INTRODUCTION
Rare diseases are illnesses that cause a great deal of misery for people and have a large impact on society. Although the number of individuals suffering from a specific rare disease is small, there is an unending list of rare diseases that exist in the world, given that only a small number of them are recognized and many more are yet undiscovered. Due to their low prevalence, there is a dearth of knowledge about the diseases as well as the paucity of information available about their treatment, and their hazardous, persistent nature has led to rare diseases, which is an emerging health issue in the world. The majority of rare diseases have a hereditary cause, and just a handful have effective therapies. Any patient suffering from a rare condition must deal with a variety of issues as diagnosing the disease effectively is difficult, and treating it is no less difficult and uncertain. Treatment of any rare disease may cause financial constraints to the patient’s family especially if it is self-funded (Cai et al., 2021; Nguengang Wakap et al., 2020).
An activating mutation of activin A receptor, type I/activin-like kinase-2 (ACVR1/ALK2), a bone morphogenetic protein type I receptor, causes Fibrodysplasia Ossificans Progressiva (FOP), a rare autosomal dominant disorder of progressive heterotopic ossification (HO), in all classically affected individuals worldwide (Gupta et al., 2018). FOP is an exceedingly unusual illness with a worldwide frequency of one case in every 2 million people. As a result, people with FOP are more likely to be misdiagnosed and/or underdiagnosed (She et al., 2020). FOP is characterized by ”flare-ups” in numerous soft tissues in multiple body areas such as the hips, knees, back, head, and shoulder that can last several days or even weeks, as well as fever, inflammation, and movement restrictions. These complications make it impossible for the patient to live a regular life. Patients may find it difficult to eat, drink, speak, or even breathe in the worst-case situation (Peng et al., 2019). Patients are usually affected by this condition throughout their infancy or adolescence, and with a typical lifetime of 50 years, only a small percentage of patients live to be 60. By the age of 30, most patients are confined to a wheelchair (Gupta et al., 2018). The different symptoms linked with the ailment decrease quality of life, making it even worse and necessitating substantial studies to learn more about this health issue (Kaplan et al., 2018). There is presently no cure, but a 4-week course of higher-dose corticosteroids given during the initial 24 hours of a “flare-up” may help out to lessen the acute soreness and tissue edema seen in the initial phases of the disorder. Numerous clinical trials are now ongoing, based on promising pre-clinical efficacy findings in FOP animal models (Pignolo et al., 2020). A literature review was undertaken to determine the epidemiology of FOP and its influence on the quality of life of patients.
MATERIALS AND METHODS
Literature search
A literature search was performed in the databases like EMBASE and PubMed from inception to 30 December 2021. The keywords used in the search were those referring to (FOP, Stone man syndrome, HO, Myositis ossificans Progressiva) and health-related quality of life (HRQoL, Quality, Pain, functional disability) as well as Depression (Emotional health, depressive, depressed), etc. and preliminarily identified studies of our interest. Then, a few studies were identified from a gray literature search in Google Scholar. Duplicity check was done and duplicate papers were removed. Once the deduplication was done, 112 studies were left which were involved in the title abstract screening. A total of 86 papers were retrieved and qualified for full-text screening based on the information in the abstract, following which 17 studies were included and relevant data were gathered.
Inclusion and exclusion criteria
Studies that mentioned epidemiology of FOP as well as the association between FOP and HRQoL in children and adults were included in this review. For studies related to epidemiology that provided data related to incidence, the prevalence of FOP throughout the world was included. Studies related to HRQoL papers were included where information regarding patient-reported outcomes (PROs) and various scales for measurement of QoL like Patient-Reported Outcomes Measurement Information System (PROMIS), 36-Item Short Form Survey (SF-36), 12-Item Short Form Health Survey, etc. were mentioned in detail. Cross-sectional, case-control, and appropriate waves of longitudinal studies were included.
Non-English studies were excluded. Studies from which extraction of data was not possible particularly related to FOP populations, such as subgroup data for FOP individuals, were not included. There were no inclusion restrictions on countries, interventions, as well as study designs. Paid articles and non-open access articles were not included.
Study selection procedure
Before selection, all papers were anonymized. This was done by taking out information like the “title,” “author(s),” “year of publication,” and “journal name.” Two independent reviewers carried out the selection of relevant studies, and for any conflicts, the third reviewer reviewed the papers and resolved the conflicts. A Preferred Reporting Items for Systematic Reviews and Meta-Analyses diagram of the study selection procedure is given in Figure 1.
Data extraction and quality evaluation
From each article, the following details were extracted: “Last name of first author,” “country,” “year of publication,” “journal name,” “sample size,” “gender,” “scales used to evaluate quality of life,” pain measurement, “incidence,” “prevalence,” and depression measurement. Microsoft Excel was used to record all of the data in a uniform way. Using descriptive statistics, the results were presented in the form of tables.
RESULTS AND DISCUSSION
Study design and population
Of the 17 studies included, nine studies reported the humanistic burden associated with FOP, and the remaining seven studies were identified reporting the prevalence of FOP. The prevalence of FOP ranged from 0.04 to 1.36 per million population. A higher prevalence of FOP was found in the USA (0.88 per million) and Europe (0.47–1.36 per million) compared to the Asian (0.11 per million) population. The mean age of diagnosis of FOP ranged from 3 months to 15 years. Eight studies reported the humanistic burden associated with FOP. PROMIS and SF-36 were the most commonly used instruments in FOP to assess the humanistic burden. During flare-ups of FOP, moderate to severe pain (on a scale of 0–10) was prevalent in 56%–67% of patients and 45%–74% of these patients also reported anxiety, depression, or irritability, according to the PROMIS scale. Assessed on the SF-36 scale, the physical dimension was the most affected. The most representative items were impaired function and physical role.
Humanistic burden measurements
A total of six different instruments were used in the nine studies, of which five were generic instruments and two were disease-specific. The most frequently used instruments were the PROMIS and the SF-36 as part of the Medical Outcomes Study. Of the four studies where the PROMIS scale was used, one study saw a combination of PROMIS with FOP disease-specific instruments FOP-Specific Physical Function Questionnaire (FOP-PFQ) and Cumulative Analog Joint Involvement Scale (CAJIS) for FOP Bone. In three studies, the generic instrument PROMIS was used alone similarly, another generic instrument SF-36 was used alone to measure the humanistic burden. In one study, SF-36 was used in combination with the Health Assessment Questionnaire and Barthel Index to estimate the relation of deterioration in “activities of daily living (ADL)” functioning with a decrease in “quality of life” in physical function domains. In one study, disease-specific instruments FOP-PFQ and CAJIS were used to measure the HRQoL of FOP populations. A list of HRQoL instruments and PROs used in eligible studies is mentioned in Table 1. All of the studies included in this review reported on additional psychological and social dimensions, such as social support and personality structure, in addition to HRQoL, but these instruments were outside the scope of this study.
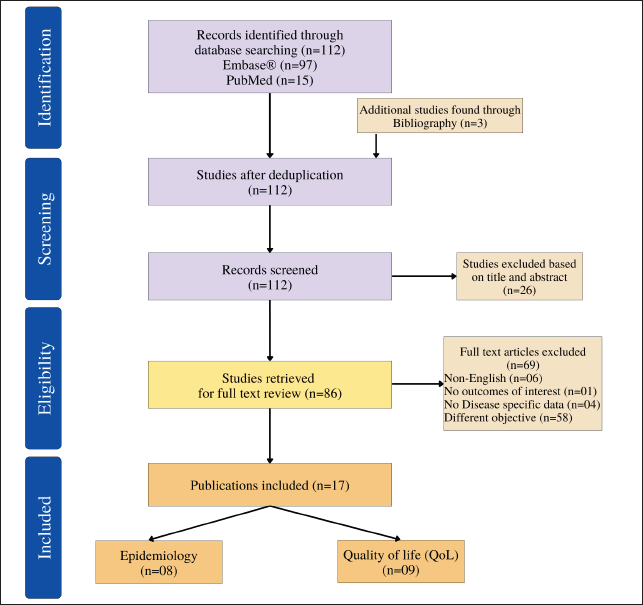 | Figure 1. Flowchart showing study selection process. [Click here to view] |
Quality of life impairment in FOP
The findings of different studies revealed that HO, or the appearance of bone in “soft tissue” where bone normally does not occur, has been discovered to be a key indicator of FOP (Peng et al., 2019; Pignolo et al., 2020). A recent study showed that Painful “soft tissue swellings or flare-ups” typically accompany HO, which can linger for months. For many people, a flare-up can signal a worsening of their disease and lead to emotions of fear or repressed effect, both of which have been shown to enhance pain perception (Peng et al., 2019). Individuals reported HO with reduced mobility in the neck, upper back, lower back, right shoulder, and left shoulder the most frequently, with 53.59%, 50.5%, 45.9%, 44.29%, and 45.39% of all participants reporting the restriction, respectively. The same locations were also the most common sites for HO, which causes complete immobility. Younger persons are less likely to have HO with partial or total loss of movement in regions affecting the lower limbs (e.g., hips, knees, ankles) or the mouth (15 years) (Pignolo et al., 2020). In one study, participants in the high pain group (N = 7) reported changed emotional functioning in domains such as “anxiety” in association with physical symptoms, namely “physical stress,” according to clinical questionnaire data obtained from FOP patients. In addition to the quantity of “physical stress” experienced (r = 0.65, p = 0.009), the severity of pain was significantly linked with the magnitude of “self-reported depressive symptoms” (r = 0.74, p = 0.0016). Significant links were also discovered between patients’ levels of anxiety, the sensory component of pain, and physical stress, indicating that these three domains interact in FOP (Peng et al., 2021).
In a recent survey conducted in 15 countries, 463 people responded to the survey (patients: 219; family members: 244). Patients with diminished joint function reported lower quality of life and a greater dependency on living accommodations. Almost half of the main caregivers reported that their psychological or physical health had been mild to moderately impacted. The majority of patients and primary caregivers (aged 18) claimed that FOP affected their choice of careers (Al Mukaddam et al., 2022).
The PROMIS global health scale was employed in another investigation to measure quality-of-life impairment. The overall “PROMIS Global Health Scale” scores were calculated, with a maximum probable score of 35 for age groups 0–9 years old and 9–15 years old based on 7 questions, and a maximum probable score of 55 for age groups >15 years old based on 10 questions. A higher score indicates a higher quality of life. For the age categories 0–9 years, 9–15 years, and >15 years, the mean total scores were 25.4, 26.6, and 32, respectively. The absolute mean total score for the youngest age groups was lower than for the >15 years old group since the total scores were based on maximum possible scores of 35 and 55, respectively (Pignolo et al., 2020).
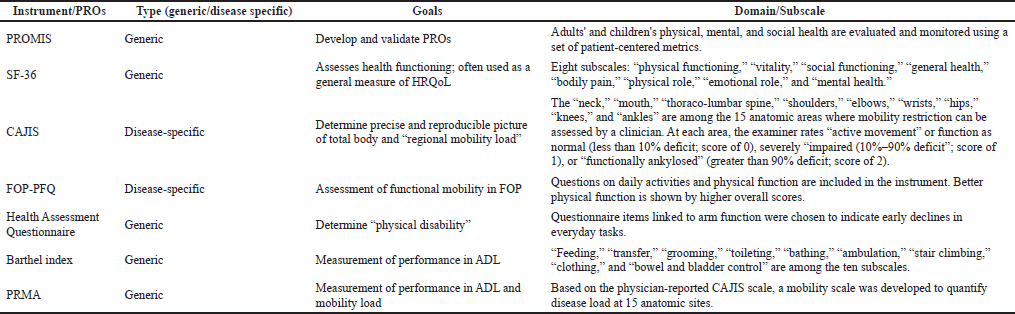 | Table 1. HRQoL instruments and PROs used in included studies. [Click here to view] |
In a longitudinal patient-reported mobility assessment (PRMA) analysis, it was found that between the first and follow-up PRMAs, 45/64 patients (70%) reported an overall deterioration of mobility, whereas 9/64 patients (14%) reported no change and 10/64 patients (16%) indicated an interval improvement. The axial area had the largest self-reported deterioration in mobility and the smallest “self-reported improvement” in mobility, while the lower limbs had the least “self-reported worsening” and biggest “self-reported improvement” in mobility. In general, nearly 40% of patients reported no differences in mobility between axial, upper limb, and lower limb locations. Around 40% of patients reported no differences in mobility across the axial, upper limb, and lower limb locations. Within 6 months following the second PRMA, 21/64 patients (33%) had a “physician-reported CAJIS” examination, with no history of intervening “flare-ups” or reported worsening of their illness (Kaplan et al., 2018). Besides this, in another study, it was observed that a sample of 57 participants (N = 57) had baseline and 12-month evaluations, with mean changes of 0.40 units for the CAJIS and 3.0% for the FOP-PFQ. The CAJIS and FOP-PFQ had a strong correlation (p = 0.70, p < 0.0001), showing that patient ratings of “functional impairment” are linked to “physician-assessed functional disability” (Kaplan et al., 2017).
According to a longitudinal investigation of the FOP group, items about arm function on the Barthel Index and the Health Assessment Questionnaire likely reflect early decreases in everyday activities. Decreases in the “quality of life” in physical function areas were closely associated with declines in the functioning of “ADL.” “ADL” and “quality of life” remained constant with baseline levels during the duration of the experiment (Barthel Index: p = 0.42; MOS SF-36: p = 0.43; Health Assessment Questionnaire: p = 0.87) (Nakahara et al., 2019). In a transverse observational study, the SF-36 was used to examine individuals with FOP. The physical component was shown to be the most impacted, with an average of 25.5 points. Impaired function and physical role were the most representative items. With an average of 44.5 points, physical discomfort was discovered. With an average of 79 and 76, the top results were obtained in the categories of “emotional role” and mental health, respectively (Ortiz-Agapito and Colmenares-Bonilla, 2015). A global survey was conducted involving patients who were members of the International FOP Association. It was found that when compared to the general population, the prevalence of neuropathic pain (NP) was substantially higher (p < 0.001) in females (15%) than in males (1.6%). Other sensory abnormalities were identified by 94% of patients with NP. The incidence of recurrent severe headaches (26%) was equal to that of the general population, whereas females with FOP (36%) had approximately four times the frequency of males. During FOP flare-ups, 23% of people experienced worsening neurological symptoms. Myoclonus was reported by three FOP patients (1.8%), a substantially higher rate than in the overall group (p < 0.001) (Kitterman et al., 2012) (Table 2).
Epidemiology of FOP worldwide
The prevalence of FOP ranged from 0.04 to 1.36 per million population (Baujat et al., 2017; Pignolo et al., 2021). As a result of the “natural history” of FOP, affected people become increasingly debilitated as they age due to progressive HO. Although HO is a one-time occurrence in FOP, the disability it causes is cumulative (Kannu and Levy, 2021). Eating and oral hygiene can be substantially hampered in situations of severe impairment, having a significant influence on the quality of life. Up to 50% of persons with FOP have hearing loss, which is generally conductive (Kannu and Levy, 2021; Kitterman et al., 2012; Mantick et al., 2018). Due to “soft-tissue” and “joint ossification” and the resultant loss of range of motion, most persons with FOP will experience a gradual “loss of ambulation.” Many people will rely on wheeled mobility to go around their homes and communities (Kannu and Levy, 2021). The median age at death is 42 years old, with a typical life expectancy of 56 years (Kannu and Levy, 2021). Hearing loss usually begins in childhood and develops over time. NP and recurring headaches are common neurologic symptoms in FOP patients, especially in post-pubertal females. Immobilization, insufficient dietary fiber, excess animal protein intake, and deficient hydration all raise the incidence of renal stones in people with FOP, which is around three-fold higher than in the general population. Swallowing difficulty, anorexia, stomach discomfort, gastroesophageal reflux, nausea, occasional vomiting, trouble digesting meals, pressure ulcers, and constipation are among the gastrointestinal symptoms experienced by persons with FOP (Kannu and Levy, 2021; Kitterman et al., 2012; Mantick et al., 2018). The prevalence of FOP in the USA is estimated to be 0.88 per million people (Baujat et al., 2017). Besides this, the estimated prevalence of registered and confirmed FOP patients ranged from 0.65 per million in North America and 0.47 per million in Western Europe to 0.27 per million in Latin America, 0.05 per million in Africa, and roughly 0.04 per million in Asia–Pacific (Pignolo et al., 2021). The incidence of FOP in Europe ranges from 0.47 to 1.36 per million (Baujat et al., 2017). A higher prevalence of FOP was found in the USA (0.88 per million) and Europe (0.47 to 1.36 per million) compared to the Asian (0.11 per million) population (Baujat et al., 2017; Pignolo et al., 2021). The mean age of diagnosis of FOP ranged from 3 months to 15 years (Morales-Piga et al., 2012). Typical congenital abnormalities of the great toes are classic/defining FOP traits. Other common FOP characteristics include thumb malformations which is a kind of congenital deformity. Cervical spine orthotopic fusions, knee osteochondromas, femoral necks that are either short or too wide, and hearing loss caused by conductive noise are other characteristics (Morales-Piga et al., 2012). FOP patients with “ACVR1R206H” mutations have a higher frequency of cardiac conduction abnormalities on electrocardiogram, according to research (Kou et al., 2020). FOP affects an estimated 3,500–4,000 persons globally, while the condition has only been identified in roughly 900 people. Although there are no authorized therapies for FOP at this time, early detection and diagnosis are critical to avoid needless stress, such as intramuscular immunization or surgery, which can cause illness flares (Kannu and Levy, 2021). The findings of a study revealed that Brazil now has the third-largest community of FOP sufferers, with 89 people (45 men and 50 women) identified and recorded in the FOP Brazil dataset. According to the FOP Brazil dataset, the southern states of Brazil account for the majority of the country’s identified FOP patients (67.4%), followed by the northeast states (22.5%), the central states (6.7%), and the northern states (3.30%) (Zorzi et al., 2022).
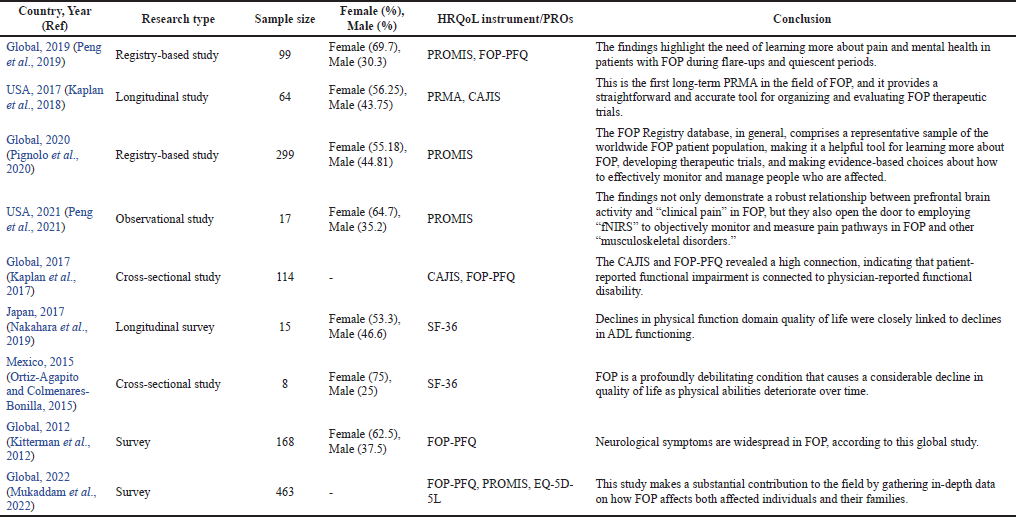 | Table 2. Summary of eligible and reviewed studies on FOP and HRQoL impairment. [Click here to view] |
LIMITATIONS
When assessing the data gathered and presented in this study, the following limitations must be kept in mind. There are currently no reliable techniques or clinical biomarkers that can be utilized to identify and track flare-ups in FOP patients. It might be more practical and reliable to ascertain whether and how pain, emotional health, and related health variables correlate with flare-up events in FOP if such approaches were available.
CONCLUSION
Published evidence assessing the epidemiology of FOP and the humanistic burden was sparse to draw meaningful conclusions. Variability in the prevalence of FOP was reported across geographies. This variability can be attributed due to a lack of awareness of FOP among the medical fraternity and a delay in correct diagnosis. Very little is understood about the mechanism(s) behind pain in FOP, either during or between flare-up occurrences, which can make it challenging to effectively administer analgesia to FOP patients. Numerous analgesic treatments with variable efficacy across modalities have been and are often used in FOP to date.
In FOP, a considerable decline in quality of life was found as a result of increasing deterioration in physical capacities, underscoring the need for effective therapeutics in this overlooked illness area. Analyzing the FOP Registry has provided a variety of fresh insights into the dynamics of flare-up, pain, emotional and mental health, physical health, and overall quality of life. There is a need to work on the development of effective treatments for FOP considering the effect of FOP on the HRQoL.
AUTHOR CONTRIBUTIONS
All authors participated in writing the article or its critical revision for important intellectual content. They all made significant contributions to its idea and design, data collection, analysis, and interpretation of content with significant intellectual value; consent to submit to the current provided final clearance for the version to be published in the journal; and accept responsibility for all facets of the work. Every author meets the requirements/guidelines for medical journal editors recommended by International Committee of Medical Journal Editors.
FINANCIAL SUPPORT
There is no funding that can be reported.
CONFLICT OF INTEREST
The authors have no funding or any other conflict of interest in this work.
ETHICAL APPROVAL
This study does not involve experiments on animal or human subjects.
DATA AVAILABILITY
All data presented in this review article were generated and analyzed for this study.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Al Mukaddam M, Toder KS, Davis M, Cali A, Liljesthröm M, Hollywood S, Croskery K, Grandoulier AS, Böing EA, Whalen JD, Kaplan FS. The impact of fibrodysplasia ossificans progressiva (FOP) on patients and their family members: results from an international burden of illness survey. Expert Rev Pharmacoecon Outcomes Res, 2022:1–15.
Baujat G, Choquet R, Bouée S, Jeanbat V, Courouve L, Ruel A, Michot C, Le Quan Sang KH, Lapidus D, Messiaen C, Landais P, Cormier-Daire V. Prevalence of fibrodysplasia ossificans progressiva (FOP) in France: an estimate based on a record linkage of two national databases. Orphanet J Rare Dis, 2017; 12(1):1–9. CrossRef
Cai X, Genchev GZ, He P, Lu H, Yu G. Demographics, in-hospital analysis, and prevalence of 33 rare diseases with effective treatment in Shanghai. Orphanet J Rare diseases, 2021; 16(1):1–1. CrossRef
Gupta RR, Delai PL, Glaser DL, Rocke DM, Al Mukaddam M, Pignolo RJ, Kaplan FS. Prevalence and risk factors for kidney stones in fibrodysplasia ossificans progressiva. Bone, 2018; 109:120–3. CrossRef
Kannu P, Levy CE. Improving the diagnosis of fibrodysplasia ossificans progressiva. J Pediatr, 2021; 232:S3–8. CrossRef
Kaplan FS, Al Mukaddam M, Pignolo RJ. Longitudinal patient-reported mobility assessment in fibrodysplasia ossificans progressiva (FOP). Bone, 2018; 109:158–61. CrossRef
Kaplan FS, Hsiao EC, Baujat G, Brown MA, De Cunto C, Di Rocco M, Keen R, Al Mukaddam M, Grogan DR, Pignolo RJ. Assessment tools of physical and functional disability in fibrodysplasia ossificans progressiva. J Bone Miner Res, 2017; 32(1):S391.
Kitterman JA, Strober JB, Kan L, Rocke DM, Cali A, Peeper J, Snow J, Delai PL, Morhart R, Pignolo RJ, Shore EM, Kaplan FS. Neurological symptoms in individuals with fibrodysplasia ossificans progressiva. J Neurol, 2012; 259(12):2636–43. CrossRef
Kou S, De Cunto C, Baujat G, Wentworth KL, Grogan DR, Brown MA, Di Rocco M, Keen R, Al Mukaddam M, le Quan Sang KH, Masharani U, Kaplan FS, Pignolo RJ, Hsiao EC. Patients with ACVR1 R206H mutations have an increased prevalence of cardiac conduction abnormalities on electrocardiogram in a natural history study of fibrodysplasia ossificans progressiva. Orphanet J Rare Dis, 2020; 15(1):1–0. CrossRef
Mantick N, Bachman E, Baujat G, Brown M, Collins O, De Cunto C, Delai P, Eekhoff M, Zum Felde R, Grogan DR, Haga N, Hsiao E, Kantanie S, Kaplan F, Keen R, Milosevic J, Morhart R, Pignolo R, Qian X, di Rocco M, Scott C, Sherman A, Wallace M, Williams N, Zhang K, Bogard B. The FOP connection registry: design of an international patient-sponsored registry for fibrodysplasia ossificans progressiva. Bone, 2018; 109:285–90. CrossRef
Morales-Piga A, Bachiller-Corral J, Trujillo-Tiebas MJ, Villaverde-Hueso A, Gamir-Gamir ML, Alonso-Ferreira V, Vázquez-Díaz M, de la Paz MP, Ayuso-García C. Fibrodysplasia ossificans progressiva in Spain: epidemiological, clinical, and genetic aspects. Bone, 2012; 51(4):748–55. CrossRef
Nakahara Y, Kitoh H, Nakashima Y, Toguchida J, Haga N. Longitudinal study of the activities of daily living and quality of life in Japanese patients with fibrodysplasia ossificans progressiva. Disabil Rehabil, 2019; 41(6):699–704. CrossRef
Nguengang Wakap S, Lambert DM, Olry A, Rodwell C, Gueydan C, Lanneau V, Murphy D, Le Cam Y, Rath A. Estimating cumulative point prevalence of rare diseases: analysis of the orphanet database. Eur J Hum Genet, 2020; 28(2):165–73. CrossRef
Ortiz-Agapito F, Colmenares-Bonilla D. Quality of life of patients with fibrodysplasia ossificans progressiva. J Child Orthop, 2015; 9(6):489–93. CrossRef
Peng K, Cheung K, Lee A, Sieberg C, Borsook D, Upadhyay J. Longitudinal evaluation of pain, flare-up, and emotional health in fibrodysplasia ossificans progressiva: analyses of the international FOP registry. JBMR Plus, 2019; 3(8):e10181. CrossRef
Peng K, Karunakaran KD, Labadie R, Veliu M, Cheung C, Lee A, Yu PB, Upadhyay J. Suppressed prefrontal cortex oscillations associate with clinical pain in fibrodysplasia ossificans progressiva. Orphanet J Rare Dis, 2021; 16(1):1–3. CrossRef
Pignolo RJ, Cheung K, Kile S, Fitzpatrick MA, De Cunto C, Al Mukaddam M, Hsiao EC, Baujat G, Delai P, Eekhoff EM, Di Rocco M, Grunwald Z, Haga N, Keen R, Levi B, Morhart R, Scott C, Sherman A, Zhang K, Kaplan FS. Self-reported baseline phenotypes from the international fibrodysplasia ossificans progressiva (FOP) association global registry. Bone, 2020; 134:115274. CrossRef
Pignolo RJ, Hsiao EC, Baujat G, Lapidus D, Sherman A, Kaplan FS. Prevalence of fibrodysplasia ossificans progressiva (FOP) in the United States: estimate from three treatment centers and a patient organization. Orphanet J Rare Dis, 2021; 16(1):1–8. CrossRef
She D, Li R, Fang P, Zong G, Xue Y, Zhang K. Serum osteocalcin level is associated with the mortality in Chinese patients with fibrodysplasia ossificans progressiva aged≤ 18 years at diagnosis. BMC Musculoskelet Disord, 2020; 21(1):1–8. CrossRef
Zorzi AR, Delai PR, Rosa HL, Brito WE, Montalli VA, Napimoga JC, Napimoga MH, Nociti FH. Fibrodysplasia ossificans progressiva in Brazil: challenges and strategies to create assistance and educational networks. Orphanet J Rare Dis, 2022; 17(1):1–4. CrossRef