INTRODUCTION
Asthma is a recurrent condition that poses a significant public health issue in both developing and developed countries, affecting more than 300 million individuals globally (Reddel et al., 2015). Asthma is a significant result of morbidity, poor quality of life, and higher healthcare costs; nevertheless, in most parts of the world, its diagnosis and care remain insufficient, especially in low-income regions (Becker and Abrams, 2017, Mirzaei et al., 2017).
The incidence and development of asthma in a child is very much based on their age; in fact, the age of onset and the present age is more predictive of symptom severity than environmental factors. Geographically, asthma is less prevalent in the Middle East than in western nations (range: 4.4%–7.6%) (Tarraf et al., 2018).
In Palestine, an intermediate incidence (3.8%) was identified, but an increased incidence of recent wheezing was reported (8.9%). Similar results were observed in neighboring nations, such as Jordan (incidence of 4.1% for asthma, 8.3% for wheezing) (Kenyon et al., 2015).
Asthma that is uncontrolled in a developing child may have major implications on the development in psychological, mental, and physical respects (Rydström et al., 2005). They may also face social restrictions such as being unable to take part in a sleepover due to the chance of having an asthma attack or they may have friends with pets that could provoke an asthma attack. In addition to the global health burden that asthma represents, it also poses many social and community restrictions in the context of an individual child’s life (Gandhi et al., 2013).
Thus, investigating parental knowledge and education against their children during and between asthmatic attacks is critical in order to avoid and manage such attacks as well as prevent further distress in those children.
This is the first study that evaluates the quality of asthma control in pediatric patients and their parents’ awareness about the disease in Palestine and is also one of few such studies in the world.
METHODS
Setting
This was a descriptive, cross-sectional, and analytical clinical study carried out at the Ministry of Health Primary Healthcare Units in Ramallah and Hebron. We included all children and adolescents diagnosed with asthma.
Study sample
The study population was comprised of children and adolescents between the ages of 6 and 17 who had been diagnosed with asthma by a specialist at least 6 months prior to enrollment in order to determine whether or not their asthma was under control. The pediatric patients and their primary caregivers were recruited from two major governmental outpatient clinics located in Ramallah and Hebron within the period from November 2020 to March 2021.
At least 120 participants were required to ensure 80% power (at two-sided α = 0.05) to detect a minimum significant difference of 1.5 points (SD 3.1) in asthma score between controlled and uncontrolled patient groups. A total of 150 patients were sought to be recruited, allowing 20% dropped outpatients, yielding a final count of 120 participants. More patients were approached in this study and the actual number recruited in this study was 132 patients.
Inclusion criteria
We included children (6–17 years old) who had been diagnosed by a specialist at least 6 months before enrolling in the study in order to allow adequate time to determine whether or not the children’s asthma was under control or not, and not having any other chronic medical condition in their history.
Exclusion criteria
We excluded children under 6 years or older than 17 years, children presenting with acute deterioration of asthma at the time of enrolment, and children having difficulty understanding the questionnaire.
Diagnosis of asthma and severity
Asthma diagnosis and severity were assessed by a respiratory consultant based on the Global Initiative for Asthma, by examining the FEV1, symptoms, nocturnal awakenings, use of rescue medication, and activity restriction. The variable expiratory airflow limitation and a history of respiratory symptoms such as wheezing, shortness of breath, chest tightness, and coughing that change over time and in intensity are the two main characteristics that distinguish asthma.
Thus, three categories of asthma patients were created: mild asthma, moderate asthma, and severe asthma.
Ethical approval
Ethical approval was obtained from the Research Ethical Committee at Al-Quds University [Ref No: 164/REC/2020]. Study authorization for data collection was gained from the Palestinian Ministry of Health in Ramallah and Hebron. Nurses contacted the patients’ caregivers in the waiting area prior to their planned appointments. An explanation of the study was provided to each patient and their parents (father or mother), and a written consent form was given to each caregiver. Each child gave verbal consent, along with the information that they could refuse to participate, could reject to respond to any questions, and may end their involvement at any moment.
Data collection and measures
A structured, self-administered questionnaire was used for data collection. The questionnaire consisted of three sections: demographic and clinical information, the asthma control test (ACT), and self-practice and knowledge test. When a child or an adolescent was found to be eligible, the study investigator and clinical pharmacists working at the study sites matched them with one primary caregiver (a parent or another adult) who accompanied them and gave their consent on their behalf to participate in the study after being fully informed of its purpose and goals.
Asthma control test
Asthma control was measured with the ACT, a tool that is validated and also most commonly used for that purpose in asthma patients. It is a patient-centered, self-administered, and five-item structured questionnaire that assesses multiple dimensions of the patient’s experience (Nathan et al., 2004; Revicki and Weiss, 2006).
Similar to other asthma evaluation instruments, the ACT measures asthma control as a continuous variable and allows the numerical differentiation of controlled and uncontrolled disease. Its questions use a 5-point Likert-type rating scale and specifically assess asthma symptoms (daytime and nocturnal), the use of rescue medications, and the effect of asthma on daily functioning in a month. Responses are summed up to give a total score of 5 to 25 (Hallit et al., 2017; Revicki and Weiss, 2006; Trivedi and Denton, 2019). The following ACT scores were utilized in the current study to determine asthma control: controlled asthma (CA), 25 points; partially controlled asthma, 20–24 points; uncontrolled asthma (UA), <19 points (Nathan et al., 2004).
In this study, responses were given by the child’s parents (father or mother). The internal consistency reliability of the ACT survey was 0.85 measured by Cronbach’s alpha. For the purpose of this study, a score of <19 points was considered UA and a score of ≥19 is considered CA.
Self-practice and knowledge test
Questions regarding asthma knowledge and self-management care were used in this study and were obtained from the literature (Beaurivage et al., 2018; Kritikos et al., 2005). Self-practice and knowledge test was composed of 10 true/false questions about the asthma action plan, putative risk factors, peak flow meter, environmental factors, and cigarette smoking at home for the purpose of this study. Therefore, the assigned score includes one point for a correct answer with a maximum score of 10. The internal validity and reliability of the questions were satisfied with Cronbach’s alpha of 0.77.
Statistical analysis
The data was coded and entered into the Statistical Package for Social Science version 22.0. Descriptive statistics were performed using means and SD for numerical data and as summary frequencies and percentages for categorical data. The chi-squared test was used to measure the relation between categorical variables and the independent t-test was used to measure the association between the means of continuous variables. Multiple regression model was performed to predict variables that affect UA. p-values ≤ 0.05 were considered to be statistically significant.
RESULTS
Patient characteristics
It included participants with asthma between the ages of 6 and 17 who had been diagnosed by a specialist at least 6 months prior to enrollment in the study. The pediatric patients and their primary caregivers were recruited from two major governmental outpatient clinics in Ramallah and Hebron within the period from November 2020 to March 2021. Of the 188 patients interviewed for this study, 132 consented to participate (response rate 70.2%). The mean age was 8.6 ± 3.0, and 79 (59.8%) of them were boys. Only one-third of the parents, either fathers or mothers, had a university education, 40 (30.3%) and 46 (34.8%), respectively. The mean duration of asthma of all participants was 30.9 ± 19.4 months, and most of the parents were smokers, 101 (76.5%). Clinically most of the patients were taking SABA, 101 (76.5%), and two-thirds were taking ICS, 88 (66.6%). More than half of the patients, 75 (56.8%), had asthma-related hospitalization (Table 1).
Level of asthma control
Patients were categorized into two categories based on their asthma control: the CA (≥19 score on ACT) and UA (<19 score on ACT). CA group included 47 patients (35.6%) and the UA group included 85 patients (64.3%) (Fig. 1). Moreover, among the 47 patients in the controlled group, 67% had mild asthma, 22% had moderate asthma, and 11% had severe asthma. However, in the UA group, 53% had mild asthma, 26% had moderate asthma, and 21% had severe asthma.
Significantly more children with UA were hospitalized at least once in the past year because of asthma in comparison to children in the CA group (87% versus 675; p < 0.05). Not surprisingly, those in the UA group had more children who use systemic corticosteroids (40% vs. 23%; p <0.05) compared to patients in the CA group. Moreover, we found that fathers’ and mothers’ education was associated with the level of asthma control too (p < 0.05); the higher the education of the parents was, the better the asthma control. There were no significant correlations between levels of asthma control for other demographic variables like children’s age, gender, BMI, or asthma duration (p > 0.05).
Knowledge and self-management practice
Overall asthma knowledge of parents was fairly good with a mean score of 6.9 ± 1.9. Univariate analysis revealed a significantly higher score of asthma knowledge for parents of CA children (6.6 vs. 7.3, t = 2; p < 0.05) than for parents of UA.
Only 15 (11.4%) children indicated obtaining an action plan to aid the treatment of asthma symptoms (Table 2).
Between children in the UA group, only 3 (3.5%) children had an action plan and indicated using it. The same is for the peak flow meter which appears to be of no common use in our routine clinical practice. Only 11 patients (8.3%) of all patients in the controlled and UA groups have used peak flow meter before. Those with an action plan were more likely to use regular inhaled corticosteroids. As expected, more parents in the CA group stated that their child tries to stay away from stressors the majority of the time (83% vs. 64%) compared to the UA group (p < 0.05). Moreover, parents within the CA group were less likely to be committed to smoking at home.
Multiple regression analysis
A stepwise multivariate logistic regression model was used to estimate connections between independent variables and UA in Table 3. The following four factors were found to be still significant and connected to UA: admission to hospitals from asthma (OR = 3.13; CI: 2.42–3.53), use of systemic steroids (OR = 2.14; CI: 1.71–2.83), exposure to smoke (OR = 2.31; CI: 1.65–2.77), and asthma knowledge (OR = 0.39; CI: 0.09–0.77). We found no significant associations with other demographic or clinical variables (Table 3).
DISCUSSION
Our study indicates that a high percentage of UA was among children and adolescents who visited governmental primary care units in West Bank.
In this analysis, patients were considered to have CA if they scored >19 on the ACT. Only 47 (35.6%) of participants had controlled disease; of those, 67% had mild asthma, 22% had moderate asthma, and 11% had severe asthma as they were diagnosed by their consultants. Globally, the proportion of asthma patients with controlled disease varies according to setting, sample size, and the assessment tool used (Banjari et al., 2018). The results of this study are inconsistent with two earlier research works conducted in Riyadh; the first determined 41% of participating children have CA, and the second reported that, among Saudi adolescents, the majority have mild to moderate asthma (Banjari et al., 2018; BinSaeed, 2014). In contrast, (Ungar et al., 2015) conducted a study in the Greater Toronto Area on 879 asthmatic children in the age group 1–18; only 11% had CA (Ungar et al., 2015).
Our findings revealed that children with asthma are better controlled when their caregivers are more knowledgeable about the condition. It is well established that knowledge is essential for managing asthma (Green and Frankish, 1994), and prior work supports that good asthma control is associated with the primary caregiver having a greater degree of asthma knowledge (Brown et al., 2010; Khdour et al., 2020; Zhao et al., 2013). Asthma control and prevention of hospital admission require parents to be equipped with the expertise and skills needed for efficient disease self-control (Leggett et al., 2005). Our findings in this study revealed that parents and caregivers have more knowledge and self-management skills to avoid asthma triggers have children whose asthma is significantly better controlled. A study conducted by BinSaeed (2014) in Saudi Arabia likewise showed that there were significant knowledge gaps existing among children’s parents with asthma that negatively affected the management of disease and so patient’s quality of life.
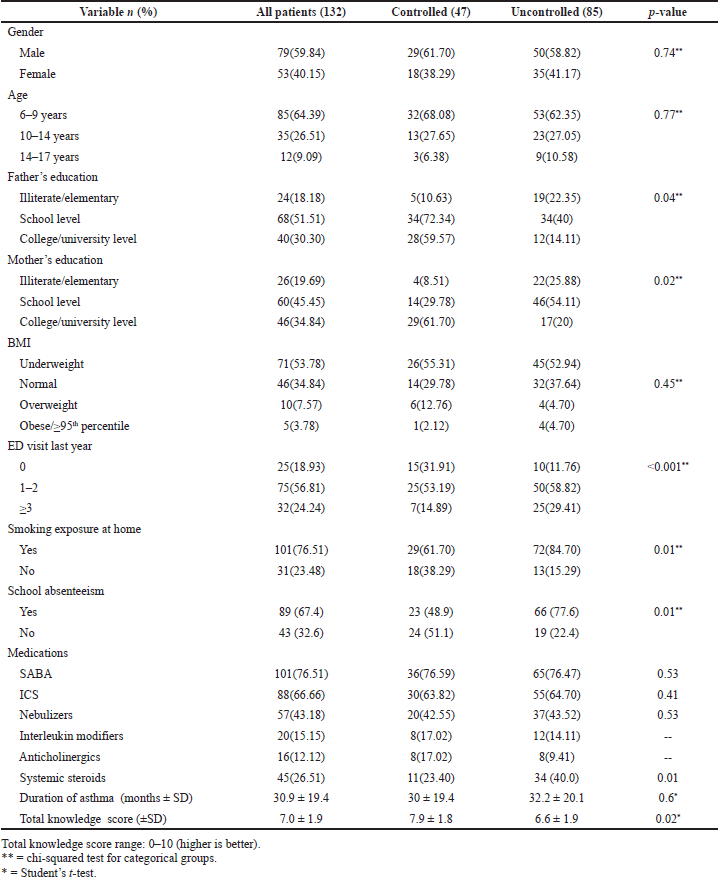 | Table 1. Patient characteristics and univariate analysis results. [Click here to view] |
Moreover, our findings revealed national guidelines’ lack of direction for healthcare providers to supply written action plans for asthma management. Asthma action plans reduce hospitalization, Emergency Department (ED) visits, and office visits; improve quality of life; and are recommended by most international guidelines. However, Kouri et al. (2017) revealed that less than 25% of asthma patients received action plans due to the fact that healthcare providers are lacking the information needed to complete instructions on intensifying therapy in the event of an exacerbation. Meanwhile, Kelso advocates in his review that better outcomes are achieved by educating parents at the time of diagnosis about the disease, medication, and the expectation of therapy, and reinforcing this information at all the following visits, rather than by means of written action plans (Kelso, 2016).
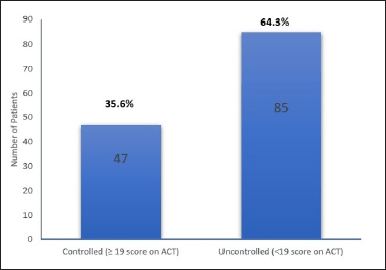 | Figure 1. Level of asthma control. [Click here to view] |
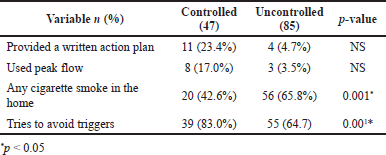 | Table 2. Knowledge and self-management practices. [Click here to view] |
Commonly reported indicators in this study included exacerbations and daytime asthma symptoms. The group having poor disease control also had a higher percentage of admissions; this is consistent with a study conducted by McGhan et al. (2006) on asthmatic children in Canada, at the age of 5–13 years, in which about half of those with poor control experienced exacerbations and daytime symptoms and a quarter had visited the ED within the last year.
A surprising finding of this work was that although inhaled corticosteroids were highly utilized, their use was not associated with better asthma control. This is similar to findings from a large cross-sectional study by Cowie et al. (2004) in which 2,437 patients used inhaled corticosteroids, but only 15% of those achieved disease control (Cowie et al., 2004; Khdour et al., 2019). However, we did observe a significant correlation between the use of systemic steroids and poor asthma control. Prescription of systemic steroids may itself indicate poor asthma control, while poor control can stem from numerous considerations involving inadequate medication adherence and wrong use of inhalers (Price et al., 2002).
Among participants in our study, 101 (76.5%) lived in households with occasional-to-regular smoke exposure, and these respondents exhibited significantly worse asthma control than others residing in nonsmoking households (p < 0.01). In fact, we found smoke exposure to be among the most significant factors for predicting poor control. Similarly, previous reports have documented moderate to severe asthma as being more likely in children exposed to tobacco smoke (Morkjaroenpong et al., 2002) and such children as being more prone to asthma exacerbations and impaired lung function (Gazzotti et al., 2013). Overall, each hour of smoke exposure in a week has been determined to increase the probability of poor management by a third. Consequently, health providers and clinicians should place a high priority on reducing smoke exposure in children (McGhan et al., 2006).
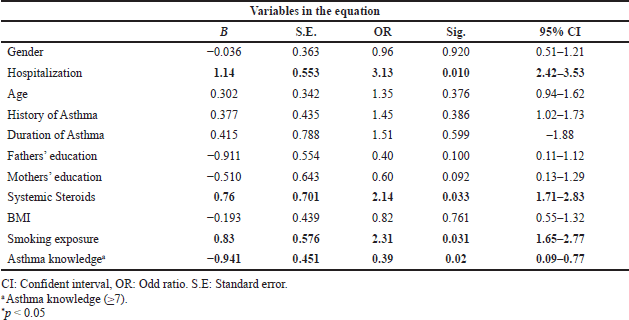 | Table 3. Multiple regression analysis for variables predicting UA. [Click here to view] |
All patients should be provided with a written action plan appropriate for their asthma control level and health literacy so that they can know how to recognize and respond to worsening asthma. In addition, asthma patients should be taught how to manage their condition in a variety of contexts, including homes, schools, and the community, enhance the conditions at home, and find and eliminate indoor asthma “triggers” that aggravate asthma.
LIMITATIONS
One limitation of this study is generalizability; it must be conducted on a bigger sample size, gathered from hospitals in various West Bank regions. In addition, qualitative research may produce more precise results than semi-structured surveys addressing the specifics of asthma effects on patients’ asthma control. Last, performing a study to determine the differences between the features of patients in general clinics and pulmonary clinics would aid in precisely defining the asthma control status.
CONCLUSION
In Palestinian children and adolescents with asthma, two-thirds of the participants had inadequate asthma control during the process of the investigation. Education of parents and children about asthma and the availability of inexpensive asthma care services may actually enhance asthma control in children.
ACKNOWLEDGMENTS
The authors would like to thank the medical staff at the Ministry of Health Primary Healthcare Units in Ramallah and Hebron for facilitating the data collection process.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to the conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
FINANCIAL SUPPORT
This research did not obtain any specific grant from funding agencies or official, commercial, or non-profit sponsors.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.
ETHICAL APPROVALS
Ethical approval was obtained from the Research Ethical Committee at Al-Quds University [Ref No: 164/REC/2020].
DATA AVAILABILITY
All data generated and analyzed are included in this research article.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Banjari M, Kano Y, Almadani S, Basakran A, Al-Hindi M, Alahmadi T. The relation between asthma control and quality of life in children. Int J Pediatr, 2018; 2018: 1–6. CrossRef
Beaurivage D, Boulet LP, Foster JM, Gibson PG, McDonald VM. Validation of the patient-completed asthma knowledge questionnaire (PAKQ). J Asthma, 2018; 55(2):169–79. CrossRef
Becker AB, Abrams EM. Asthma guidelines: the global initiative for asthma in relation to national guidelines. Curr Opin Allergy Clin Immunology, 2017; 17(2):99–103. CrossRef
BinSaeed AA. Caregiver knowledge and its relationship to asthma control among children in Saudi Arabia. J Asthma, 2014; 51(8):870–5. CrossRef
Brown N, Gallagher R, Fowler C, Wales S. The role of parents in managing asthma in middle childhood: an important consideration in chronic care. Collegian, 2010; 17(2):71–6. CrossRef
Cowie RL, Underwood MF, Field SK. Inhaled corticosteroid therapy does not control asthma. Can Respir J, 2004; 11(8):555–8. CrossRef
Gandhi PK, Kenzik KM, Thompson LA, DeWalt DA, Revicki DA, Shenkman EA, Huang IC. Exploring factors influencing asthma control and asthma-specific health-related quality of life among children. Respir Res, 2013; 14(1):1–10. CrossRef
Gazzotti MR, Nascimento OA, Montealegre F, Fish J, Jardim JR. Level of asthma control and its impact on activities of daily living in asthma patients in Brazil. J Bras Pneumol, 2013; 39:532–8. CrossRef
Green LW, Frankish CJ. Theories and principles of health education applied to asthma. Chest, 1994; 106(4):219S–30S. CrossRef
Hallit S, Raherison C, Waked M, Salameh P. Validation of asthma control questionnaire and risk factors affecting uncontrolled asthma among the Lebanese children’s population. Respir Med, 2017; 122:51–7. CrossRef
Kelso JM. Do written asthma action plans improve outcomes? Pediatr Allergy Immunol Pulmonol, 2016; 29(1):2–5. CrossRef
Kenyon N, Zeki AA, Albertson TE, Louie S. Definition of critical asthma syndromes. Clin Rev Allergy Immunol, 2015; 48(1):1–6. CrossRef
Khdour MR, Elyan SO, Hallak HO, Jarab AS, Mukattash TL, Astal A. Assessment of the inhalation technique and adherence to therapy and their effect on disease control in outpatients with asthma. J Pharm Health Serv Res, 2019; 10(3):353–8. CrossRef
Khdour MR, Elyan SO, Hallak HO, Jarab AS, Mukattash TL, Astal A. Pharmaceutical care for adult asthma patients: a controlled intervention one-year follow-up study. Basic Clin Pharmacol Toxicol, 2020; 126(4):332–40. CrossRef
Kouri A, Boulet LP, Kaplan A, Gupta S. An evidence-based, point-of-care tool to guide completion of asthma action plans in practice. Eur Respir J, 2017; 49(5):1602238. CrossRef
Kritikos V, Krass I, Chan HS, Bosnic-Anticevich SZ. The validity and reliability of two asthma knowledge questionnaires. J Asthma, 2005; 42(9):795–801. CrossRef
Leggett JJ, Johnston BT, Mills M, Gamble J, Heaney LG. Prevalence of gastroesophageal reflux in difficult asthma. Chest, 2005; 127(4):1227–31. CrossRef
McGhan S, MacDonald C, James D, Naidu P, Wong E, Sharpe H, Hessel PA, Befus AD. Factors associated with poor asthma control in children aged five to 13 years. Can Respir J, 2006; 13(1):23–9. CrossRef
Mirzaei M, Karimi M, Beheshti S, Mohammadi M. Prevalence of asthma among middle eastern children: a systematic review. Med J Islam Repub Iran, 2017; 31:9. CrossRef
Morkjaroenpong V, Rand CS, Butz AM, Huss K, Eggleston P, Malveaux FJ, Bartlett SJ. Environmental tobacco smoke exposure and nocturnal symptoms among inner-city children with asthma. J Allergy Clin Immunol, 2002; 110(1):147–53. CrossRef
Nathan RA, Sorkness CA, Kosinski M, Schatz M, Li JT, Marcus P, Murray JJ, Pendergraft TB. Development of the asthma control test: a survey for assessing asthma control. J Allergy Clin Immunol, 2004; 113(1):59–65. CrossRef
Price D, Castro M, Bourdin A, Fucile S, Altman P. Short-course systemic corticosteroids in asthma: striking the balance between efficacy and safety. Eur Respir Rev, 2002; 29(155):190151. CrossRef
Trivedi M, Denton E. Asthma in children and adults-what are the differences and what can they tell us about asthma? Front Pediatr, 2019; 7:256. CrossRef
Reddel HK, Bateman ED, Becker A, Boulet LP, Cruz AA, Drazen JM, Haahtela T, Hurd SS, Inoue H, de Jongste JC, Lemanske Jr RF, Levy ML, O’Byrne PM, Paggiaro P, Pedersen SE, Pizzichini E, Soto-Quiroz M, Szefler SJ, Wong GWK, FitzGerald JM. A summary of the new GINA strategy: a roadmap to asthma control. Eur Respir J, 2015; 46(3):622–39. CrossRef
Revicki D, Weiss KB. Clinical assessment of asthma symptom control: review of current assessment instruments. J Asthma, 2006; 43(7):481–7. CrossRef
Rydström I, Dalheim-Englund AC, Holritz-Rasmussen B, Möller C, Sandman PO. Asthma–quality of life for Swedish children. J Clin Nurs, 2005; 14(6):739–49. CrossRef
Tarraf H, Aydin O, Mungan D, Albader M, Mahboub B, Doble A, Lahlou A, Tariq L, Aziz F, El Hasnaoui A. Prevalence of asthma among the adult general population of five Middle Eastern countries: results of the SNAPSHOT program. BMC Pulm Med, 2018; 18(1):1–14. CrossRef
Ungar WJ, Hadioonzadeh A, Najafzadeh M, Tsao NW, Dell S, Lynd LD. Parents and adolescents preferences for asthma control: a best-worst scaling choice experiment using an orthogonal main effects design. BMC Pulm Med, 2015; 15(1):1–10. CrossRef
Zhao J, Shen K, Xiang L, Zhang G, Xie M, Bai J, Chen Q. The knowledge, attitudes and practices of parents of children with asthma in 29 cities of China: a multi-center study. BMC Pediatr, 2013; 13(1):1–6. CrossRef