INTRODUCTION
The COVID-19 pandemic caused a considerable and wide-ranging impact on morbidity and mortality and led to devastating economic and social disruption across various countries (Bonotti and Zech, 2021; Talic et al., 2021; Xiang et al., 2021). At first, governments’ responses aimed to limit COVID-19 spread and its associated impact in the absence of effective treatment and vaccines. Initial activities included enhanced disease surveillance, quarantine arrangements, the introduction of social distancing regulations, and lockdown measures, such as border closure, home confinement, prohibition of gatherings, and closure of establishments and premises (Girum et al., 2021; Haider et al., 2020; Nussbaumer-Streit et al., 2020). Malaysia was no exception with the early introduction of extensive lockdown measures in conjunction with complex disease prevention and control arrangements (Godman et al., 2020; Shah et al., 2020; Umair et al., 2021).
In particular, the higher education sector had temporarily closed and transitioned to online teaching and learning (Shah et al., 2020). A recent paper showed that challenges in the transition of Malaysian higher education to online teaching and learning included insufficient availability of the necessary devices and equipment, unaffordability of Internet bundles, and issues with the speed and quality of the Internet connection among students, especially those from low-income families or living in rural areas (Azman and Abdullah, 2021). Faculty members often lacked the necessary skills to conduct tutorials and practical skills training remotely, as well as the required equipment, such as microphones and webcams, and appropriate lighting and audio modulation facilities while working from home or in the office (Azman and Abdullah, 2021). Besides, there was a need to introduce innovative approaches when delivering classes to keep students engaged without face-to-face interaction (Mustafa, 2020).
The pandemic has affected health professions’ education (HPE) especially severely. HPE is a separate domain of higher education that emerged in the 1960s with the responsibility to society to produce competent practitioners trained to work in a health or health-related fields (Blouin, 2022). HPE’s domain draws from a wide range of disciplinary knowledge to consider the practitioners’ different professional backgrounds and cultures. It includes medicine, nursing, dentistry, pharmacy, and biomedical sciences. More than ever before, HPE in Malaysia had to be seen in the context of health systems to meet the challenges caused by the pandemic, including the rising need for skilled health professionals (HP) (Azman and Abdullah, 2021).
For instance, before the pandemic, several studies revealed insufficient knowledge about antimicrobial resistance (AMR) among medical and dental students in Malaysia (Haque et al., 2019; Tiong and Chua, 2020; Wong et al., 2016). Since the pandemic’s beginning, the importance of HPs’ awareness about AMR has grown with high rates of inappropriate prescribing of antibiotics for patients with COVID-19 despite limited bacterial or fungal coinfections (Chowdhury et al., 2022a; Kumar et al., 2022; Langford et al., 2021). The issue could be efficiently addressed by enhanced training of a wide range of HPs in the appropriate use of antibiotics, such as introducing AMR stewardship programs among physicians and pharmacists (Godman et al., 2021; Mohamad et al., 2022).
Another concern is the growing prevalence of noncommunicable diseases (NCDs) in Malaysia which has had profound implications during the COVID-19 pandemic. Higher NCD burden, especially concerning cardiovascular diseases, obesity, and diabetes mellitus, corresponded to higher COVID-19 death rates (Ariaratnam et al., 2020; Rahim et al., 2020; Sazlina et al., 2020; You et al., 2019). Training of HPs, involving community pharmacists and nurses in careful handling of the patients based on evidence-based approaches, can help in improving the continuity of healthcare and addressing the double burden of COVID-19 and NCDs (Ayadurai et al., 2019; Hassali, 2017; Mustapha et al., 2020). Therefore, the COVID-19 pandemic has highlighted HPE’s crucial role in ensuring preparedness and quality of healthcare services.
Little evidence covering the impact of the COVID-19 pandemic on higher education in Malaysia exists. Previous studies explored students’ perception (Sababathy et al., 2021), the efficiency of e-learning (Nordin and Nordin, 2020), and university employees’ well-being (Daud et al., 2020) during the pandemic. However, we could not find papers focusing explicitly on the challenges faced by HPE establishments in Malaysia. Similar studies were undertaken in other settings, including higher income countries where resources and familiarity with e-learning approaches can be less of an issue (Alrasheedy et al., 2021; Alsoufi et al., 2020; Azlan et al., 2020; Azman and Abdullah, 2021; Chowdhury et al., 2022b, 2022c; Dhawan, 2020; Etando et al., 2021; Sharma et al., 2022).
OBJECTIVES OF THE STUDY
This study aims to explore educators’ perceptions of the impact of COVID-19 on HPE in Malaysia. The research generated from professionals’ views may increase our understanding of the challenges faced by HPE establishments during pandemics and their response in addressing these. Consequently, it offers a more comprehensive approach to current COVID-19 and HPE research data. The present study is a pilot project. Ultimately, we aimed to answer the research question “How do educators in Malaysia perceive the impact of the COVID-19 pandemic on health professionals’ education?” to develop a preliminary research framework. The findings of this study, combined with those from subsequent analyses, can potentially be used to improve HPE in Malaysia during the current and future pandemics.
METHODS
Approach
This descriptive pilot study is an extension of cross-cultural exploratory research conducted by the coauthors in different countries around the globe (Chowdhury et al., 2022b, 2022c; Etando et al., 2021; Sharma et al., 2022). A pragmatism strategy was applied to practically address the issues in question (Allemang et al., 2022; Kelly and Cordeiro, 2020). The inherent focus of pragmatism is based on experience and action rather than on understanding reality as a value on its own (Hothersall, 2019). As a flexible and highly reflexive approach to research, pragmatism supports deductive and inductive reasoning, allowing the choice of a methodology that is the most relevant to address the research question (Kaushik and Walsh, 2019).
Sampling
A purposive sampling approach was used for this study, which was based on the expert knowledge of the coauthors, who are themselves HP educators. This enhanced the ability to obtain a rich source of data from a limited sample to achieve the study’s objectives (Bhardwaj, 2019; Campbell et al., 2020). To enhance the study’s credibility, transferability, and dependability, a data source triangulation method was used with participants from various medical and other health profession disciplines (Carter et al., 2014; Heale and Forbes, 2013). The initial sample of 10 participants included 5 educators from public and 5 from private universities in Malaysia to ensure complete coverage. The participants also covered a wide range of subjects, including physiology, microbiology, early clinical skills, internal medicine, surgery, otorhinolaryngology, dentistry, and biosciences.
Study instrument and data collection
A qualitative semistructured questionnaire approach was adopted. The questionnaire was based on recent research conducted among African and Asian countries (Chowdhury et al., 2022b; Etando et al., 2021; Sharma et al., 2022). The qualitative exploratory survey method allows participants to answer questions at a place of their convenience and formulate and modify their answers over time before being sent back (Hanna and Gough, 2020; Safdar et al., 2016; Tuckett and Stewart, 2003, 2004), which is essential during pandemics. Data collection was conducted from October 2021 to January 2022. The questionnaires were emailed to the selected educators upon receiving their verbal consent to participate. The participants were encouraged to constantly communicate with the researchers to clarify any details as the need arose.
The questionnaire consisted of four main open-ended questions and some prompt questions. The main questions focused on the challenges presented by the COVID-19 pandemic, the response and support provided by the universities to address them, and the lessons learned for future pandemics. The four questions are as follows:
1) What challenges has COVID-19 presented to HPE in Malaysia?
2) How did your university respond immediately to the challenges presented by the COVID-19 pandemic?
3) What support was harnessed to help mitigate the challenges faced by your university?
4) What lessons can be learned to prepare HPE establishments in Malaysia for future pandemics?
The questions were deliberately developed to avoid closed and leading questions to maintain flexibility, considering that the content should generate ideas and valuable information. The respondents were expected to provide four to five answers to each main question. Five follow-on questions were added to achieve a more specific understanding of the respondent’s experience.
Analysis
A framework method of data analysis was applied (Goldsmith, 2021). This approach allows researchers to identify themes systematically according to predetermined procedures and make necessary changes throughout the research process. The framework created through setting codes and subsequently organizing them into categories transforms the data into a new structure that helps summarize the findings (Gale et al., 2013). Besides, this approach provides a detailed outline of individual observations and enables themes to develop deductively and emerge inductively from participants’ experiences and views (Cavallieri et al., 2021).
This study reports on the initial framework shaped by recurring and salient themes and subthemes identified through the analysis of the answers provided by the respondents in the pilot study. The main themes were predetermined deductively by the research questions and stored using different sheets of Microsoft Excel. The further analysis relied on inductive reasoning in which subthemes emerged through repeated evaluation of the questionnaire data. Initially, two research team members independently coded the responses from the same 10 questionnaires and subsequently agreed on a set of codes to form the initial analytical framework. Some of the codes were subsequently grouped into categories. Using diagrams, several codes were then mapped to explore the relationship between the subthemes. In addition, patterns among the different types of participants were identified.
Ethical considerations
Verbal informed consent was taken from the participants before starting the pilot project to ensure they fully comprehended all aspects of the study and voluntarily agreed to participate. They were informed that their identities would be kept confidential, guaranteeing respect for autonomy and trust.
RESULTS
Participants in this pilot study represented a number of disciplines including preclinical disciplines (n = 4), clinical disciplines (n = 4), dentistry (n = 1), and biosciences (n = 1). Table 1 summarizes the distribution of the research participants.
The qualitative analysis yielded three main themes predetermined by the research questions: 1) challenges in HPE presented by the COVID-19 pandemic, 2) response of HPE establishments to the COVID-19 pandemic, and 3) lessons learned to prepare HPE establishments for future pandemics.
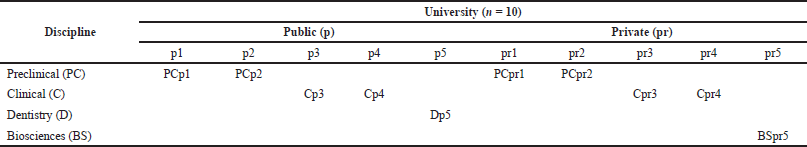 | Table 1. Distribution of research participants. [Click here to view] |
 | Table 2. Challenges in HPE presented by COVID-19. [Click here to view] |
Challenges in HPE presented by the COVID-19 pandemic
Challenges brought about by the COVID-19 pandemic caused unprecedented disruption regarding the education of HPs in Malaysia, predominantly their clinical and practical skills teaching.
The initial coding for the theme “challenges” identified several key issues that needed to be addressed by the universities at the beginning of the COVID-19 pandemic. These are summarized in Table 2.
The participants mentioned closely related themes, including digital needs and the learning environment at home, as key opposing factors with e-learning approaches. While some educators said that most of the students had access to the necessary equipment, others reported that there were students experiencing problems with the Internet connectivity and affordability and availability of Internet bundles and devices.
[One of the main challenges is] instability of the Internet coverage and unavailability of two [electronic] devices (mobile phone and computer) [the second device with a camera is used for online exams] … some of [the students] have only one device. Not all students can afford the Internet. (PCp1)
Few students have no access to the necessary equipment; some have to share [the equipment] with other family members due to financial constraints at the start of the pandemic. (Cp4)
Issues with the environment for online learning for the students at home [included] …. no private place, noisy environment [due to loud] siblings. (Cp4)
The relationship between the subthemes “digital needs” and “learning environment at home” is shown in Figure 1.
Several educators highlighted insufficient technology-based teaching and learning training at the start of the pandemic. A few also stated that there were delays with the initiation of appropriate training.
Much of the problems arose at the beginning since [online teaching] is a new method of teaching that had not been explore or used before. At the beginning of the pandemic, no formal courses were conducted [for] the teachers on how to use the online platform. (Cp4)
Almost all the respondents reported difficulties in teaching practical and clinical skills due to restricted access to laboratories and healthcare facilities. Overall, this was one of the biggest challenges faced by the HP educators during the pandemic.
[One of the main challenges is] difficulty in preparing immediate simulation-based education and online modules to facilitate clinical competencies. (PCp2)
Practical sessions had to be delivered virtually; access to laboratories was totally stopped (BSpr5)
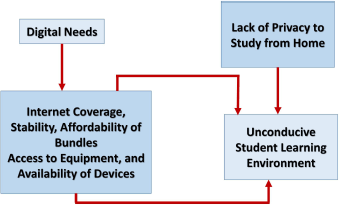 | Figure 1. Relationship between “digital needs” and “learning environment at home.” [Click here to view] |
The participants reported issues associated with the change from paper-based to fully online assessments during the pandemic. They highlighted the problems with maintaining the security and integrity of assessment systems, especially the inability to conduct clinical case-based and practical skills assessments online. Some educators did not believe online assessment could be a viable alternative to face-to-face examinations.
[One of the main challenges is lack of] fair and thorough assessment: complete assessment is only possible via face-to-face. (Cpr3)
[One of the main challenges is] inability to validate students’ performance of a practical session, to assess a student’s ability to perform a skill. (PCpr2)
The codes “practical and clinical skills” and “assessment” were mapped, and several new subthemes emerged in exploring the relationship between the initial themes (Fig. 2).
Most educators reported difficulties regarding a lack of interaction between students and teachers during the session and with each other. Participants mentioned the inability to meet with students in person and a lack of interaction with them as one of the main challenges with HPE brought about by the pandemic.
[One of the main challenges is] complete shift from face-to-face lectures to online teaching, ... unable to meet the students in person. (BSpr5)
[One of the main challenges is] lack of interaction [of students] with each other: continuous interaction [among students] contributes extensively to learning. (Cpr3)
Among the other challenges mentioned by the participants were difficulties in educational planning and decision-making due to the uncertainty caused by the pandemic, increased mental distress among educators, a higher risk of contracting COVID-19 in clinical settings, and hampered research activities.
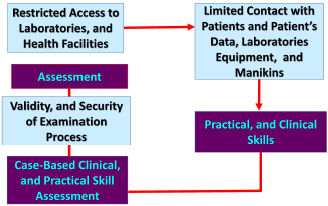 | Figure 2. Relationship between “practical and clinical skills” and “assessment.” [Click here to view] |
Response of HPE establishments to the COVID-19 pandemic
The immediate response of the universities to the pandemic and the support harnessed to help mitigate the challenges they faced were subsequently analyzed. Table 3 outlines the codes for the “responses” identified from the initial analytical framework.
To address the digital needs, the university’s quick response included the provision of digital equipment as well as ensuring IT connectivity for both educators and students. A particular focus was placed on supporting students with limited access to necessary equipment, including devices and Internet bundles.
Screening [was conducted to identify] the students who need help [with equipment and bundles]. (Cp3)
The university has identified those poor students and provided them with a laptop [for] loan for them to use for online learning. (Cp4)
All lecturers (mentors) [had] to check and identify if any of their students (mentees) had ... related problems... The lecturers were reminded to avoid unnecessary online streaming sessions so that students may use the internet quota prudently. (PCp2)
At the beginning of the pandemic, training was provided for both the educators and students to enhance online teaching and learning preparedness.
Survey on [lecturers’ and students’] readiness to use [online] systems [was conducted]. (PCp1)
There were many [...] trainings conducted by the university. All trainings were made mandatory for [...] staff, quickly transform to online teaching and learning methods. (PCpr2)
The universities also provided various teaching resources to support lecturers in the transition to an online mode of knowledge transfer, especially to assist with online teaching clinical and practical skills (subtheme 1) and assessments (subtheme 2).
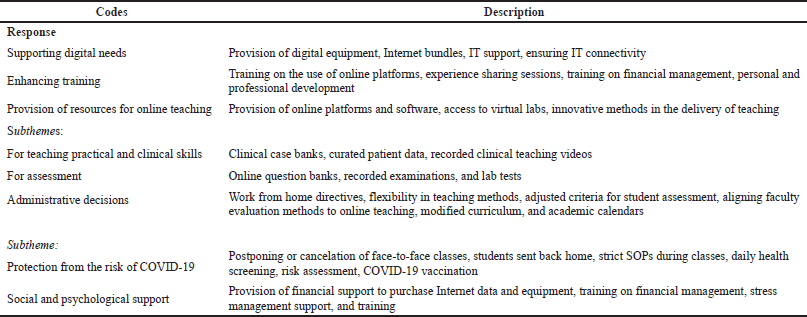 | Table 3. Response of HPE establishments to COVID-19. [Click here to view] |
Access to virtual labs was made available to us. [The university management tried] to innovate the delivery of teaching with the help of available resources. (BSpr5)
[The university organized] online clerking of patients and case scenarios, [provided with] recorded lung (and heart) sounds and physical examination videos. Online assessment of clinical skills [was arranged] with recorded examination and laboratory tests. Clinical case banks were created. Curated clinical material like X-rays, ECGs, etc. [was collected] from hospitals and online sources. (Cpr4)
The COVID-19 pandemic also forced many higher learning establishments to adopt alternative procedures to work, modify curricula, and make changes to academic calendars. One of the critical administrative responses to the pandemic was to protect staff and students from contracting COVID-19. This was achieved through postponing or cancelling face-to-face classes and sending students home. In addition, whenever face-to-face classes (especially clinical sessions) resumed, the university administration organized risk assessments, daily screening, monitoring of standard operating procedure (SOP) compliance, and, as soon as it became possible, COVID-19 vaccinations for both students and educators.
We have to rearrange the academic calendar to adapt to the dynamic changes of the COVID-19 pandemic. Our university has instructed us to start online teaching and learning activities during the Movement Control Order. The clinical teaching has to be withheld until a certain period. (Cp4)
Our institution [came out] with a special application to assess daily risk of COVID-19 infection among staff and students. This software was created by a team of university researchers during the pandemic’s beginning. It has been used since then, where every working day, staff and students have to log in to the system and answer the question to assess their risk of COVID -19 infection. (Cp4)
Several participants mentioned that social and psychological support was provided to students and staff. Educators were also encouraged to take courses on identifying students in mental distress.
For online teaching activities, our institution has provided financial support to the students to purchase the Internet data [and] to buy a computer for those in need. (Cp4)
University’s psychology department conducts numerous mindfulness sessions for the well-being of students and staff to overcome the difficulties or issues faced during this ‘new normal.’ (PCpr2)
Lessons learned to prepare HPE establishments for future pandemics
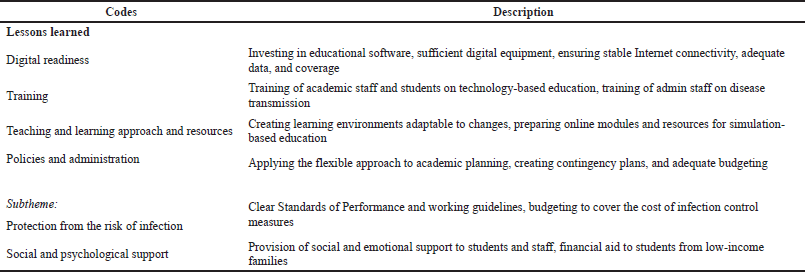
The codes identified from the initial analytical framework for the theme “lesson learned” corresponded to the ones determined to the “response” (Table 4).
University educators highlighted the importance of maintaining an adequate level of digital readiness to ensure educational preparedness for future pandemics and the ability to preserve the continuity of teaching and learning.
Internet connectivity and Wi-Fi access should be improved at the national level, especially in rural areas. [Universities should] improve the Internet access in the students’ accommodations. (Dp4)
According to several participants, the ability of universities to educate and train their staff on the use of online teaching and learning methods was highly valued. Besides, one of the educators stated that it is also important to educate university administrators on adapting to the online work mode and the basics of disease transmission.
Administrators and teachers should learn to adapt to as many activities as possible online and to make online activity the norm. Administrators should read and understand about disease transmission. (Cpr3)
 | Table 4. Lessons learned to prepare HPE establishments for future pandemics. [Click here to view] |
Several HP educators highlighted that the teaching-learning process and resources approach has to change with blended learning here to stay.
[There should be] transformation from the traditional teacher-centered to student-centered model to create learning environments that are responsive to continuously changing situations. (Cpr4)
The previous supply of hard copy books, articles, manuals, and other education resources [should be digitalized] into e-books and downloadable versions. (Dp4)
[Universities should prepare resources for] simulation-based education and online modules to develop clinical competencies. (PCp2)
Participants in this study also suggested a flexible approach is now needed for academic planning, contingency planning, and ensuring adequate budgets to help mitigate the impact of future pandemics on HPE. A subtheme “protection from the risk of infection” emerged within the theme “policies and administration.”
[It is important to have] adequate budgeting, especially to cover costs of quarantine, swabbing, and transportation and also to help the poor students and staff during these trying times, […] need to [make sure] that the flow of work is in order while maintaining the SOP to prevent infection among staff. (Cp4)
Finally, several participants mentioned the importance of providing students and staff with social, financial, and emotional support.
DISCUSSION
This pilot study aims to divulge a substantial number of challenges faced by HP educators in Malaysia at the start of the pandemic, as well as their responses to these challenges and the lessons learned. The main challenges faced by HP lecturers in Malaysia at the beginning of the pandemic included rapid adaptation to the e-learning environment, preparing necessary changes to the academic timetable, including delays in clinical exams, digital needs, and how to undertake practical and clinical examinations in an e-learning environment. These challenges were similar to several low- and middle-income countries (LMICs). The educators and students from these countries also had to adapt to online learning, lack of equipment, cost of Internet bundles (especially among disadvantaged students), and modifications in the pedagogy of teaching and learning, especially those involving practical and clinical teaching (Al-Balas et al., 2020; Alsoufi et al., 2020; Chowdhury et al., 2022b, 2022c; Etando et al., 2021; Sharma et al., 2022; Shawaqfeh et al., 2020; Shehata et al., 2020). Conversely, higher-income countries appeared better prepared for the closure of universities as they had been undertaking blended learning for several years before the onset of the pandemic (Alrasheedy et al., 2021; Chowdhury et al., 2022b).
Upon assessing the digital needs and the learning environment at home, we found that poor Internet coverage, affordability of devices and access to equipment, and a lack of privacy will affect the students’ learning. This finding is similar to a study conducted among university students in the Faculty of Business Management in a public university in Malaysia (Ismail et al., 2020). Additionally, we found that COVID-19 badly affected teaching practical and clinical skills due to restricted access to laboratories and healthcare facilities. There was limited contact between patients and students. Moreover, the academic burden for the lecturers has increased because they had to create additional online cases for the clinical sessions. Concerns over assessment validity and security of exams were strongly linked to skill-based teaching and learning. Assessment remains vital as it is the parameter of attainment of curriculum learning outcomes. Therefore, alternative assessment modes must be considered as reported in other settings (Rao et al., 2021).
The response of governments and universities in Malaysia to the challenges faced by HP educators and students to the closure of educational establishments and the instigation of online learning was similar to other LMICs (Al-Balas et al., 2020; Alsoufi et al., 2020; Chowdhury et al., 2022b, 2022c; Etando et al., 2021; Sharma et al., 2022; Shawaqfeh et al., 2020). The measures included supporting digital needs where there were concerns, such as the provision of devices and Internet bundles and online platforms, including virtual labs. Besides, training needs for both educators and students were addressed. Moreover, all lecturers were fully equipped with the necessary devices and software (Azman and Abdullan, 2021). Additional arrangements were in place for resuming face-to-face classes, such as strict compliance with COVID-19 SOPs. We have seen flexibility of academic calendars across countries, which is likely to remain post-pandemic with hybrid learning here to stay in Malaysia and across countries (Azlan et al., 2020). Additionally, more significant investments in simulation-based learning (SBL) have been made by many institutions to improve clinical competencies, although countries are still learning from each other on how to address these issues (Etando et al., 2021).
The lessons learned among the educators following the necessary instigation of e-learning approaches in Malaysia were similar to several other countries (Chowdhury et al., 2022b; Etando et al., 2021; Sharma et al., 2022). The need to invest in digital readiness was highlighted, including Internet and software availability and affordability. The participants stated the importance of maintaining academic staff adequately trained in e-learning approaches. Finally, this study emphasized the importance of a flexible approach toward e-learning and psychological support for students and staff (Chowdhury et al., 2022b; Etando et al., 2021; Sharma et al., 2022). Social and psychological support during the pandemic is necessary, given the impact of COVID-19 on mental health among HP students and educators during the pandemic which is consistent with the findings from previous studies (Chinna et al., 2021; Saddik et al., 2020; Saraswathi et al., 2020; Sundarasen et al., 2020).
CONCLUSION
The COVID-19 pandemic has conveyed several challenges faced by HPE in Malaysia due to the transition to online teaching and learning. This pilot study showed that the main challenges included unavailability of necessary equipment and regular access to the Internet, as well as unfamiliarity of educators and students with remote learning. These challenges have been addressed accordingly, and the gaps in response of HP establishments to the pandemic have been identified. The suggestions for future pandemic planning for HP establishments have been proposed considering hybrid learning is here to stay in Malaysia. Hence, the measures to support digital and training needs, including the expansion of online platforms and virtual labs, are being implemented by many HPE establishments of higher learning. Ultimately, social and psychological support to address mental health issues for students and educators during any pandemic remains crucial. We will be exploring these results further in the full study to provide additional directions to all key stakeholder groups in Malaysia during future pandemics.
ACKNOWLEDGMENTS
The authors show gratitude to Naufela Nafisa Ahmad, Master of Arts in English Language (Linguistics), Jalan Wangsa Delima 7, Wangsa Maju, 53300 Kuala Lumpur, Malaysia, for revising and providing her expert opinion about the quality of the English language of this article. The authors also express gratitude to Faiza Binte Mozammel, Photographer and Editor, 7/16/1 South Mugdapara Dhaka, Bangladesh, for her kind effort and time regarding image development and editing.
CONSENT FOR PUBLICATION
All authors reviewed and approved the final version and have agreed to be accountable for all aspects of the work, including any accuracy or integrity issues.
DISCLOSURE
The authors declare that they have no financial involvement or affiliations with any organization, association, or entity directly or indirectly with the subject matter or materials presented in this paper. This includes honoraria, expert testimony, employment, ownership of stocks or options, patents or grants received or pending, or royalties.
AUTHORS’ CONTRIBUTION
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis, and interpretation or in all these areas; they took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted, and have decided to be accountable for all aspects of the work.
DATA AVAILABILITY
The data is available to the principal author only for research purposes.
ETHICAL CONSIDERATIONS
Details include in Materials and Method section.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Al-Balas M, Al-Balas HI, Jaber HM, Obeidat K, Al-Balas H, Aborajooh EA, Al-Taher R, Al-Balas B. Distance learning in clinical medical education amid COVID-19 pandemic in Jordan: current situation, challenges, and perspectives. BMC Med Educ, 2020; 20(1):341; doi:10.1186/s12909-020-02257-4. CrossRef
Allemang B, Sitter K, Dimitropoulos G. Pragmatism as a paradigm for patient-oriented research. Health Expect, 2022; 25(1):38–47; doi:10.1111/hex.13384. CrossRef
Alrasheedy AA, Abdulsalim S, Farooqui M, Alsahali S, Godman B. Knowledge, attitude and practice about coronavirus disease (COVID-19) pandemic and its psychological impact on students and their studies: a cross-sectional study among pharmacy students in Saudi Arabia. Risk Manag Healthc Policy, 2021; 14:729–41; doi:10.2147/RMHP.S292354. CrossRef
Alsoufi A, Alsuyihili A, Msherghi A, Elhadi A, Atiyah H, Ashini A, Ashwieb A, Ghula M, Ben Hasan H, Abudabuos S, Alameen H, Abokhdhir T, Anaiba M, Nagib T, Shuwayyah A, Benothman R, Arrefae G, Alkhwayildi A, Alhadi A, Zaid A, Elhadi M. Impact of the COVID-19 pandemic on medical education: medical students’ knowledge, attitudes, and practices regarding electronic learning. PLoS One, 2020; 15(11):e0242905; doi:10.1371/journal.pone.0242905. CrossRef
Ariaratnam S, Rodzlan Hasani WS, Krishnapillai AD, Abd Hamid HA, Jane Ling MY, Ho BK, Shariff Ghazali S, Tohit NM, Mohd Yusoff MF. Prevalence of obesity and its associated risk factors among the elderly in Malaysia: findings from the National Health and Morbidity Survey (NHMS) 2015. PLoS One, 2020; 15(9):e0238566; doi:10.1371/journal.pone.0238566.
Ayadurai S, Sunderland B, Tee LB, Hattingh HL. A training program incorporating a diabetes tool to facilitate delivery of quality diabetes care by community pharmacists in Malaysia and Australia. Pharm Pract (Granada), 2019; 17(2):1457; doi:10.18549/PharmPract.2019.2.1457. CrossRef
Azlan CA, Wong JHD, Tan LK, A D Huri MSN, Ung NM, Pallath V, Tan CPL, Yeong CH, Ng KH. Teaching and learning of postgraduate medical physics using Internet-based e-learning during the COVID-19 pandemic—a case study from Malaysia. Phys Med, 2020; 80:10–6; doi:10.1016/j.ejmp.2020.10.002. CrossRef
Azman N, Abdullah D. A critical analysis of malaysian higher education institutions’ response towards COVID-19: sustaining academic program delivery. J Sustain Sci Manag, 2021; 16(1):70–96; doi:10.46754/jssm.2021.01.008 CrossRef
Bhardwaj P. Types of sampling in research. J Pract Cardio Sci, 2019; 5(3):157–63; doi:10.4103/jpcs.jpcs_62_19. CrossRef
Blouin D. Health professions education as a discipline: evidence based on Krishnan’s framework. Med Teach, 2022; 44(4):445–9; doi:10.1080/0142159X.2021.2020233. CrossRef
Bonotti M, Zech ST. The human, economic, social, and political costs of COVID-19. Recovering Civility during COVID-19, 2021; 1–36; doi:10.1007/978-981-33-6706-7_1. CrossRef
Campbell S, Greenwood M, Prior S, Shearer T, Walkem K, Young S, Bywaters D, Walker K. Purposive sampling: complex or simple? Research case examples. J Res Nurs, 2020; 25(8):652–61; doi:10.1177/1744987120927206. CrossRef
Carter N, Bryant-Lukosius D, DiCenso A, Blythe J, Neville AJ. The use of triangulation in qualitative research. Oncol Nurs Forum, 2014; 41(5):545–7; doi:10.1188/14.ONF.545-547. CrossRef
Cavallieri F, Sireci F, Fioravanti V, Toschi G, Rispoli V, Antonelli F, Costantini M, Ghirotto L, Valzania F. Parkinson’s disease patients’ needs during the COVID-19 pandemic in a red zone: a framework analysis of open-ended survey questions. Eur J Neurol, 2021; 28(10):3254–62; doi:10.1111/ene.14745. CrossRef
Chinna K, Sundarasen S, Khoshaim HB, Kamaludin K, Nurunnabi M, Baloch GM, Hossain SFA, Sukayt A, Dalina N, Rajagopalan U, Kumar R, Memon Z. Psychological impact of COVID-19 and lock down measures: an online cross-sectional multicounty study on Asian university students. PLoS One, 2021; 16(8):e0253059; doi:10.1371/journal.pone.0253059. CrossRef
Chowdhury K, Etando A, Shahwan M, Škrbi? R, Jairoun AA, Haque M, Godman B. COVID-19 and the impact on the education of healthcare professionals across countries with a particular focus on developing countries. Bangladesh J Med Sci, 2022b; 21(1):221–32; doi:10.3329/bjms.v21i2.58053 CrossRef
Chowdhury K, Haque M, Lutfor AB, Siddiqui TH, Ahmad R, Sultana I, Sharma P, Lugova H, Etando A, Godman B. Impact of the COVID-19 pandemic on dental and medical education in Bangladesh: a pilot study and the implications. Bangladesh J Med Sci, 2022c; 21(1):444–54; doi:10.3329/bjms.v21i2.58080 CrossRef
Chowdhury K, Haque M, Nusrat N, Adnan N, Islam S, Lutfor AB, Begum D, Rabbany A, Karim E, Malek A, Jahan N, Akter J, Ashraf S, Hasan MN, Hassan M, Akhter N, Mazumder M, Sihan N, Naher N, Akter S, Zaman SU, Chowdhury T, Nesa J, Biswas S, Islam MD, Hossain AM, Rahman H, Biswas PK, Shaheen M, Chowdhury F, Kumar S, Kurdi A, Mustafa ZU, Schellack N, Gowere M, Meyer JC, Opanga S, Godman B. Management of children admitted to hospitals across Bangladesh with suspected or confirmed COVID-19 and the implications for the future: a nationwide cross-sectional study. Antibiotics (Basel), 2022a; 11(1):105; doi:10.3390/antibiotics11010105. CrossRef
Daud S, Hanafi WNW, Toolib SN, Rajadurai J. Employee well-being during COVID-19 in higher education institution in Malaysia: a case study. Int J Business Manag, 2020; 3(2):1–10.
Dhawan S. Online learning: a panacea in the time of COVID-19 crisis. J Educ Tech Syst, 2020; 49(1):5–22; doi:10.1177/0047239520934018 CrossRef
Etando A, Amu AA, Haque M, Schellack N, Kurdi A, Alrasheedy AA, Timoney A, Mwita JC, Rwegerera GM, Patrick O, Niba LL, Boahen-Boaten BB, Tabi FB, Amu OY, Acolatse J, Incoom R, Sefah IA, Guantai AN, Opanga S, Chikowe I, Khuluza F, Kibuule D, Kalemeera F, Hango E, Lates J, Fadare J, Ogunleye OO, Saleem Z, Oosthuizen F, Cordier W, Matlala M, Meyer JC, Schellack G, Massele A, Malande OO, Kalungia AC, Sichone J, Banda SS, Zaranyika T, Campbell S, Godman B. Challenges and innovations brought about by the COVID-19 pandemic regarding medical and pharmacy education especially in Africa and implications for the future. Healthcare (Basel), 2021; 9(12):1722; doi:10.3390/healthcare9121722. CrossRef
Gale NK, Heath G, Cameron E, Rashid S, Redwood S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med Res Methodol, 2013; 13:117; doi:10.1186/1471-2288-13-117. CrossRef
Girum T, Lentiro K, Geremew M, Migora B, Shewamare S, Shimbre MS. Optimal strategies for COVID-19 prevention from global evidence achieved through social distancing, stay at home, travel restriction and lockdown: a systematic review. Arch Public Health, 2021; 79(1):150; doi:10.1186/s13690-021-00663-8. CrossRef
Godman B, Egwuenu A, Haque M, Malande OO, Schellack N, Kumar S, Saleem Z, Sneddon J, Hoxha I, Islam S, Mwita J, do Nascimento RCRM, Dias Godói IP, Niba LL, Amu AA, Acolatse J, Incoom R, Sefah IA, Opanga S, Kurdi A, Chikowe I, Khuluza F, Kibuule D, Ogunleye OO, Olalekan A, Markovic-Pekovic V, Meyer JC, Alfadl A, Phuong TNT, Kalungia AC, Campbell S, Pisana A, Wale J, Seaton RA. Strategies to improve antimicrobial utilization with a special focus on developing countries. Life (Basel), 2021; 11(6):528; doi:10.3390/life11060528. CrossRef
Godman B, Haque M, Islam S, Iqbal S, Urmi UL, Kamal ZM, Shuvo SA, Rahman A, Kamal M, Haque M, Jahan I, Islam MZ, Hossain MM, Munzur-E-Murshid, Kumar S, Charan J, Bhatt R, Dutta S, Abhayanand JP, Sharma Y, Saleem Z, Phuong TNT, Kwon HY, Kurdi A, Wale J, Sefah I. Rapid assessment of price instability and paucity of medicines and protection for COVID-19 across Asia: findings and public health implications for the future. Front Public Health, 2020; 8:585832; doi:10.3389/fpubh.2020.585832. CrossRef
Goldsmith L. Using framework analysis in applied qualitative research. Qual Rep, 2021; 26(6):2061–76. CrossRef
Haider N, Osman AY, Gadzekpo A, Akipede GO, Asogun D, Ansumana R, Lessells RJ, Khan P, Hamid MMA, Yeboah-Manu D, Mboera L, Shayo EH, Mmbaga BT, Urassa M, Musoke D, Kapata N, Ferrand RA, Kapata PC, Stigler F, Czypionka T, Zumla A, Kock R, McCoy D. Lockdown measures in response to COVID-19 in nine sub-Saharan African countries. BMJ Glob Health, 2020; 5(10):e003319; doi:10.1136/bmjgh-2020-003319. CrossRef
Hanna E, Gough B. The social construction of male infertility: a qualitative questionnaire study of men with a male factor infertility diagnosis. Sociol Health Illn, 2020; 42(3):465–80; doi:10.1111/1467-9566.13038. CrossRef
Haque M, Rahman NAA, McKimm J, Binti Abdullah SL, Islam MZ, Zulkifli Z, Saidin NB, Azhar NIK, Binti Lutfi SNN, Binti Othman NSA. A cross-sectional study evaluating the knowledge and beliefs about, and the use of antibiotics amongst Malaysian university students. Expert Rev Anti Infect Ther, 2019; 17(4):275–84; doi:10.1080/14787210.2019.1581607. CrossRef
Hassali M. Role of community pharmacists in medication management: current and future prospects in Asia. J Acad Soc Qual Life, 2017; 3(3):1–18.
Heale R, Forbes D. Understanding triangulation in research. Evid Based Nurs, 2013; 16(4):98; doi:10.1136/eb-2013-101494. CrossRef
Hothersall SJ. Epistemology and social work: enhancing the integration of theory, practice and research through philosophical pragmatism. Eur J Soc Work, 2019; 22(5):860–70; doi:10.1080/13691457.2018.1499613 CrossRef
Ismail NS, Abu Bakar NM, Tarek Wafa SW. Online. learning challenges during pandemic COVID-19 in Malaysian Higher Learning Institution. Univers J Educ Res, 2020; 8(12):7151–9; doi:10.13189/ujer.2020.081282. CrossRef
Kaushik V, Walsh CA. Pragmatism as a research paradigm and its implications for social work research. Soc Sci, 2019; 8(9):255; doi:10.3390/socsci8090255. CrossRef
Kelly LM, Cordeiro M. Three principles of pragmatism for research on organizational processes. Methodol Innov, 2020; 13(2):2059799120937242; doi:10.1177/2059799120937242 CrossRef
Kumar S, Haque M, Shetty A, Acharya J, Kumar M, Sinha VK, Manohar B, Gowere M, Godman B. Current management of children with COVID-19 in hospitals in India; pilot study and findings. Adv Hum Biol, 2022; 12(1):16–21; doi:10.4103/aihb.aihb_162_21. CrossRef
Langford BJ, So M, Raybardhan S, Leung V, Soucy JR, Westwood D, Daneman N, MacFadden DR. Antibiotic prescribing in patients with COVID-19: rapid review and meta-analysis. Clin Microbiol Infect, 2021; 27(4):520–31; doi:10.1016/j.cmi.2020.12.018. CrossRef
Mohamad IN, Wong CK, Chew CC, Leong EL, Lee BH, Moh CK, Chenasammy K, Lim SC, Ker HB. The landscape of antibiotic usage among COVID-19 patients in the early phase of pandemic: a Malaysian national perspective. J Pharm Policy Pract, 2022; 15(1):4; doi:10.1186/s40545-022-00404-4. CrossRef
Mustafa Z. Coping with online lectures. 2020. Available via https://www.nst.com.my/education/2020/05/594096/coping-online-lectures (Accessed 11 March 2022).
Mustapha FI, Aagaard-Hansen J, Lim SC, Nasir NH, Aris T, Bjerre-Christensen U. Variations in the delivery of primary diabetes care in Malaysia: lessons to be learnt and potential for improvement. Health Serv Res Manag Epidemiol, 2020; 7:2333392820918744; doi:10.1177/2333392820918744. CrossRef
Nordin N, Nordin, N. Impact of pandemic COVID-19 to the online learning: case of higher education institution in Malaysia. Univers J Educ Res, 2020; 8(12A):7607–15; doi:10.13189/ujer.2020.082546 CrossRef
Nussbaumer-Streit B, Mayr V, Dobrescu AI, Chapman A, Persad E, Klerings I, Wagner G, Siebert U, Christof C, Zachariah C, Gartlehner G. Quarantine alone or in combination with other public health measures to control COVID-19: a rapid review. Cochrane Database Syst Rev, 2020; 4(4):CD013574; doi:10.1002/14651858.CD013574. CrossRef
Rahim FF, Abdulrahman SA, Kader Maideen SF, Rashid A. Prevalence and factors associated with prediabetes and diabetes in fishing communities in penang, Malaysia: a cross-sectional study. PLoS One, 2020; 15(2):e0228570; doi:10.1371/journal.pone.0228570. CrossRef
Rao S, Chowdhury N, Naithani M, Singh A, Singh N, Gupta AK, Kathrotia R. Alternative strategy adopted in practical assessment for pathology postgraduate certification examination amidst COVID-19 nationwide lockdown: an Indian experience with a novel hybrid method of assessment. Adv Med Educ Pract, 2021; 12:1. CrossRef
Sababathy M, Kalok AHM, Hafizz AMHA, Sharip S, Zainuddin ZM, Shafiee MN. Perception of medical students towards COVID-19 outbreak and movement control order (MCO) in Malaysia and impact on education. Res Square, 2021:1–13; doi:10.21203/rs.3.rs-646716/v1. CrossRef
Saddik B, Hussein A, Sharif-Askari FS, Kheder W, Temsah MH, Koutaich RA, Haddad ES, Al-Roub NM, Marhoon FA, Hamid Q, Halwani R. Increased levels of anxiety among medical and non-medical university students during the COVID-19 pandemic in the United Arab Emirates. Risk Manag Healthc Policy, 2020; 13:2395–406; doi:10.2147/RMHP.S273333. CrossRef
Safdar N, Abbo LM, Knobloch MJ, Seo SK. Research methods in healthcare epidemiology: survey and qualitative research. Infect Control Hosp Epidemiol, 2016; 37(11):1272–7; doi:10.1017/ice.2016.171. CrossRef
Saraswathi I, Saikarthik J, Senthil Kumar K, Madhan Srinivasan K, Ardhanaari M, Gunapriya R. Impact of COVID-19 outbreak on the mental health status of undergraduate medical students in a COVID-19 treating medical college: a prospective longitudinal study. PeerJ, 2020; 8:e10164; doi:10.7717/peerj.10164. CrossRef
Sazlina SG, Sooryanarayana R, Ho BK, Omar MA, Krishnapillai AD, Mohd Tohit N, Inche Zainal Abidin S, Ariaratnam S, Ahmad NA. Cardiovascular disease risk factors among older people: Data from the National Health and Morbidity Survey 2015. PLoS One, 2020; 15(10):e0240826; doi:10.1371/journal.pone.0240826. CrossRef
Shah AUM, Safri SNA, Thevadas R, Noordin NK, Rahman AA, Sekawi Z, Ideris A, Sultan MTH. COVID-19 outbreak in Malaysia: actions taken by the Malaysian government. Int J Infect Dis, 2020; 97:108–16; doi:10.1016/j.ijid.2020.05.093. CrossRef
Sharma P, Chowdhury K, Kumar S, Bhatt R, Hirani T, Duseja S, Haque M, Lutfor AB, Etando A, Škrbi? R, Shahwan M, Jairoun AA, Godman B. A pilot study regarding the consequence of the COVID-19 pandemic on Healthcare Education in India and the implications. Adv Hum Biol, 2022; 12:180–9; doi:10.4103/aihb.aihb_34_22 CrossRef
Shawaqfeh MS, Al Bekairy AM, Al-Azayzih A, Alkatheri AA, Qandil AM, Obaidat AA, Al Harbi S, Muflih SM. Pharmacy students perceptions of their distance online learning experience during the COVID-19 pandemic: a cross-sectional survey study. J Med Educ Curric Dev, 2020; 7:2382120520963039; doi:10.1177/2382120520963039. CrossRef
Shehata MH, Abouzeid E, Wasfy NF, Abdelaziz A, Wells RL, Ahmed SA. Medical education adaptations post COVID-19: an Egyptian reflection. J Med Educ Curric Dev, 2020; 7:2382120520951819; doi:10.1177/2382120520951819. CrossRef
Sundarasen S, Chinna K, Kamaludin K, Nurunnabi M, Baloch GM, Khoshaim HB, Hossain SFA, Sukayt A. Psychological impact of COVID-19 and lockdown among university students in Malaysia: implications and policy recommendations. Int J Environ Res Public Health, 2020; 17(17):6206; doi:10.3390/ijerph17176206. CrossRef
Talic S, Shah S, Wild H, Gasevic D, Maharaj A, Ademi Z, Li X, Xu W, Mesa-Eguiagaray I, Rostron J, Theodoratou E, Zhang X, Motee A, Liew D, Ilic D. Effectiveness of public health measures in reducing the incidence of COVID-19, SARS-CoV-2 transmission, and COVID-19 mortality: systematic review and meta-analysis. BMJ, 2021; 375:e068302; doi:10.1136/bmj-2021-068302.
Tiong TW, Chua SS. Knowledge and attitude of university students on antibiotics: a cross-sectional study in Malaysia. Drug Healthc Patient Saf, 2020; 12:135–44; doi:10.2147/DHPS.S253301. CrossRef
Tuckett AG, Stewart DE. Collecting qualitative data: part I: journal as a method: experience, rationale, and limitations. Contemp Nurs, 2003; 16(1–2):104–13; doi:10.5172/conu.16.1-2.104. CrossRef
Tuckett AG, Stewart DE. Collecting qualitative data: Part II. Group discussion as a method: experience, rationale, and limitations [corrected]. Contemp Nurs, 2004; 16(3):240–51; doi:10.5172/conu.16.3.240. CrossRef
Umair S, Waqas U, Faheem M. COVID-19 pandemic: stringent measures of Malaysia and implications for other countries. Postgrad Med J, 2021; 97(1144):130–2; doi:10.1136/postgradmedj-2020-138079. CrossRef
Wong YC, Mohan M, Pau A. Dental students’ compliance with antibiotic prescribing guidelines for dental infections in children. J Indian Soc Pedod Prev Dent, 2016; 34(4):348–53; doi:10.4103/0970-4388.191415. CrossRef
Xiang L, Tang M, Yin Z, Zheng M, Lu S. The COVID-19 pandemic and economic growth: theory and simulation. Front Public Health, 2021; 9:741525; doi:10.3389/fpubh.2021.741525. CrossRef
You HW, Tajuddin NSA, Anwar YAS. Measuring availability, prices, S and affordability of ischaemic heart disease medicines in Bangi, Selangor, Malaysia. Malays J Med Sci, 2019; 26(5):113–21; doi:10.21315/mjms2019.26.5.10. CrossRef