addition, metformin has several effects on other endogenous chemicals and biological processes within the body, including leptin, and insulin sensitivity, oxidation, and storage of fat in different body tissues (Malin et al., 2014). A literature review reported heterogeneity in weight reduction induced by metformin. Some studies reported a 2.5–3 kg reduction in weight during approximately 3–4 years compared to the placebo group. On the other hand, weight loss of 2.6 kg was observed 18 months later in the metformin group, while slight nonsignificant weight loss was noted after 12 weeks (Solymár et al., 2018).
In Jordan, alternative medicine is widely used for weight loss. It includes dietary and herbal supplements, as well as consuming local traditional plants and drinking plant-based hot beverages (Shehadeh et al., 2020).
Although comparisons of these different approaches to weight loss, including herbs, diets, exercise, and dietary supplements, have been discussed by several researchers, none of these reports focused on the use of metformin as an option for weight loss (Al-Safi et al., 2008; Issa, 2018). Hence, the aim of the present study was to assess the attitudes and behavior of the Jordanian public toward weight loss and to compare their practices in weight loss with a special emphasis on participants’ beliefs of and experiences with the ability of metformin to decrease weight and/or to manage their obesity.
MATERIALS AND METHODS
A cross-sectional, questionnaire-based study was conducted in the Jordanian community during the period of November 2020 to February 2021. The questionnaire was designed by the authors following a comprehensive literature review about different approaches used for weight gain and obesity management including metformin use in weight loss. The questionnaire was distributed using Google Forms. A total of 574 questionnaire responses were received to assess the participants’ behavior and approaches in weight gain management by focusing on metformin as an option for weight loss
The questionnaire contained four parts. The first part is an interface that clarifies the purpose of the study and confirms the confidentiality of information. The second part contains the participants’ demographic data questions, such as age and weight. The third part contains questions related to the participants’ approaches to weight loss. The last part is related to Jordanians’ experiences during their use of metformin, mainly in weight loss.
To acquire more insight into the details regarding weight gain management and the effect of metformin use among the Jordanian population, the participants were classified into two main groups: metformin users and non-metformin users, as illustrated in the following chart.
 | Flow chart: Selection of Study Participants. [Click here to view] |
It should be pointed out that bariatric surgery was not included in the present study as an option for weight loss since it is indicated mainly either for people with morbid obesity with BMI ≥ 40 or for obese people with BMI ? 35 (Piche et al., 2015). All study data were obtained as percentages and frequencies. IBM SPSS (version 22) was used to compute percentages and frequencies in addition to creating graphs. The study was approved by the Ethics Committee of the Al-Balqa Applied University (Approval No. 26/3/1/276). The submission of completed questionnaires by the responders was considered consent to participate in the study.
RESULTS
Data were analyzed from 574 responses. The sociodemographic data of the participants are shown in Table 1. The majority of the participants (96.1%) were Jordanians. Female participants were more (78.9%) than male participants (21.1%), of whom 63.6% were married. More than half of the participants were above 35 years old (56.5%) and held bachelor’s degrees (53%). More than two-thirds of the participants were urban residents (76.6%), while the rest were suburb and rural residents (23.4%).
 | Table 1. Sociodemographic data of the participants (N = 574). [Click here to view] |
Weight loss management approaches reported by Jordanians
It was found that 78.2% of the participants were overweight, of whom 10.3% had DM and 22% had other chronic diseases such as hypertension and hypothyroidism. More than half of the participants reported that weight gain resulted from lack of exercise (51.2%), while 42.7% attributed the gain in weight due to consuming too much food rich in fat and sugars and 14.5% believed it is inherited. Other less common causes included polycystic ovary syndrome (10.1%), hypothyroidism (7.8%), and the use of certain medications (3.7%).
Among the approaches Jordanian people adopted for their control of weight gain were diet (64.8%), exercise (47.7%), herbal use (20.2%), use of medications (16.6%), and use of dietary supplements for weight loss (12.4%). In particular, it was found that less than half of all participants (40.6%) used metformin for different causes, while 59.4% did not use metformin.
Weight loss management by non-metformin users
Figure 1 shows that 69.5% of the non-metformin users were overweight, with 0.9% suffering from DM and 14.9% from other chronic diseases. The most common causes of weight gain in this group included lack of exercise, eating too much food rich in fat and sugars, and inheritance (46.9%, 37.5%, and 10.3%, respectively). More than half (54%) followed a diet to manage weight loss, while 45.7% practiced exercising. On the other hand, a lesser percentage used herbs and dietary supplements (13.2% and 7.0%, respectively). Only a small percentage of participants in this group used medications other than metformin for weight loss (5.3%).
The source of medical information among the participants of this group was mainly from relatives/friends (30.8%), followed by social media (30.5%), while healthcare providers represented 30.5% as a source of information (14.1% and 16.4% for doctors and pharmacists, respectively).
Weight loss management by metformin users
It was found that less than half of all participants (40.6%) used metformin mainly for the treatment of other existing ailments other than weight gain. The majority of this group (91%) were overweight, 24% of them reported having DM, while 32.2% had other chronic diseases.
Interestingly, the common causes of weight gain in this group were similar to the non-metformin users. These included the lack of exercise and eating too much food rich in fat and sugars, in addition to the prevalence of different diseases such as polycystic ovaries and hypothyroidism, in addition to inheritance (53.6%, 48.1%, 23.2%, 11.6%, and 20.2%, respectively). The majority of metformin users (79%) followed a diet for weight loss, while 48.9% practiced exercising. On the other hand, lower percentages used medications, herbs, and dietary supplements. The source of information about metformin benefits in weight loss among users was mainly doctors (48.1%) and relatives and friends (32.2%), followed by pharmacists (24.9%) and the experience of previous patients (21.9%) (Fig. 2).
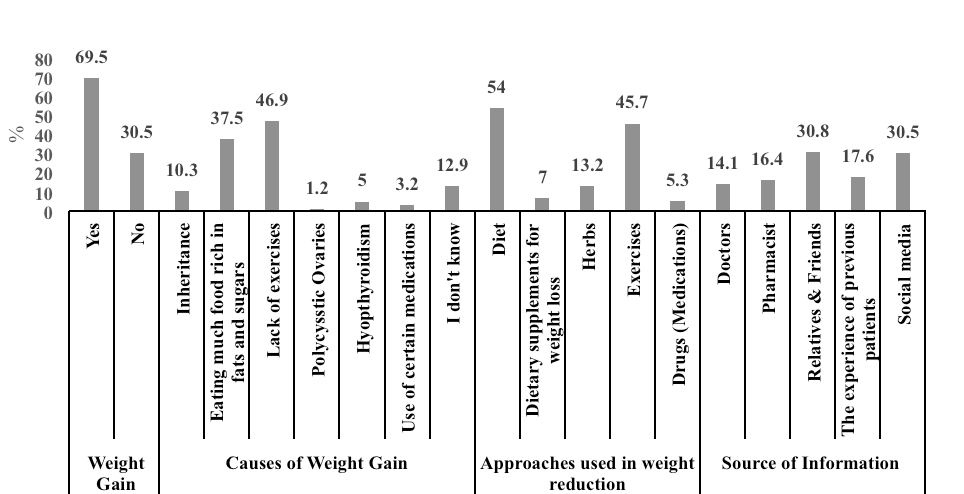 | Figure 1. Percent frequency distribution of reasons behind weight gain, approaches in controlling weight gain and, source of information related to weight gain management among non–Metformin users. [Click here to view] |
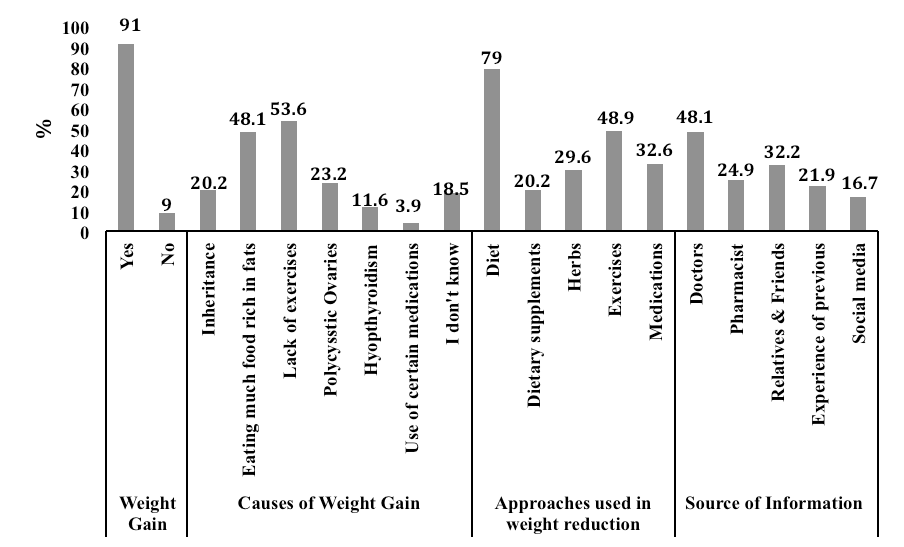 | Figure 2. Percent frequency distribution of reasons behind weight gain, approaches in controlling weight gain and source of information related to weight gain management among Metformin users. [Click here to view] |
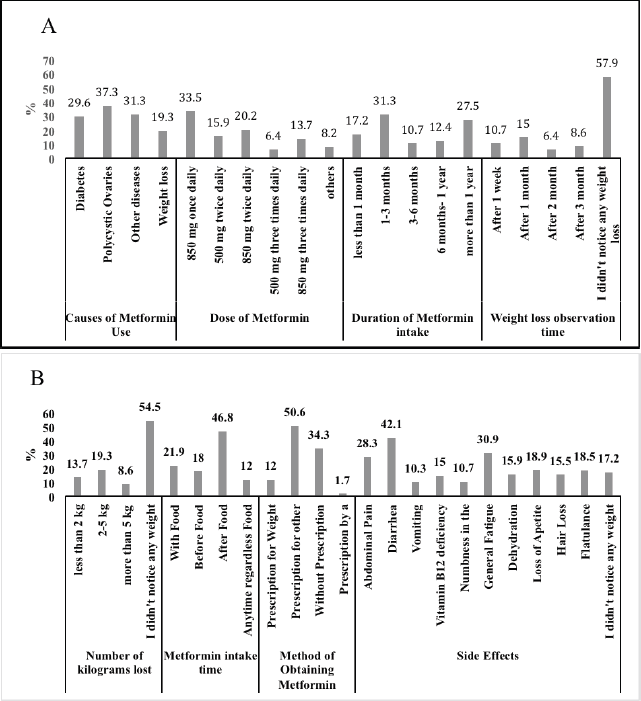
Figure 3 shows the frequency analysis of the data related to metformin users. Polycystic ovary disease was the most common cause of metformin use by this group (37.7%), followed by DM (29.6%), and only 19.3% used it for weight loss management.
The most widely used dose regimen was 850 mg daily (33.5%) for 1–3 months’ duration (31.3%), and 46.8% of metformin users took it after food. Approximately 40% noticed weight loss in different ranges of kilograms at different durations of time, while more than half of the users (54.5%) did not notice any weight loss. 32.2% used diet while using metformin for weight loss compared to 50.2% who used exercise in combination with metformin for control of weight. Figure 4 shows that 48% of the study participants observed a decrease in weight ranging from less than 2 up to 5 kg when metformin use was combined with diet, whereas 46% of the participants’ responses showed a decrease in weight ranging from less than 2 up to 5 kg when metformin use was combined with exercise. Specifically, the pronounced weight loss in the range of 2–5 kg was observed by 32% who combined metformin with exercise compared to 17% who combined metformin with diet.
 | Figure 3. Knowledge regarding Metformin Use. A–shows frequency distribution in causes of uses, dose and duration of metformin, and weight loss observation time. B–Number of kilograms lost, metformin intake time, method of obtaining metformin, and side effects in metformin users. [Click here to view] |
Among the participants of this group, 50.6% received it as a prescription for the treatment of other diseases, and only 12% received it as a prescription for weight loss. Diarrhea and general fatigue are the most common side effects experienced by metformin users (42.1% and 30.9%, respectively), followed by abdominal pain (28.3%), loss of appetite (18.9%), and flatulence (18.5%).
DISCUSSION
Obesity is a global health problem that may increase the risk of several diseases such as hypertension, DM, and other heart diseases (Arroyo-Johnson et al., 2016; Fruh, 2017). It is associated with high morbidity and mortality rate (Omer, 2020b). Different approaches used to manage obesity include lifestyle changes, drugs, and surgery (Kahan, 2016). In the present study, the attitudes and behavior of the Jordanian population toward weight gain and obesity management were assessed.
This study revealed different approaches used by Jordanians for weight loss, including diet and exercise (64.8% and 47.7%, respectively). These findings were approximately similar to those reported in a previous study conducted on Jordanian university students, in which 76.6% followed a specific diet plan and 64.9% did exercise to control weight gain (Issa, 2018). The importance of nonpharmacological/invasive techniques in managing obesity has been highlighted also by Higuera-Hern et al. (2018). In addition to diet and exercise, the researchers reported the use of cognitive-behavioral intervention and transcranial direct current stimulation as noninvasive techniques which can be performed under medical supervision (Higuera-Hernández et al., 2018).
 | Figure 4. knowledge regarding Combining Metformin with Exercise & diet. A –Weight change after combining metformin and exercises. B–Weight change after combining metformin and Diet. [Click here to view] |
The current study showed that a low percentage (20.2%) of Jordanians using herbs for weight loss despite the previously reported studies showing the increased use of herbal medicines among Jordanians for the treatment of multiple diseases/conditions (53.3%), including weight loss (23.6%) (Abdel-Qader et al., 2020). The effectiveness of herbal medicine has been reviewed by Liu et al. (2017). They reported that huge progress had been made in the study of weight loss therapy with herbal medicines in the last 10 years, evidenced by pharmacological and clinical investigations of herbal medicine in the treatment of obesity (Liu et al., 2017).
Medications, specifically metformin, are another approach used by Jordanians for weight loss, although its use in the recent study was low. Other medications, such as orlistat, were not covered by our study because orlistat was already approved by the FDA for weight loss (Londoño-Lemos, 2018), and a literature review reported its effectiveness in reducing blood sugar, lipids, and blood pressure (Khalil et al., 2020).
In the present study, females represented the majority of metformin users. This can be justified and explained since metformin is used in the treatment of PCOS, which is considered a major endocrine disease occurring in females during their reproductive age (Abu-Taha et al., 2020). Metformin is recommended for these patients due to its lowering effect on testosterone levels (Sam and Ehrmann, 2017). In addition, metformin was used by females for the management of obesity which is more common among Jordanian females and exhibited an increasing tendency, especially in 2020 (Ajlouni et al., 2020). In the current study, a third of metformin users noticed weight loss of up to 5 kg. More than half of them had chronic diseases including DM in which metformin is considered the first line of therapy (Zhou et al., 2018). This finding is supported by previous studies that reported the effect of metformin in weight loss in patients with DM and other comorbidities (Diabetes Prevention Program Research Group, 2012). In a meta-analysis conducted in 2020, several clinical trials showed the effect of metformin in obesity treatment. Metformin decreased BMI moderately, and the weight loss was significant in patients with BMI ? 35 (Pu et al., 2020). In another meta-analysis study conducted in 2018 which included 971 articles, 6 placebo control studies on diabetic elderly patients showed weight reduction in the metformin-treated group compared to the metformin-nontreated group (Solymár et al., 2018).
The effect of diet and exercise on weight loss could not be ignored since the participants’ responses demonstrated the efficiency of the combined use of specific diets and exercise in addition to metformin for weight loss. This finding is supported by previous studies that reported the efficacy of metformin use in addition to a low-calorie diet in reducing body weight compared to the use of a low-calorie diet only (Ejtahed et al., 2019; Kay et al., 2001). Still, there are further studies emphasizing the superiority of lifestyle changes in weight loss compared to metformin use (Lim et al., 2011).
According to the current study, the participants’ responses presented weight loss at different doses where the most widely used dose regimen by metformin users was 850 mg once daily, followed by 850 mg twice daily and 500 mg twice daily. Similarly, previous studies reported the efficacy of metformin in weight loss at different dosage regimens, such as dosage regimens of 850 mg twice daily and 500 mg twice daily (Diabetes Prevention Program Research Group, 2012; Ejtahed et al., 2019; Kay et al., 2001). Previous studies have shown variation in the weight loss range that metformin causes and the duration of its use until its effect appears. Some studies reported a weight loss range of 5.8 ± 7 kg after six months’ duration of use (Seifarth et al., 2013), while Hanieh-Sadat Ejtahed et al. (2019) reported a weight loss of 4.5% in BMI after two months’ duration of use (Ejtahed et al., 2019).
According to the published literature, metformin does not seem to operate similarly or ideally in all individuals due to variances in their genetic profiles, resulting in a decrease in its efficacy (Al-Eitan et al., 2019). A previous study in Jordan reported the effect of genetic variation on the pharmacokinetics of metformin and so the response of the human body to that drug (Hakooz et al., 2017).
The side effects reported by the patients were similar to those mentioned in the literature as common side effects observed following metformin intake. Diarrhea, fatigue, abdominal pain, and loss of appetite were the most common side effects (Al-Qallaf, 2016; Ghosal et al., 2019). Comparing these adverse effects with other weight control medications, such as orlistat, lorcaserin, and liraglutide, one can assume that metformin is a safe drug provided the user follows the correct regimen under medical supervision (Van Gaal et al., 2016).
More than half of participants (64.3%) in the present study received metformin by prescription either for weight loss or for the treatment of other diseases, while 34.3% of metformin users received it without a prescription for control. This can be attributed to the strong effect of relatives and friends as well as social media on the choice of treatment for controlling weight gain. Burke et al. (2011) reported the importance of behavioral self-monitoring in dietary intake and physical activity so that individuals are aware of their eating habits. They concluded that consistent self-monitors of exercise experienced significantly greater weight loss and improved their exercising frequencies. This can be achieved by using a traditional paper diary, mobile applications, and exercise groups (Burke et al., 2011).
In conclusion, most of the Jordanians in the current study selected diet and exercise for obesity management. Furthermore, there were different responses to metformin on different dose regimens in patients suffering from chronic diseases who used metformin compared to those who used metformin as a medication to treat obesity. Moreover, interindividual response variation to metformin was observed among Jordanians earlier. Consequently, further clinical studies are needed to evaluate metformin’s exact role in weight reduction. The present study suggests that great attention should be paid to the problem of overweight and obesity among the Jordanian population. It highlights the role that the public health authorities should take part in conducting awareness campaigns through media and other channels to point out the risks of overweight and obesity on individuals’ health.
CONFLICTS OF INTEREST
The authors declare no conflicts of interest.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
FUNDING
There is no funding to report.
ETHICAL APPROVALS
Al-Balqa Applied University (Approval No. 26/3/1/276).
DATA AVAILABILITY
All data generated and analyzed are included within this research article.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Abdel-Qader DH, Albassam A, Ismael NS, Aljamal MS, Chen LC, Mansoor K, Hamadi S, Al Mazrouei N, Al Meslamani AZ. Herbal medicine use in the Jordanian population: a nationally representative cross-sectional survey. J Pharm Pharmacogn Res, 2020; 8:525–36.
Abu-Taha M, Daghash A, Daghash R, Abu Farha R. Evaluation of women knowledge and perception about polycystic ovary syndrome and its management in Jordan: a survey-based study. Int J Clin Pract, 2020; 74(10):e13552. CrossRef
Ajlouni K, Khader Y, Batieha A, Jaddou H, El-Khateeb M. An alarmingly high and increasing prevalence of obesity in Jordan. Epidemiol Health, 2020; 42:e2020040. CrossRef
Al-Eitan LN, Almomani BA, Nassar AM, Elsaqa BZ, Saadeh NA. Metformin pharmacogenetics: effects of SLC22A1, SLC22A2, and SLC22A3 polymorphisms on glycemic control and HbA1c levels. J Pers Med, 2019; 9(1):17. CrossRef
Al-Qallaf, S. M. Efficacy and safety of metformin in weight loss in Bahraini population. J Appl Pharm Sci, 2016; 6(6):91–5. CrossRef
Al-Rahamneh, H. The prevalence of obesity, overweight, and thinness among Jordanian children and adolescents. J Exercise Physiol Online, 2020; 23(2):95–108.
Al-Safi SA, Ayoub NM, Ayoub AM, Al-Momany E, Al-Doghim I, Al-Balas M, Alkofahi A, Aboul-Enein FH, Aboul-Enein BH. Public awareness of the abuse of herbs and drugs to decrease body weight: a novel national survey in Jordan. J Public Health, 2008; 16(3):205–13. CrossRef
Apovian C. Obesity: definition, comorbidities, causes, and burden. Am J Manag Care, 2016; 22(7 Suppl): s176–85.
Arroyo-Johnson C, Mincey K. Obesity epidemiology worldwide. Gastroenterol Clin, 2016; 45(4):571–9.
Badran M, Laher I. Obesity in Arabic-speaking countries. J Obes, 2011; 2011:686430. CrossRef
Bray GA, Frühbeck G, Ryan DH, Wilding JP. Management of obesity. Lancet, 2016; 387(10031):1947–56; doi: 10.1016/S0140-6736(16)00271-3 CrossRef
Burke LE, Wang J, Sevick MA. Self-monitoring in weight loss: a systematic review of the literature. J Am Diet Assoc, 2011; 111(1):92–102. CrossRef
Coll AP, Chen M, Taskar P, Rimmington D, Patel S, Tadross JA, Patel S, Tadross JA, Cimino I, Yang M, Welsh P, Virtue S, Goldspink DA, Miedzybrodzka EL, Konopka AR, Esponda RR, Huang JT, Tung YCL, Rodriguez-Cuenca S, Tomaz RA, Harding HP, Melvin A, Yeo GSH, Preiss D, Vidal-Puig A, Vallier L, Nair KS, Wareham NJ, Ron D, Gribble FM, Reimann F, Sattar N, Savage DB, Allan BB, O’Rahilly S. GDF15 mediates the effects of metformin on body weight and energy balance. Nature, 2020; 578(7795):444–48; doi: 10.1038/s41586-019-1911-y CrossRef
Diabetes Prevention Program Research Group. Long-term safety, tolerability, and weight loss associated with metformin in the Diabetes Prevention Program Outcomes Study. Diabetes Care, 2012; 35(4):731–7. CrossRef
Eanes L. Obesity a persistent global health problem. Int Arch Nurs Health Care, 2015; 1:1–3. CrossRef
Ejtahed HS, Tito RY, Siadat SD, Hasani-Ranjbar S, Hoseini-Tavassol Z, Rymenans L, Verbeke K, Soroush AR, Raes J, Larijani B. Metformin induces weight loss associated with gut microbiota alteration in non-diabetic obese women: a randomized double-blind clinical trial. Eur J Endocrinol, 2019; 180(3):165–76. CrossRef
Fruh, S. M. Obesity: risk factors, complications, and strategies for sustainable long-term weight management. J Am Assoc Nurse Pract, 2017; 29(S1):S3–14. CrossRef
Ghosal S, Ghosal S. The side effects of metformin—a review. J Diabetes Metab Disord, 2019; 6:030. CrossRef
Hakooz N, Jarrar YB, Zihlif M, Imraish A, Hamed S, Arafat T. Effects of the genetic variants of organic cation transporters 1 and 3 on the pharmacokinetics of metformin in Jordanians. Drug Metab Pers Ther, 2017; 32(3):157–62. CrossRef
Higuera-Hernández MF, Reyes-Cuapio E, Gutiérrez-Mendoza M, Rocha NB, Veras AB, Budde, H, Jesse J, Zaldívar-Rae J, Blanco-Centurión C, Machado S, Murillo-Rodríguez E. Fighting obesity: non-pharmacological interventions. Clin Nutr ESPEN, 2018; 25:50–5. CrossRef
Issa R. Research article use of herbal remedies, conventional medicine, diet and exercise for weight loss: case study of university students in Jordan. Pak J Nutr, 2018; 17:76–88. CrossRef
Kahan S. Overweight and obesity management strategies. Am J Manag Care, 2016; 22:S186–96.
Kay JP, Alemzadeh R, Langley G, D’angelo L, Smith P, Holshouser S. Beneficial effects of metformin in normoglycemic morbidly obese adolescents. Metab Clin Exp, 2001; 50(12):1457–61. CrossRef
Khalil H, Ellwood L, Lord H, Fernandez R. Pharmacological treatment for obesity in adults: an umbrella review. Ann Pharmacother, 2020; 54(7):691–705; doi: 10.1177/1060028019898912 CrossRef
Lim SS, Norman RJ, Clifton PM, Noakes M. The effect of comprehensive lifestyle intervention or metformin on obesity in young women. Nutr Metab Cardiovasc Dis, 2011; 21(4):261–68. CrossRef
Liu Y, Sun M, Yao H, Liu Y, Gao R. Herbal medicine for the treatment of obesity: an overview of scientific evidence from 2007 to 2017. Evid Based Complement Altern Med, 2017; doi: 10.1155/2017/8943059. CrossRef
Londoño-Lemos ME. Pharmacological advances to the treatment of obesity. J Child Obes, 2018; 3(1):3; doi:10.21767/2572-5394.100043 CrossRef
Lv Z, Guo Y. Metformin and its benefits for various diseases. Front Endocrinol, 2020; 11:191.
Malin SK, Kashyap SR. Effects of metformin on weight loss: potential mechanisms. Curr Opin Endocrinol Diabetes Obes, 2014; 21(5):323–9; doi: 10.1097/MED.0000000000000095 CrossRef
a Omer T. The causes of obesity: an in-depth review. Adv Obes Weight Manag Control, 2020; 10(4):90–4. CrossRef
b Omer T. The health and economic impacts of obesity. Adv Obes Weight Manag Control, 2020; 10(4):96–8. CrossRef
Piche ME, Auclair A, Harvey J, Marceau S, Poirier P. How to choose and use bariatric surgery in 2015. Canad J Cardiol, 2015; 31(2):153–66. CrossRef
Pu R, Shi D, Gan T, Ren X, Ba Y, Huo Y, Bai Y, Zheng T, Cheng N. Effects of metformin in obesity treatment in different populations: a meta-analysis. Ther Adv Endocrinol Metab, 2020; 11:2042018820926000. CrossRef
Rena G, Hardie DG, Pearson ER. The mechanisms of action of metformin. Diabetologia, 2017; 60(9):1577–85. CrossRef
Ruban A, Stoenchev K, Ashrafian H, Teare J. Current treatments for obesity. Clin Med, 2019; 19(3):205. CrossRef
Sam S, Ehrmann DA. Metformin therapy for the reproductive and metabolic consequences of polycystic ovary syndrome. Diabetologia, 2017; 60(9):1656–61. CrossRef
Seifarth C, Schehler B, Schneider HJ. Effectiveness of metformin on weight loss in non-diabetic individuals with obesity. Exp Clin Endocrinol Diabetes, 2013; 121(01):27–31. CrossRef
Shehadeh MB, Suaifan G, Abu-Odeh A, Darwish R. Complementary and alternative medicine use for weight management among females in Jordan: a community-based survey. East Mediterran Health J, 2020; 26(4). CrossRef
Solymár M, Ivic I, Pótó L, Hegyi P, Garami A, Hartmann P, Pétervári E, Czopf L, Hussain A, Gyöngyi Z, Sarlós P, Simon M, Mátrai P, Bérczi B, Balaskó M. Metformin induces significant reduction of body weight, total cholesterol and LDL levels in the elderly—a meta-analysis. PLoS One, 2018; 13(11):e0207947. CrossRef
Van Gaal L, Dirinck E. Pharmacological approaches in the treatment and maintenance of weight loss. Diabetes Care, 2016; 39(Supplement 2):S260–67. CrossRef
Wadden TA, Tronieri JS, Butryn ML. Lifestyle modification approaches for the treatment of obesity in adults. Am Psychol, 2020; 75(2):235; doi: 10.1037/amp0000517 CrossRef
Yerevanian A, Soukas AA. Metformin: mechanisms in human obesity and weight loss. Curr Obes Rep, 2019; 8(2):156–64. CrossRef
Zhou J, Massey S, Story D, Li L. Metformin: an old drug with new applications. Int J Mol Sci, 2018; 19(10):2863. CrossRef