INTRODUCTION
According the International Diabetes Federation (IDF) diabetes atlas, the global estimate of diabetes prevalence in the year 2000 was 151 million, which now shows an alarming increase tripling to 463 million in 2019 (IDF Diabetes Atlas, 2019). A steep rise in the incidence of diabetes in the last 20 years clearly shows the need for preventive strategies across the globe, especially in the prediabetes stage where there is chance for reversal to normoglycemia. The attitude of the physician towards prediabetes management is the key factor in the early detection of diabetes. Moreover, the diagnostic criteria and treatment modalities of prediabetes differ in various guidelines, indicating the need for a uniform effective management protocol (Bansal, 2015), since diabetes is a highly prevalent disease where patients consult various general practitioners as first approach before specialist consultation. So, it is the need of the hour to enhance the prediabetes awareness among all primary care physicians. Hippocrates suggested that doctors may influence patient’s health and effective doctor–patient communication can be a source of motivation, reassurance, and support. According to the American Diabetes Association, prediabetic subjects should be referred to an intensive behavioral counseling program to improve lifestyle before starting pharmacological therapy. But most patients with prediabetes do not receive evidence-based treatment from healthcare providers, especially specific counseling and referral for lifestyle modification (Tseng et al., 2017). According to John Hopkins researchers, most primary care doctors could not identify all of the risk factors for prediabetes. The American Medical Association has focused its efforts toward educating physicians to screen and refer individuals with prediabetes to CDC-recognized lifestyle change programs.
METHODS
A detailed search on PubMed, Science Direct, Research Gate, and Scopus was carried out using the keywords prediabetes, questionnaire survey, physician awareness, diabetes prevention programs, prediabetes awareness, prediabetes knowledge attitude, and practices. The search was limited to full-text English articles on physicians’ prediabetes awareness. The reference lists of original studies and narrative reviews were also searched manually. All the publications on prediabetes awareness and practice among physicians carried out for the last 13 years, from 2008 to 2021, was considered for literature review and relevant research articles among them were included in the preparation of this review (Fig. 1). This review aims to exhibit the current status of prediabetes awareness among different specialities of physicians worldwide and highlights the importance of increasing primary care providers’ knowledge especially general practitioners and family physicians who deal first with this high-risk population (Table 1).
Prediabetes awareness among Southeastern European physicians
Southeastern European physicians of different categories, like general practitioners, non-endocrine specialists, endocrinologists, diabetologists and residents from different fields coming under the age group of 26–65 years, were included in a questionnaire survey to extract the awareness about prediabetes. Physicians from southeastern European countries like Croatia, Slovenia, Macedonia, Serbia, Montenegro, Bosnia, and Herzegovina with a work experience between 0.10 and 40 years were the participants. The questionnaire comprised 11 questions on the characteristics, features, and diagnostic parameters of prediabetes. The questionnaire was given to 500 physicians, among which 397 completed the survey. Endocrinologists and diabetologists exhibited more awareness on prediabetes compared to general practitioners and non-endocrine specialists, like cardiologists, neurologists, and surgeons. Moreover, junior physicians had more knowledge on the diagnostic values than seniors who did not follow the current guidelines considerably (Kokic et al., 2017). General practitioners and non-endocrine specialists play a vital role in screening and identifying patients at high risk for developing diabetes. The knowledge variation among the different categories of physicians was found due to insufficient education during the undergraduate medical education. So, these data show an urgent need for awareness raising and active education through workshops, conferences, and seminars on prediabetes among all medical professionals.
Prediabetes awareness and practice among Indian physicians
India is among the top four countries with prediabetes and diabetes according to the 2021 statistics of the International Diabetes Federation, but the awareness on prediabetes among the Indian population was found to be low (Hyder et al., 2021). One cross-sectional survey using a questionnaire was found, which assessed the KAP among physicians dealing with prediabetes in Kolar, Karnataka, India. The prevalidated questionnaire was administered directly to the physicians and general practitioners. For physicians from distant places, the questionnaire and consent form was send through email. The questionnaire consisted of 24 questions regarding various aspects of prediabetes management. The questionnaire consisted of three sections. The first part dealt with demographics of participants, while second part on knowledge and attitude among subjects. Part 3 addressed the daily routine practice related to detection and early management of prediabetes. 150 questionnaires were distributed, among which 120 filled questionnaires were received which included 14 MBBS primary care physicians, 46 MD qualified doctors on general medicine, 48 general medicine specialized postgraduates, and 14 specialists. The demographic details of the participants were not revealed in the data published. All the practitioners who participated were aware of prediabetes, but majority were actively involved in sieving out the population having prediabetes. Only specialized doctors took this condition as a serious step by detecting and providing advices on lifestyle modifications and preventive pharmacotherapy early (Basavareddy et al., 2015). The barriers to effective management of prediabetes were found to be delayed diagnosis, general practitioners lack of screening practice, and lack of patient adherence to lifestyle modification. Physicians should incorporate their gained knowledge into practice, diagnose the high-risk population early, and treat them at the prediabetes stage before they fall into irreversible diabetes.
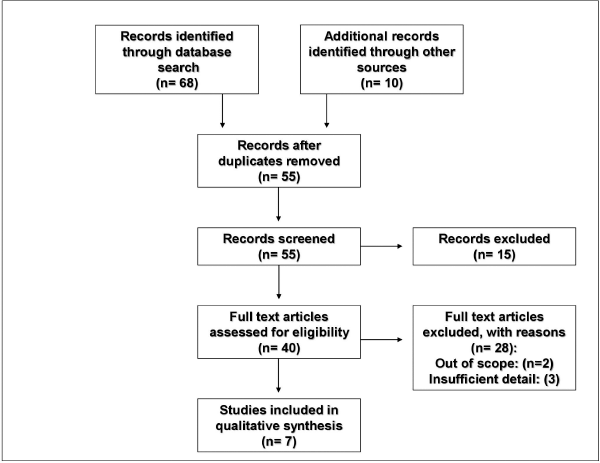 | Figure 1. Flowchart for the selection of articles [Click here to view] |
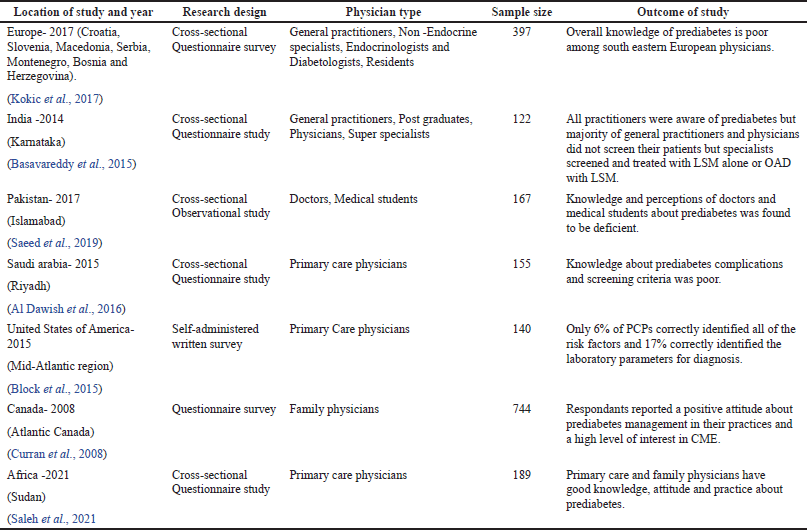 | Table 1. Physician prediabetes awareness surveys and their outcomes. [Click here to view] |
Knowledge and perceptions about prediabetes among Pakistani physicians
As per the latest statistics of the International Diabetes Federation Diabetes Atlas, 10th edition, Pakistan came third among the top three countries with diabetes. A clinic-based cross-sectional observational questionnaire survey was captured from Islamabad city of Pakistan during the year 2017. Physicians from departments of internal medicine, gastroenterology, neurology, and emergency and intensive care unit, with a mean age of 27.8+ 5.1 years, were the respondents. 46 were male and 39 were female, with a mean work experience after MBBS of 3.9 ± 4.1 years. Direct administration of the questionnaire was done in which senior medical students were selected as interviewers after getting proper training on prediabetes. The questionnaire contained questions on screening, diagnosis, risk factors, determinants of risk reduction, and interventions on prediabetes. The questionnaire was administered to 100 doctors, among which 85 were completed and returned. Respondents’ category involved physicians, house officers, fellowship trainees, medical officers, consultants, and specialists. The study results found important deficiencies among doctors regarding various aspects of prediabetes and its management. Although doctors followed the American Diabetes Association guidelines in their treatment decisions, results showed some contrasts in their approach to evidence-based therapy. The study could not find a positive correlation between correct identification of biochemical parameters to specialization and experience in the field; very few knew the proper directions to start biguanides as per the current guidelines (Saeed et al., 2019). The deficiency of prediabetes awareness among some of the physicians was assumed to be due to the gaps in the undergraduate medical curriculum and lack of continuous medical education for physicians on updated worldwide guidelines on prediabetes.
Awareness among primary care physicians in Saudi Arabia
The World Health Organization (WHO) has reported that Saudi Arabia ranks the second highest in the Middle East, and is seventh in the world for the rate of diabetes (Al Dawish et al., 2016). We found a cross-sectional study which assessed the knowledge of primary care physicians about the management, complications, screening criteria, screening age, and diagnostic criteria of prediabetes in Riyadh, Saudi Arabia. The study was conducted in primary healthcare centers of Riyadh through the multistage random sampling technique which included both general practitioners and family physicians. In the first stage, Riyadh city was divided into five regions, namely east, west, south, north, and middle. In the second stage, a list of primary healthcare centers from each region was constructed and among that biggest seven centers were sorted out. In the third stage, all the physicians of the chosen center were enrolled into the study. All the participants were asked to fill a predesigned self-administered questionnaire that was already pretested. 155 primary care physicians were enrolled in the study, among which 153 returned the questionnaire; 64 were male and 89 were female, with 30 Primary Care Physicians (PCP)s having a work experience below 5 years, 62 PCPs with 5–10, and 61 PCPs with above 10 years of experience. The results showed that primary care physicians in Riyadh had a good level of awareness about prediabetes but lacked knowledge on topics like screening criteria and complications of prediabetes. Physicians’ knowledge about the definition and laboratory values of prediabetes was found to be good. In this study, no significant association was found between the years of experience and the knowledge on prediabetes. The results also revealed that female physicians’ knowledge was higher than male physicians (Jammah et al., 2019). The study concluded by focusing on both undergraduate and postgraduate medical education curricula to increase the awareness among primary care physicians.
Knowledge and perceptions of primary care physicians on prediabetes in the USA
According to the American Diabetes Association and IDF statistics of 2021, USA stands fourth in position with 32.2 million diabetes and 96 million prediabetes cases. A large number of prediabetes awareness surveys and research have been conducted in USA compared to other countries in the world. A cross-sectional email survey was extracted which assessed primary care physicians’ knowledge, attitude, and practice on prediabetes. Respondents were 298 general practitioners working in America from American Medical Association (AMA) Masterfile. The study population included family physicians, general practitioners, and general interns who finished their training. Majority of the participants were above 50 years and in practice for around 20 years among which 96 were female. The survey evaluated domains like practice behaviors regarding prediabetes management, awareness on lab parameters, risk factors, existing barriers, and possible interventions and recommendations. Substantial gaps in primary care physicians’ knowledge on various parameters on prediabetes were detected. Only 36% of the physicians referred prediabetes to diabetes prevention lifestyle modification as their initial management program. The other 43% opted to start biguanides for prediabetes management. Only 15% of the doctors had the knowledge on all risk factors of prediabetes, while others gave wrong options. Doctors always preferred biguanides as soon they detect nonadherence or nonresponse to lifestyle modification. Lack of motivation, failure of prior lifestyle program, and stress were found to be the potential barriers in prediabetes management. Lack of awareness on risk factors and biochemical parameters among doctors lead to inadequate checkup among high-risk individuals in the USA (Tseng et al., 2019). There was also inadequate knowledge on weight loss programs and its impact among American physicians (Garay et al., 2019). A survey conducted among the academic family medicine clinic physicians showed a moderate knowledge on prediabetes parameters but limited awareness on diabetes prevention programs (Keck et al., 2019). Two-thirds of the adults were overweight or obese in the United States of America, so weight loss programs as well as behavioral intervention roles in diabetes prevention is inevitable (Block et al., 2015).
Primary care physicians’ knowledge and awareness on prediabetes across Atlantic Canada
According to Diabetes Canada, almost six million Canadians have prediabetes. A questionnaire-survey was searched out among the family physicians across Atlantic Canada. A total of 2,320 questionnaires were mailed to the study population during the year 2008 and 744 emails were received. Among the respondents, 395 were male and as equal 342 were female, and majority had above 10 years of work experience. Topics included in the survey were detection and management of prediabetes, attitude among prediabetes, and continuing medical education interventions. Participants showed a positive attitude toward prediabetes management and willingness in continuing medical education in areas like diagnosis, pharmacological, and nonpharmacological treatment of prediabetes. Prediabetes biochemical parameters like impaired fasting glucose and impaired glucose tolerance values were found to be confused by some respondents during the email survey. Physicians also showed more eagerness in acquiring knowledge on weight loss strategies and physical activity in diabetes prevention among prediabetes. Respondents reported lack of motivation and busy work schedules as a hindrance in implementing lifestyle modification in their daily routine. Physicians who handled more prediabetes patients in their daily practice strongly agreed that it is challenging to detect and manage this condition early (Curran et al., 2008).
Prediabetes knowledge, attitude, and practice among primary care physicians in Sudan
Nigeria, located on the western coast of Africa, comes under the top 10 countries with the highest impaired tolerance cases all over the world. Ethiopia, another country of Africa, is also predicted to see a rise the cases and will be top listed by the year 2045. A cross-sectional questionnaire survey was carried out among primary care providers working in primary healthcare centers in localities of Karary and Khartoum, Sudan. The questionnaires were given to 200 general physicians, out of which 189 filled and completed the study. Among the respondents, 79% were female, median age of the respondents were 34 years, and median duration of work experience was 7 years. The topics included in the questionnaire were patient demographics, attitude, knowledge, practices, and potential barriers to prediabetes management. Among the total respondents, 60% showed acceptable knowledge, positive attitude, and good practices. Completing courses and clinical training on prediabetes revealed statistically significant improvement in prediabetes awareness. The identified hurdles for prediabetes prevention included lack of motivation, awareness on prediabetes, and lack of time for follow-up (Saleh et al., 2021).
CONCLUSION
Identifying the high-risk population having prediabetes, which is an asymptomatic condition, is a real challenge in modern Diabetology along with the prospect of trying to change the lifestyle habits of those from different cultures and genetic makeup (Edwards et al., 2016). We need to develop a national registry of patients who have prediabetes similar to the other diseases and need to have a thorough follow-up of these patients at least annually (Tuso, 2014). There is a requirement of systematic evaluation of the health outcomes of prediabetes and benefits, if any, with its early management (Bansal, 2015). Awareness of prediabetes, which was found to be low among primary care doctors than specialists, needs to be raised and uniform guidelines for its management needs to be developed (Wylie et al., 2002).
ACKNOWLEDGEMENT
The authors express their gratitude to JSS College of Pharmacy, Ooty, and JSS Academy of Higher Education and Research, Mysuru, for providing various facilities used during the project. The authors thank the staff and healthcare professionals of Govt. Medical College and Hospital, Ooty, for supporting the project.
CONFLICT OF INTEREST
There are no conflicts of interest.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
FUNDING
There is no funding to report.
CONFLICTS OF INTEREST
The authors report no financial or any other conflicts of interest in this work.
ETHICAL APPROVALS
This study does not involve experiments on animals or human subjects.
DATA AVAILABILITY
All data generated and analyzed are included within this research article.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Al Dawish MA, Robert AA, Braham R, Al Hayek AA, Al Saeed A, Ahmed RA, Al Sabaan FS. Diabetes mellitus in Saudi Arabia: a review of the recent literature. Curr Diabetes Rev, 2016; 12(4):359–68. CrossRef
Bansal N. Prediabetes diagnosis and treatment: a review. World J Diabetes, 2015; 6(2):296–303. CrossRef
Block G, Azar KM, Romanelli RJ, Block TJ, Hopkins D, Carpenter HA, Dolginsky MS, Hudes ML, Palaniappan LP, Block CH. Diabetes prevention and weight loss with a fully automated behavioral intervention by email, web, and mobile phone: a randomized controlled trial among persons with prediabetes. J Med Internet Res, 2015; 17(10):e240. CrossRef
Basavareddy A, Dass AS, Narayana S. Prediabetes awareness and practice among Indian doctors—a cross-sectional study. J Clin Diagn Res, 2015; 9(8):FC01–3. CrossRef
Curran VR, Hollett MA, Allen MD, Steeves J, Dunbar P. A continuing medical education needs assessment of primary care physicians knowledge and awareness of prediabetes care. Can J Diab, 2008; 32(4):273–80. CrossRef
Edwards CM, Cusi K. Prediabetes: a worldwide epidemic. Endocrinol Metab Clin North Am, 2016; 45(4):751–64. CrossRef
Garay J, Camacho PA, Lopez-Lopez J, Alvernia J, Garcia M, Cohen DD, Calderon C, Lopez -Jaramillo P. Survey of knowledge for diagnosing and managing prediabetes in Latin-America: cross-sectional study. Diabetol Metab Syndr, 2019; 11:102. CrossRef
Hyder KM, Mohan J, Varma V, Ponnusankar S, Raja D. Impact of prediabetes education program on knowledge, attitude and practice among prediabetic population of south India. Prev Med Rep, 2021; 23:101395. CrossRef
International Diabetes Federation. IDF diabetes atlas, 9th edition, International Diabetes Federation, Brussels, Belgium, 2019. Available via https://www.diabetesatlas.org
Jammah AA, Alateeg EA, AlShalawi HA, Alsafi AM, AlGhamlas RE, Alzahrani SH. Awareness of prediabetes stage among primary care physicians in Riyadh. Indo Am J Pharm Sci, 2019; 06(02):3651–8.
Keck JW, Thomas AR, Hieronymus L, Roper KL. Prediabetes knowledge, attitudes, and practices at an Academic Family Medicine practice. J Am Board Fam Med, 2019; 32(4):505–12. CrossRef
Kokic V, Kokic S, Krnic M, Petric M, Liberati AM, Simac P, Milenkovic T, Capkun V, Rahelic D, Blaslov K. Prediabetes awareness among Southeastern European physicians. J Diabetes Investig, 2017; 9(3):544–8. CrossRef
Saeed N, Jaffery T, Ansari FA, Hamid B, Khan BA. Knowledge and perceptions about Pre-diabetes amongst doctors, medical students, and patients in a tertiary care hospital of Islamabad. J Pak Med Assoc, 2019; 69(4):527–32.
Saleh AM, Almobarak AO, Badi S, Siddiq SB, Tahir H, Suliman M, Ahmed MH. Knowledge, attitudes and practice among primary care physicians in Sudan regarding prediabetes: a cross-sectional survey. Int J Prev Med, 2021; 12:80.
Tseng E, Greer RC, O’Rourke P, Yeh HC, McGuire MM, Clark JM, Maruthur NM. Survey of primary care providers’ knowledge of screening for diagnosing and managing prediabetes. J Gen Intern Med, 2017; 32(11):1172–8. CrossRef
Tseng E, Greer RC, O’Rourke P, Yeh HC, McGuire MM, Albright AL, Marsteller JA, Clark JM, Maruthur NM. National survey of primary care physicians’ knowledge, practices, and perceptions of prediabetes. J Gen Intern Med, 2019; 34(11):2475–81. CrossRef
Tuso P. Prediabetes and lifestyle modification: time to prevent a preventable disease. Perm J, 2014; 18(3):88–93. CrossRef
Wylie G, Hungin AP, Neely J. Impaired glucose tolerance: qualitative and quantitative study of general practitioner’s knowledge and perceptions. BMJ, 2002; 324:1190–5. CrossRef