INTRODUCTION
According to the Ministry of Health of the Republic of Indonesia, the population of older people in Indonesia has increased from 18 million people (7.56%) in 2010 to 25.9 million (9.7%) in 2019, and it is expected to continue expanding to 48.2 million people (15.77%) in 2035 (Biro Komunikasi dan Pelayanan Masyarakat, 2019). Older people are usually divided into two groups by age: 65–84 years (young-old) and >84 years old and older (elders). Moreover, they often have functional disorders associated with chronic diseases or aging. In geriatric medicine, it is important to protect organ systems as well as to maintain physical functions because organ functioning in older people is vulnerable to a variety of diseases (Tristanto, 2020). One of the most essential organs is the eye. It has the function of observing or seeing and showing facial expressions (Kaur, 2017). The absence of an eyeball inside the orbital cavity is clinically defined as socket anophthalmia, more commonly referred to as anophthalmos or anophthalmia (Dewi & Lyrawati, 2011). Socket anophthalmia can occur for a variety of reasons, including congenital defects, irreversible damage, tumors, a blind painful eye, the requirement for histological confirmation of a suspected illness, the avoidance of sympathetic ophthalmia, and cosmetic problems (related to the appearances). There are three forms of surgical therapy, depending on the severity of the situation: exenteration, evisceration, and enucleation (Choubisa, 2016; Jamayet et al., 2017).
Socket contracture (SC) is a common symptom of socket anophthalmia. In this condition, the socket is unable to support the prosthesis. This makes it difficult or impossible to connect the prosthesis to the socket, presenting aesthetic issues for those who are affected. The SC categorization is critical for determining the best prosthesis and reconstructive procedures. Only slight siltation of the fornix is obtained, but the prosthesis can still be connected. The silting of the fornix will get broader and heavier as the degree of SC increases. The fornix can be completely lost in the most severe cases (Dewi and Lyrawati, 2011).
Patients who have had their ocular structures eviscerated or enucleated can get an ocular prosthesis (Choubisa, 2016). Ready-made ocular prosthesis (stock eyes) and custom-made ocular prostheses (custom-made) are also options (Gunaseelaraj et al., 2012; Kaur, 2017). When there are time limits and financial considerations, patients might be given a stock eye. However, there are several disadvantages, including not fitting (less comfortable), infection due to the difference in size between the eyeball and the socket, which causes a water bag, which is a breeding ground for bacteria, and improper color matching (iris color discrepancy) causing aesthetic issues (Gunaseelaraj et al., 2012), as in the McBain et al. (2014) study, which explained that patients had artificial eyes installed due to psychological factors rather than clinical or demographic factors.
A custom-made ocular prosthesis is designed to improve adaptability, eyeball movement, and iris position that is similar to or identical to the natural eye. Custom-made ocular prostheses have the disadvantage of a long laboratory production time. The problem is that laboratory methods take time to create prostheses. An ocular prosthesis is often recommended following surgical evisceration and enucleation. Patients with allergies to acrylic materials or a lack of retention in their eye sockets are prohibited.
Case Report
The patient in this case had been blind since she was a kid due to the infectious disease varicella zoster (chickenpox). Low economic and educational levels, as well as poor environmental sanitation, were also contributing causes. Enucleation surgery was performed at the age of 10 years. Ophthalmic shingles is caused by the zoster varicella virus, which infects the ganglion section of the gasseri, which receives nerve (NV) fibers from the ophthalmic branch of the trigeminus NV and is characterized by unilateral herpetic eruptions on the face and around the eyes. If it reaches the eyes, it might cause major issues (Himayani and Haryant, 2017).
An Ocular prosthesis was made after enucleation surgery, and the patient has been using them for 62 years (Fig. 1). Due to financial difficulties, the prosthesis has never been compensated. Because it was often detached, the previous ocular prosthesis had become uncomfortable to wear. It was a challenging task to treat a 72-year-old patient who required rapid treatment with an appealing and comfortable ocular prosthesis outcome.
The informed consent was provided by the Prosthodontics Specialist Universitas Airlangga, Dental Hospital, and given to the patient. The patient agreed to the informed consent, the examination, and the publication of the case.
RESULT AND DISCUSSION
The initial visit was used to examine the patient’s condition and get informed permission. Secondly, an objective examination was performed, which contained minor SC, no irritation, tumors, or infection, and eyelid muscles that can open and close (Fig. 2). Due to a serious infection, the patient’s bulbus oculi dextra had been lost. The treatment strategy entailed employing the hollow custom-built eye prosthesis process to create a customized eye prosthesis made of an acrylic resin material.
 | Figure 1. Patient profiles are front-facing with old eye prosthesis (A) and old front-facing prosthesis (B). [Click here to view] |
The following visit involved doing asepsis of the work area prior to printing. Special printing spoons and hydrocolloid (alginate) irreversible printing ingredients were used in the printing procedure. The printing material was slightly diluted and applied evenly to all parts of the eye socket with an injection syringe. Then, the printing spoon was gently inserted into the printed material, and the patient was instructed to grind the eye to the right, left, top, and bottom and finally close the eyes before the printed material hardens. As a result, the surface of the eye socket’s base would be properly printed. The patient was then told to open her eyes when the printed material had hardened, and the printed material was gently removed from the eye socket. As a result, a negative print of the patient’s eye socket was obtained.
Planting was done in a type III gypsum cast after getting the printing. After the gypsum had cured, the center was sliced off to remove the printing spoon, resulting in a printout that fits the patient’s eye socket. The printing was then filled with modeling wax to create a sclera wax pattern. After that, the wax design is cleaned up and smoothed. (Fig. 3).
The scleral wax pattern was then tested on the patient by elevating the upper eyelid and inserting the upper edge of the scleral wax pattern, followed by the lower eyelid and the lower margin of the night pattern. The scleral night pattern should be comfortable and fit the size and natural curve of the eyeball to avoid discomfort. We examined the movement of the eyelids as they opened and closed. After that, the focus point of the iris was recorded, the diameter of the iris was measured, and the color of the sclera and iris was determined in accordance with a normal eye (Fig. 4).
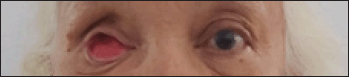 | Figure 2. Front view patient profile with contracture socket. [Click here to view] |
 | Figure 3. The result of the pattern of dental modeling wax sclera that has been smoothed. [Click here to view] |
The night sclera pattern was planted into gypsum type II in order to get the blueprint used for the sketch. Then, it was continued with the application of acrylic self-cure material (Stellon) no. 4. The finished sclera pattern was then perforated to place a predetermined iris diameter. Then, in the fourth visit, the patient tried the eye scoket by paying attention to the shape, color, comfortability, and position of the iris (Fig. 5). The next step was to coat the scleral pattern with a thin layer of wax and remove the wax and give it a color like blood vessels, followed by clear acrylic packing. After smoothing the clear acrylic layer, the pupil and iris were stained using oil paint according to the condition of the patient’s eye color. Then, the posterior part of the prosthesis is covered using self-cure acrylic and polished to a glossy finish (Fig. 6).
The next treatment was the insertion of the eye prosthesis (Fig. 7). Prior to implantation, checking the cleanliness of the prosthesis, eye socket, and the operator’s and patient’s hands was needed. Then, the eye prosthesis was cleaned using soap under running water. The insertion procedure must consider the aesthetics, retention, stability, and comfort of the eye prosthesis. The patient was then educated on how to remove and maintain the prosthesis. The first control was performed one day after the insertion, and the second control was performed one week later, and the patient did not complain and adjusted well.
Functional impairment is common in the elderly as a result of chronic illness or aging. It is important to protect organ systems and maintain physical functions in order to sustain independence, such as daily living functions, cognitive function, emotion, and sociality (family, friends, and work) (Arai et al., 2012) because losing an eye is a terrible occurrence in a person’s life.
A common problem with anophthalmic sockets is SC. In this condition, the socket cannot hold the prosthesis. This makes it difficult or impossible to attach the prosthesis to the socket, causing cosmetic problems for the patient (Quaranta-Leoni et al., 2021). At mild degrees only siltation is obtained on the fornic, but the prosthesis can still be attached.
Ocular prostheses can be available as stock eyes made or custom-made. In this case, the patient lost her eyeball as a toddler due to a viral disease and underwent enucleation surgery and has used eye prostheses for 62 years without replacement. The type of eye prosthesis that is made is a custom-made hollow eye prosthesis.
This custom-made ocular prosthesis improves flexibility, eyeball mobility, and precise iris alignment with the nearby natural eye. The problem is that the production of the prosthesis requires laboratory processing time (Waskitho et al., 2015). Furthermore, this custom-made prosthesis is created by reducing the inside of the sclera pattern, which is then closed with acrylic (Kavlekar et al., 2016; Maskey et al., 2019). The weight of the ocular prosthesis is greatly lowered, one-third lighter than its initial weight, and the prosthesis becomes light, comfortable, and visually pleasing because thick prostheses previously overburdened the lower eyelid, producing pain, irritation, discharge, and redness (Worrell, 2016). Maintaining the shape of damaged sockets avoids loss of eyelid shape, offers normal muscle action on the eyelids, prevents fluid buildup in the cavity, maintains palpebral apertures comparable to natural eyes, replicates natural eye color and proportions, and provides a gaze similar to natural eyes (Dhillon et al., 2020; Varamudy et al., 2014). The advantage of making eye prostheses is that it exerts a positive influence on the patient’s relationships and acceptance in society, thereby improving the quality of life (Goiato et al., 2018). However, the limitation of the study is that the report did not follow up on the prosthetic treatment till a few months later, and thus it cannot be evaluated for the duration of the eye prostheses.
 | Figure 4. Determining the focus and diameter of the iris and the color of the sclera. [Click here to view] |
 | Figure 5. Trying in sclera pattern in patients. [Click here to view] |
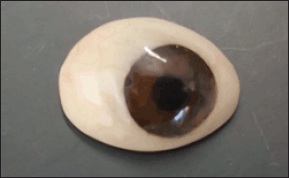 | Figure 6. Hollow custom-made eye prosthesis after smoothing. [Click here to view] |
 | Figure 7. Insertion of hollow custom-made eye prosthesis. [Click here to view] |
CONCLUSION
In conclusion, the placement of a custom prosthesis in an elderly patient was a success. With her new eye, the patient is at ease. Hollow custom-made prostheses made through accurate printing are retentive when the prosthesis is incised and also light, comfortable, and aesthetic for the users. As a result, the patient is not terrified of other people’s comments or interference. The goal of an eye prosthesis is to return the patient’s look to that of a normal eye, allowing the elderly to feel more accepted in society and enhance their quality of life. It is suggested that future studies examine the durability of the custom-made eye prostheses and see whether there is a side effect or not, such as if the patient is allergic to acrylic. Focusing on the psychosocial aspects of patients having prosthetic eyes is also recommended.
FUNDING
There is no funding to report.
CONFLICTS OF INTEREST
The authors declare there are no conflicts of interest.
AUTHOR CONTRIBUTIONS
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work. All the authors are eligible to be an author as per the international committee of medical journal editors (ICMJE) requirements/guidelines.
DATA AVAILABILITY
All data generated and analyzed are included within this research article.
DECLARATION OF PATIENT CONSENT
The authors certify that they have obtained all appropriate patient consent forms. The patient has/have given his/her consent for his/her images and other clinical information to be reported in the journal. The patients informed clearly that their names will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
PUBLISHER’S NOTE
This journal remains neutral with regard to jurisdictional claims in published institutional affiliation.
REFERENCES
Arai H, Ouchi Y, Yokode M, Ito H, Uematsu H, Eto F, Oshima S, Ota K, Saito Y, Sasaki H, Tsubota K, Fukuyama H, Honda Y, Iguchi A, Toba K, Hosoi , Kita T, and Members of Subcommittee for Aging. Toward the realization of a better aged society: messages from gerontology and geriatrics. Japan Geriatr Soc, 2012; 12(1):16–22; doi:10.1111/j.1447-0594.2011.00776.x CrossRef
Biro Komunikasi dan Pelayanan Masyarakat. Indonesia Masuki Periode Aging Population. Kementerian Kesehatan RI, 2019 (Accessed 7 June 2022).
Choubisa D. A simplified approach to rehabilitate an ocular defect: ocular prosthesis. J Indian Prosthodont Soc, 2016; 17(1):89–94; doi:10.4103/0972-4052.179260 CrossRef
Dewi DS, Lyrawati D. Soket Kontraktur Orbita: Definisi, Penyebab dan Klasifikasi. Jurnal Kedokteran Brawijaya, 2011; 26(4):185–90; doi:10.21776/ub.jkb.2011.026.04.12 CrossRef
Dhillon HK, Raj A, Dhasmana R, Bahadur H. Anophthalmic socket—a cosmetic dilemma. IP Int J Ocul Oncol Oculoplasty, 2020; 4(1):6–11; doi:18231/2455-8478.2018.0004 CrossRef
Goiato MC, de Caxias FP, dos Santos DM. Quality of life living with ocular prosthesis. Expert Rev Ophthalmol, 2018; 13(4):187–9; doi:10.1080/17469899.2018.1503534 CrossRef
Gunaseelaraj R, Karthikeyan S, Kumar MN, Balamurugan T, Jagadeeshwaran AR. Custom-made ocular prosthesis. J Pharm Bioallied Sci, 2012; 4(6):177; doi:10.4103/0975-7406.100264 CrossRef
Himayani R, Haryant IAP. Herpes Zoster Oftalmika dengan Blefarokonjungtivitis Okuli Sinistra. Jurnal Kesehatan Dan Agromedicine, 2017; 4(1):49–55.
Jamayet NB, Kirangi JK, Husein A, Alam MK. A comparative assessment of prosthetic outcome on enucleation and evisceration in three different etiological eye defects: a case series. Eur J Dent, 2017; 11(01):130–4; doi:10.4103/1305-7456.202636 CrossRef
Kaur J. Prosthetic rehabilitation of a patient with ocular defect—a case report. Dent J Adv Stud, 2017; 5(1):67–70. CrossRef
Kavlekar AA, Aras MA, Chitre V. A light weight ocular prosthesis fabricated by a simplified technique: an eye in a day. Int J Contemp Med Res, 2016; 3(6):1591–3.
Maskey B, Mathema SRB, Shrestha K, Bhochhibhoya A. A simplified approach to fabricate a hollow ocular prosthesis. J Prosthodon, 2019; 28(7):849–52; doi:10.1111/jopr.12757 CrossRef
McBain HB, Ezra DG, Rose GE, Newman SP. The psychosocial impact of living with an ocular prosthesis. Orbit, 2014; 33(1):39–44; doi:10.3109/01676830.2013.851251 CrossRef
Quaranta-Leoni FM, Fiorino MG, Quaranta-Leoni F, Di Marino M. Anophthalmic socket syndrome: prevalence, impact and management strategies. Clin Ophthalmol, 2021; 15:3267–81; doi:10.2147/OPTH.S325652 CrossRef
Tristanto A. Dukungan Kesehatan Jiwa dan Psikososial (DKJPS) dalam Pelayanan Sosial Lanjut Usia pada Masa Pandemi COVID-19. Sosio Informa, 2020; 6(2):205–22. CrossRef
Varamudy N, Raghavan R, Regish KM, Sharma D, Prithviraj DR, Divakar KP. Comparison of two techniques of rehabilitating ocular defect with custom made ocular prosthesis. JBR J Interdiscip Med Dent Sci, 2014; 02(04); doi:10.4172/2376-032X.1000135 CrossRef
Waskitho A, Sugiatno E, Ismiyati T. Protesa Mata: Rehabilitasi Pasien. Majalah Kedokteran Gigi Indonesia, 2015; 20(2):178; doi:10.22146/majkedgiind.7957 CrossRef
Worrell E. Hollow prosthetic eyes. Ophthalmic Plast Reconstr Surg, 2016; 32(6):e132–e5; doi:10.1097/IOP.0000000000000320 CrossRef